Walk into almost any clinic in 2026 and you’ll feel it: medicine is quietly but firmly shifting into a new gear. Diagnoses are faster, treatments are more targeted, and more and more people are living with conditions that, not long ago, would have defined or ended their lives. It doesn’t feel like science fiction anymore; it feels like opening the door to a very different kind of future.
At the same time, this new era is messy and uneven. Some breakthroughs are already saving lives, others are still trapped in clinical trials, and a few are probably overhyped. But taken together, they point toward something big: a world where healthcare is less about reacting to illness and more about predicting, preventing, and personalizing it. Let’s walk through what’s really changing – and what it could mean for your life in the next decade.
The Rise of Precision Medicine: One Size No Longer Fits All
Imagine walking into your doctor’s office and getting a treatment plan that’s built around your DNA, your lifestyle, and even your gut bacteria, instead of generic guidelines. That’s the promise of precision medicine, and it’s already reshaping cancer care and rare disease treatment. Rather than guessing which drug might work, doctors can increasingly match therapies to specific genetic mutations or molecular markers in your body.
In oncology, for example, targeted drugs and immunotherapies are chosen based on the exact profile of a tumor, not just where it sits in the body. This doesn’t mean cures for everyone, and many patients still face tough odds, but it does mean more people responding to therapy and fewer enduring brutal, ineffective treatments. Over the next decade, this approach will likely extend far beyond cancer – to heart disease, autoimmune conditions, mental health, and more – turning medicine from broad strokes into something closer to a custom-made suit.
Gene Editing Moves from the Lab to the Clinic

