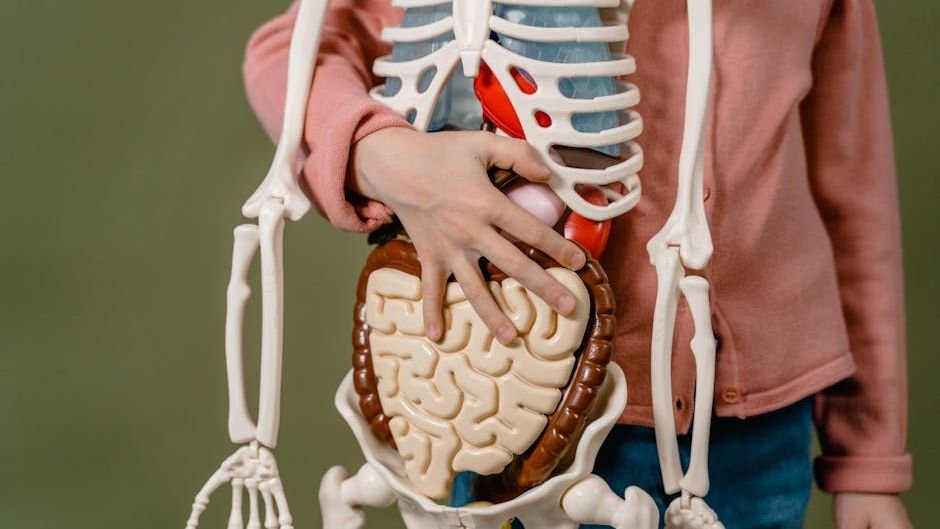
If someone told you that a few pounds of microscopic organisms are quietly steering your mood, your cravings, and even parts of your immune system, you might laugh it off. But that is exactly what is happening inside your gut every day. You are carrying around a bustling inner ecosystem that acts so intelligently and independently that scientists often call it your “second brain.”
Once you start to see your gut as a living city instead of just a food tube, a lot of things begin to make sense: why some days you feel mentally sharp and energized and other days foggy and irritable, why stress can send you running to the bathroom, and why what you eat can shape how you feel far beyond your stomach. Understanding your microbiome does not mean obsessing over every bite; it means finally having a clear, science-based map of a system that has been quietly influencing you your entire life.
The Hidden World Inside You: What Your Microbiome Really Is
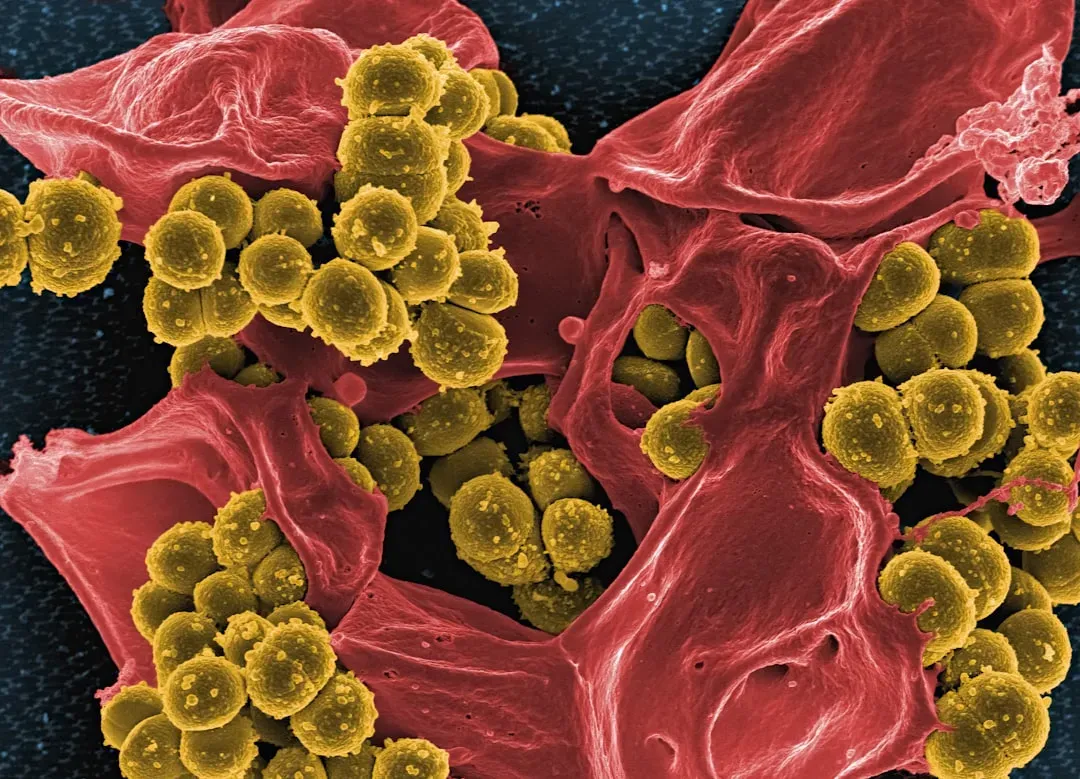
Right now, you are outnumbered by microbes. For every human cell in your body, you host roughly a similar order of magnitude of bacteria, viruses, and fungi, with a huge proportion living in your gut. Together, this community is called your gut microbiome, and it behaves less like a random mix of bugs and more like a complex, coordinated ecosystem. You can think of it as a rainforest: countless species, each doing its own small job, but together creating a stable, resilient environment.