For years, gene editing felt like the medical equivalent of talking about flying cars: exciting, but not really part of daily life. That’s changing fast. Techniques like CRISPR-based editing have already been used in real patients to treat certain inherited blood disorders and eye diseases, with some people experiencing life-changing improvements after a single treatment. Regulators in several countries have started approving gene-editing therapies for specific conditions, marking a major turning point.
This doesn’t mean we’re editing embryos or casually designing “better” humans – that’s heavily restricted and ethically charged territory. Instead, most current progress is focused on fixing faulty genes in people already living with serious diseases, often when no other good options exist. These are still high-risk, high-cost interventions, and no one knows the full long-term effects yet. But if early results continue to hold up, it’s not unrealistic to think that certain genetic diseases could shift from life sentences to treatable, or even one-day curable, conditions.
AI and Robotics: The New Partners in the Exam Room
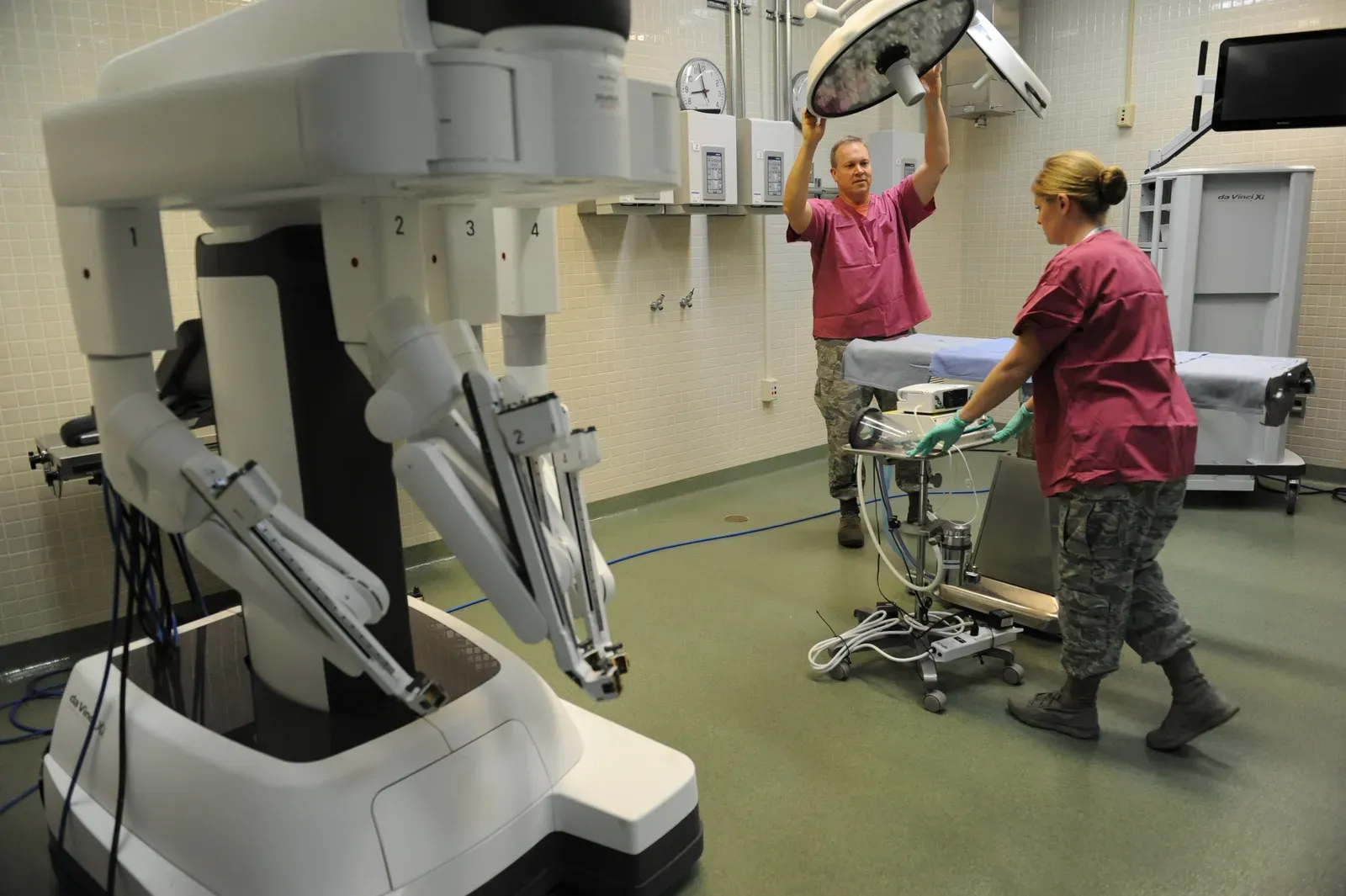
Artificial intelligence in healthcare used to sound like marketing jargon; now, it’s scanning real images, reading real charts, and suggesting real decisions. AI tools already help radiologists spot early signs of cancer in medical imaging, sometimes catching subtle patterns humans might miss when tired or rushed. In pathology labs, algorithms can analyze slides of tissue faster than any person, flagging suspicious areas for closer review and freeing up specialists for the hardest cases.
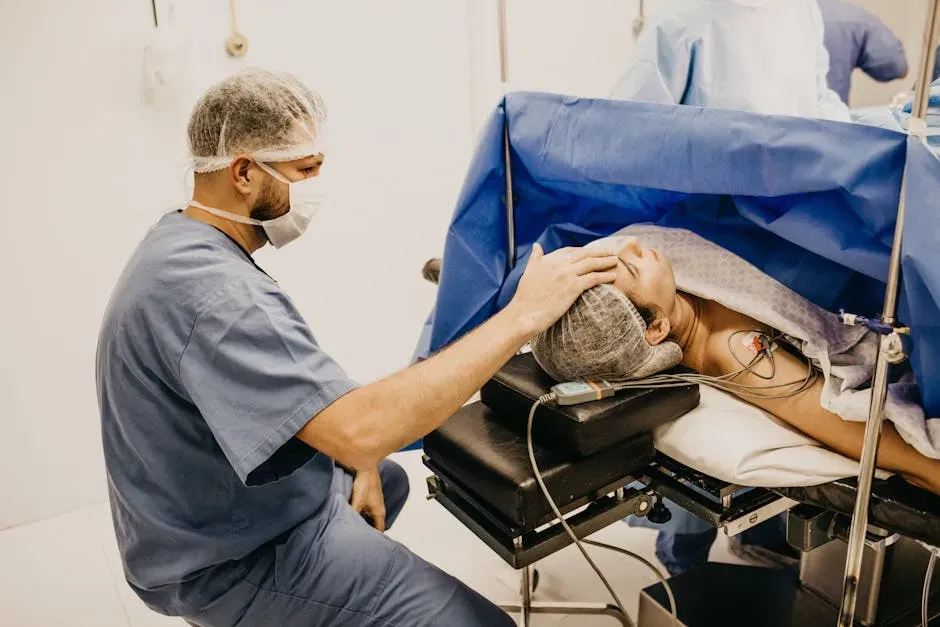
In operating rooms, robotic-assisted surgery has become increasingly common, with surgeons using precise instruments and 3D visualization systems to perform minimally invasive procedures. These systems don’t replace surgeons; they extend their capabilities. On the more experimental side, AI models are helping design new drugs, predict which patients are at highest risk of complications, and even generate draft clinical notes. The big question now isn’t whether AI will be used, but how to make sure it’s safe, fair, and transparent – and not just another black box making life-or-death calls.