Most of these microbes are not invading enemies; they are more like long-term roommates and business partners. Many of them help you digest fibers you cannot break down on your own, produce vitamins, and train your immune system to tell the difference between harmless visitors and real threats. When this inner city is in balance, you tend to feel better, digest more smoothly, and bounce back faster from stressors. When it is out of balance, you are more likely to notice bloating, irregular bowel habits, low energy, or just a vague sense that your gut is not on your side.
Your Second Brain: How Your Gut Talks to Your Mind
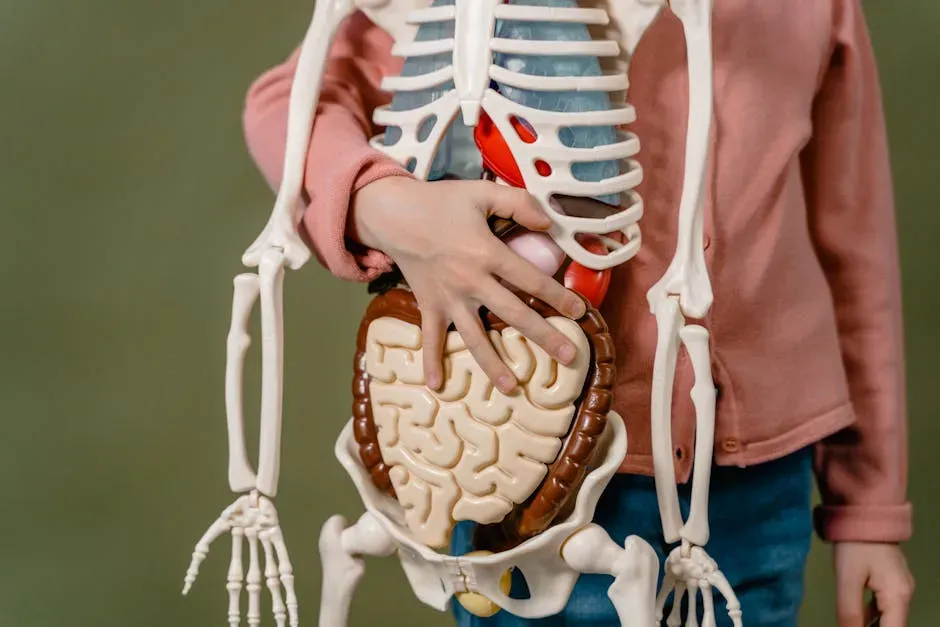
It might sound dramatic to call your gut a second brain, but biologically it is not that far off. Lining your digestive tract is a dense network of neurons called the enteric nervous system, which can operate independently of your brain and spinal cord. This system constantly communicates with your central nervous system through what is known as the gut–brain axis, sending and receiving signals that influence digestion, mood, pain, and even decision-making. You are not always conscious of it, but your brain is in nonstop conversation with your gut.