mRNA and Next-Generation Vaccines Redefine Prevention
The COVID-19 pandemic stress-tested medicine in terrifying ways, but it also accelerated one of the most important vaccine breakthroughs in decades: mRNA technology. Once considered too delicate or theoretical for widespread use, mRNA vaccines went from concept to real-world deployment at record speed, and they’ve now protected hundreds of millions of people worldwide. The real story in 2026 is what comes after that emergency sprint.
Researchers are exploring mRNA vaccines against a range of threats: influenza, RSV, certain cancers, and even some autoimmune diseases. Because mRNA platforms can be updated relatively quickly, they offer a powerful tool against emerging pathogens and viral variants. We shouldn’t expect instant solutions to every disease – biology rarely cooperates that neatly – but there’s a strong chance that the next generation of vaccines will be faster to develop, easier to adapt, and more precisely targeted than anything we grew up with.
Regenerative Medicine: Repairing, Replacing, and Rebuilding
Regenerative medicine tries to do something radical: instead of just treating damage, it aims to help the body rebuild itself. Stem cell therapies, engineered tissues, and bio-printed organs are all part of this developing toolkit. We’re already seeing promising applications in conditions like certain blood cancers, where engineered immune cells (like CAR-T therapies) are used to hunt down and destroy malignant cells that once seemed unstoppable.
In other areas, researchers are working on lab-grown skin for burn victims, cartilage for damaged joints, and even early-stage organ models that may one day evolve into transplantable organs. It’s not a magic fix, and for every sensational headline, there are countless careful, incremental experiments happening quietly in the background. But the basic idea – that your body’s own cells, or engineered cells, can be used as medicine – is no longer a wild fantasy. It’s turning into a new branch of therapy that might one day make replacement parts for the human body feel almost routine.
Digital Health, Wearables, and the Shift to Continuous Care

For most of modern history, healthcare has been episodic: you get sick, you visit a doctor, then you go home and hope for the best. Wearables and digital health tools are starting to flip that script. Smartwatches and patches can now track heart rhythms, sleep patterns, blood oxygen levels, and even early signals of infections, giving a continuous stream of data instead of a single snapshot during a clinic visit. In some cases, they’ve already helped detect silent conditions like atrial fibrillation before they lead to strokes.
Beyond consumer gadgets, remote monitoring systems are helping doctors follow patients with chronic illnesses from a distance, adjusting medications more quickly and stepping in before a crisis hits. This could be a game changer for people living with diabetes, heart failure, lung disease, or high-risk pregnancies. Of course, there’s a real risk of data overload and burnout – for both patients and clinicians – but the direction is clear: health is becoming something we track every day, not just when something goes very wrong.
From Big Data to Better Decisions: The Power and Peril of Health Analytics

Hospitals, insurers, labs, and devices now generate enormous floods of data – far more than any human team could analyze on its own. Advanced analytics and machine learning tools are being thrown at these datasets to try to answer big questions: Which treatment really works best for which people? What early signs predict who is likely to end up in an ICU next month? Which hospital practices quietly save lives, and which just waste resources?