Your gut microbes are active participants in this conversation. They help produce and modulate signaling molecules that can affect neurotransmitters involved in mood, such as serotonin and GABA. A large share of the body’s serotonin is found in the gut rather than the head, and although that does not mean your microbiome is “controlling your emotions,” it does mean your digestive system plays a genuine role in how you feel. When your gut is inflamed or your microbiome is disrupted, those signals can change, and you may notice more anxiety, irritability, or just a less steady emotional baseline.
Mood, Stress, and the Gut–Brain Feedback Loop

You have probably felt your gut react to your emotions: the stomach knots before a difficult conversation, the sudden urge to run to the restroom before a big presentation, or the loss of appetite after bad news. That is your gut responding to stress hormones and nervous system signals, tightening or speeding up digestion as your body prepares for potential danger. This reaction may have made sense when your threats were physical, but in modern life, repeated emotional stress can keep your gut in a low-grade state of agitation.
The tricky part is that the loop runs both ways. When stress alters your gut environment, it can shift your microbial balance, which may in turn change the signals sent back to your brain. Over time, this can set up a feedback cycle where chronic stress and microbiome imbalance feed into each other. You might notice this as more frequent indigestion, changes in bowel habits, or more “gut feelings” of unease. Learning to manage stress is not just about mental calm; it is also one of the simplest ways to protect the stability and diversity of your gut ecosystem.
Food as Information: How Your Diet Shapes Your Microbial City

Every meal you eat is not just feeding you; it is feeding your microbes. Different species thrive on different substrates, so your dietary pattern acts like a vote for which microbes you want to support. A diet rich in plant fibers, for example, tends to nourish bacteria that produce beneficial short-chain fatty acids, which can support your gut lining, help regulate inflammation, and even influence metabolic health. When you eat this way repeatedly, you are essentially landscaping your inner rainforest in favor of more resilient and helpful species.
On the other hand, a pattern heavy on ultra-processed foods, added sugars, and very low fiber can narrow the diversity in your microbiome. When the menu gets monotonous and low in fiber, some microbes lose their favorite food sources and decline, while others that can live on mucus or simple sugars may expand in ways that are not ideal. You might not feel the shift overnight, but over months or years, you can see the effects as more frequent digestive discomfort, lower energy, or difficulty managing weight. When you look at your plate, it helps to ask not just what this food does for you, but what it does for the microscopic community that works for you every day.
Signs Your Second Brain May Be Out of Balance
Your microbiome does not send you neatly labeled alerts, but it does offer hints when something is off. Recurring bloating, frequent constipation or diarrhea, and unexplained abdominal discomfort are common red flags that your gut environment may not be thriving. These symptoms are not proof of a microbiome problem on their own, but they are clear invitations to pay closer attention. You might notice that your digestion swings wildly depending on stress, sleep, or what you have been eating lately.
Beyond obvious digestive signs, a struggling microbiome can show up more subtly. You may feel more fatigued, catch minor infections more often, or notice shifts in your mood and mental clarity that do not seem fully explained by life circumstances. Sometimes, you might feel “off” in a way that is hard to describe, almost like your body’s baseline has shifted slightly downward. When you notice these patterns over weeks or months, it is worth considering your gut as a possible player, not to self-diagnose serious conditions, but to take your internal ecosystem seriously as a factor in how you feel day to day.
Practical Ways to Support a Healthy Gut Microbiome

You do not need a complicated supplement stack or a perfect diet to treat your microbiome better. One of the most powerful steps is surprisingly simple: increase the variety of whole plant foods you eat over the course of a week. Different fibers from vegetables, fruits, legumes, whole grains, nuts, and seeds become food for different microbial species, and that diversity is one of the clearest markers of a resilient gut ecosystem. Instead of fixating on one “superfood,” think about building a colorful, varied menu your microbes can feast on.
Beyond food variety, daily habits matter more than you might expect. Prioritizing consistent sleep, moving your body regularly, and managing stress through practices like walks, breathing exercises, or simple hobbies can all help regulate your gut–brain axis. Fermented foods such as yogurt, kefir, kimchi, or sauerkraut can add live microbes, while minimally processed, fiber-rich foods help them stick around. You do not have to overhaul your entire life at once; even small, steady shifts can give your microbial city better building blocks to work with.
Probiotics, Prebiotics, and What You Really Need to Know

With all the buzz around gut health, you might feel pressure to grab the latest probiotic or cleanse promising a total reset. Probiotics are live microorganisms that can confer benefits in certain situations, but they are not magic pills that override your lifestyle. Different strains do different things, and the ones studied for specific conditions are not always the same as what you see in generic products. If you are dealing with a medical issue, it is wise to discuss any targeted probiotic use with a healthcare professional instead of experimenting blindly.
Prebiotics are another key piece, and they often deserve more attention than they get. These are fibers and compounds in foods that your body does not digest but your microbes love, such as those found in onions, garlic, leeks, asparagus, oats, and many fruits and legumes. When you focus on prebiotic-rich foods, you are creating the conditions for helpful microbes to flourish, which may have a wider, more stable effect than occasionally swallowing a capsule. Think of probiotics as visitors and prebiotics as the long-term housing and food supply; both can have a place, but the foundations of your gut health are still your everyday diet, sleep, stress, and movement.
When to Seek Professional Help for Gut Issues

It is tempting to self-treat every gut symptom with diet tweaks or over-the-counter remedies, but there are times when you should not go it alone. If you notice ongoing pain, unexplained weight loss, blood in your stool, persistent diarrhea, or symptoms that wake you from sleep, it is important to get evaluated by a qualified healthcare professional. Your microbiome is powerful, but so are conditions like inflammatory bowel disease, celiac disease, or infections, and they need proper diagnosis rather than guesswork. Ignoring serious warning signs in the hope that a probiotic will fix everything can delay care you genuinely need.
Even when your symptoms are milder, talking with a professional can help you avoid common traps, like overly restrictive diets or unnecessary supplements. A clinician familiar with gut health can help you sort out what is likely to be harmless variation, what might reflect something more serious, and what simple changes could realistically help. You deserve more than random internet advice and trial-and-error; your second brain is complex, and getting expert eyes on the situation is an act of respect for your own body rather than a sign of failure.
Your Relationship With Your Second Brain
Once you realize that your gut is not just a passive tube but an active, talking partner in your health, it changes how you see everyday choices. That tired afternoon when you automatically reach for ultra-processed snacks, the weeks when you sleep poorly and live on takeout, the periods when stress becomes your default setting – your microbiome is quietly recording and responding to all of it. You are not expected to be perfect, but you are no longer in the dark either. You can see how the pattern of your days nourishes or depletes your inner ecosystem.
For me, noticing that my mood dipped on weeks when my meals were rushed and identical was a wake-up call. Once I started adding more variety – different grains, more colors on my plate, the occasional fermented food – I noticed not only less digestive grumbling but a steadier sense of energy. Your path will be your own, but the core idea is the same: you are in an ongoing relationship with your second brain, and every choice is a small conversation. The more you listen and respond with care, the more that hidden world inside you can work in your favor.
In the end, your microbiome is not a mysterious enemy or a miracle cure; it is a partner you have been living with all along. When you feed it well, protect it from chronic stress, and seek help when something feels truly off, you give your second brain the best chance to support your digestion, your immunity, and even your mood. The question is not whether your gut is influencing your life – it already is – but how intentionally you want to shape that influence from here on out. What small shift could you make today that your future self and your inner microbial city will quietly thank you for?