When used thoughtfully, these insights can reshape care guidelines, improve hospital safety, and personalize risk predictions. But there’s a darker side lurking: poorly designed models can amplify biases, misinterpret messy real-world data, or push decisions that look efficient on paper but harmful in practice. We’re learning that more data isn’t automatically better; it’s only as useful as the questions we ask and the guardrails we build. The real breakthrough here may not be the technology itself, but our willingness to use it with humility and oversight.
Longevity Science and the Slow Rethink of Aging

Aging used to be treated like a background setting – inevitable, unchangeable, and not really the focus of medicine except when something broke. Now, researchers are increasingly treating aging itself as a risk factor that can be studied, slowed, and maybe one day modified in targeted ways. Experiments in animals have shown that certain drug classes, metabolic tweaks, and cellular “cleanup” mechanisms can extend healthy lifespan, and some of these approaches are starting to be cautiously explored in humans.
We’re nowhere near an immortality pill, and anyone promising that is selling a fantasy. But there is a reasonable hope that future medicine can extend the healthy, functional part of life, pushing back frailty, cognitive decline, and chronic disease by a few or maybe several years. Even modest gains here could transform society: think of grandparents who can play with their great-grandkids without pain, or workers staying sharp and engaged in their seventies. The hard part will be making sure any longevity advances are safe, evidence-based, and not just the privilege of a tiny wealthy slice of the world.
Mental Health Breakthroughs: Brains Finally Get Equal Attention

For decades, mental health lagged behind the rest of medicine, weighed down by stigma and underfunding. That’s beginning to shift. New imaging techniques, digital tools, and more precise diagnostic approaches are helping us understand conditions like depression, anxiety, PTSD, and schizophrenia as brain-based and body-linked, not moral failings or personal weaknesses. This change alone is huge – it opens the door to better treatment, better funding, and more open conversations.
On the treatment front, research into psychedelic-assisted therapies, rapid-acting antidepressants, neuromodulation devices, and tailored psychotherapy approaches is moving quickly, though not without controversy. Early trials suggest that, for some people who have failed multiple treatments, these new approaches can offer relief where traditional options fell short. At the same time, the rise of mental health apps and remote therapy has made support more reachable for many, even as quality and regulation struggle to keep up. In this new era of breakthroughs, the brain is finally being treated as central to health, not an afterthought.
Ethics, Access, and the Risk of a Two-Tier Future
Every new medical breakthrough comes with a hard question baked in: who gets it, and who gets left behind? Many of the therapies making headlines – gene editing, cell therapies, advanced cancer drugs – currently come with breathtaking price tags. Even in wealthy countries, insurers and public systems are wrestling with how to pay for them, and in lower-income regions, they may be completely out of reach. The danger is painfully clear: a future where the healthiest people are not just the luckiest, but the wealthiest.
There’s also the issue of consent, privacy, and control. When your DNA, brain scans, or years of wearable data sit on servers somewhere, who owns that information, and how can it be used? The next phase of medical progress isn’t just a scientific project; it’s a political and moral one. Getting this right will demand public debate, smart regulation, and a willingness to say no to certain uses of powerful tools, even when they are technically possible. The promise of this new era will only be fully realized if it lifts many, not just a select few.
Conclusion: Choosing the Future We Want for Our Health
Standing in 2026, it’s tempting to see these breakthroughs as an unstoppable wave of progress, but nothing about the future of health is guaranteed. The science is racing ahead, but how it actually lands in our lives depends on countless choices we make as patients, voters, professionals, and communities. We can push for care that’s more personal, more preventive, and more humane – or we can drift into a world where dazzling technology coexists with widening gaps in who gets to benefit.
In the end, the new era of medical breakthroughs isn’t just about better machines or smarter drugs; it’s about redefining what it means to live well, age well, and care for one another. These advances carry enormous hope, but they also hand us responsibility: to ask hard questions, demand solid evidence, and keep human dignity at the center of every shiny innovation. When you imagine your own future health, which of these possibilities feels most important to fight for – and which ones would you be willing to say no to, even if they were possible?