Imagine sitting around a dinner table in 2050 and realizing that, in all likelihood, everyone there will easily live past one hundred. That might sound like science fiction, but right now in 2026, some of the most serious scientists, physicians, and biotech founders on the planet are quietly working toward exactly that kind of world. The goal is not just to stretch life like an old rubber band, but to extend the years in which people feel clear-headed, energetic, and genuinely alive.
At the same time, it’s important to separate hype from reality. For every careful clinical trial inching forward, there’s a wild headline promising immortality next Tuesday. The truth sits somewhere in between: we are undeniably gaining tools to slow aspects of aging and reverse certain forms of damage, but we’re still far from being “ageless.” This article walks through the most serious, evidence-backed areas where medicine is rewriting what a normal lifespan might mean – and where we still need to be cautious.
The Shift From Treating Disease To Targeting Aging Itself

The most radical idea in modern medicine might also be the simplest: instead of fighting one disease at a time, what if we treat aging as the root cause? Many of the conditions that kill or disable us – heart disease, cancer, dementia, frailty – rise sharply with age, like branches of the same tree. Researchers in geroscience argue that by slowing the underlying aging processes, we might delay many diseases at once, gaining not just extra years, but extra healthy years.
There’s already real data hinting this is more than a dream. Certain genetic variants that influence pathways like insulin signaling or lipid metabolism have been linked to people who live unusually long and stay surprisingly free of disease well into their nineties and beyond. Drugs that tweak some of these same pathways, like those affecting how cells sense nutrients or manage energy, are being tested to see if they can nudge human biology into a slower-aging mode. No one has a “longevity pill” yet, but the strategy – target aging, not just disease – has shifted from fringe theory to mainstream research agenda.
Senolytic Therapies: Clearing Out The Body’s “Zombie” Cells
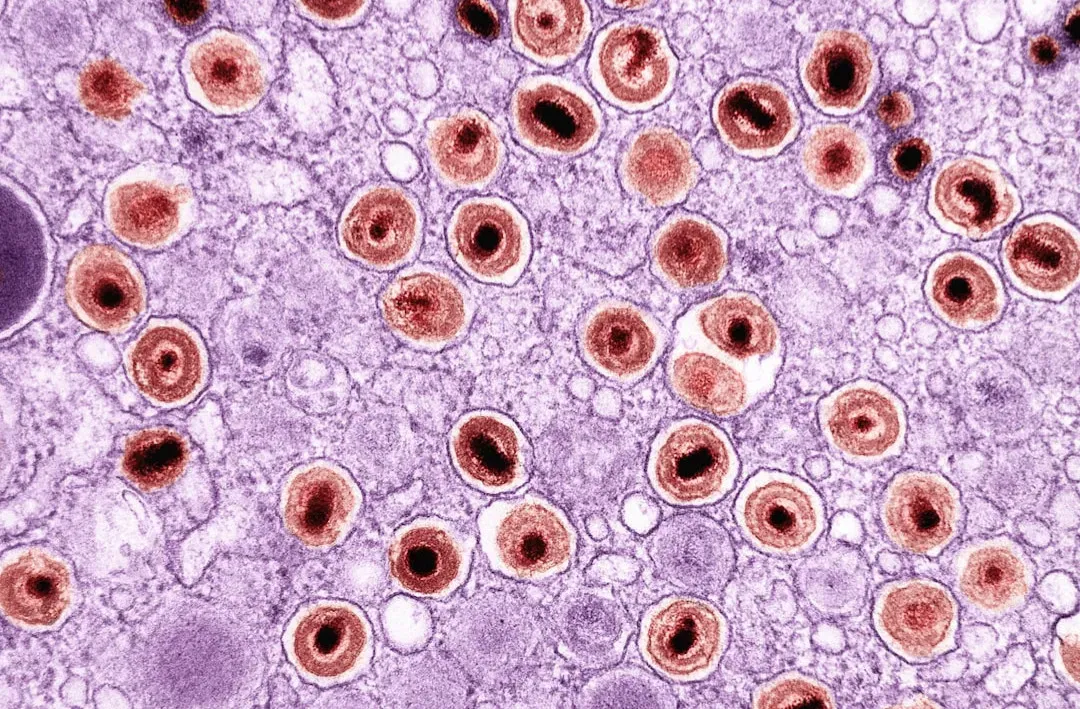
One of the most eye-catching fronts in longevity research is the hunt for senolytic drugs, therapies that selectively destroy old, damaged cells known as senescent cells. These cells stop dividing, but they don’t quietly die; instead, they hang around and leak inflammatory signals that can disrupt nearby tissues, like a few rotten apples spoiling the whole basket. As we age, these cellular “zombies” accumulate in organs, joints, blood vessels, and even the brain.
In animal studies, periodically removing senescent cells has extended lifespan and, more importantly, improved healthspan – better heart function, stronger muscles, delayed cancers, and sharper cognition in older mice. Early human trials for conditions like age-related lung disease and certain fibrotic disorders have produced cautious optimism, though the data is still limited and very much in progress. If senolytics can be made safe, specific, and practical, they could become a periodic tune-up for aging bodies, more like getting your car serviced than undergoing a major operation.
Regenerative Medicine: Stem Cells, Tissue Repair, And Organ Engineering
Living much longer only sounds appealing if your body can keep up – and that’s where regenerative medicine steps in. The big promise here is that we won’t just manage decline, but actually repair or replace worn-out parts. Stem cell therapies, where immature cells can develop into many different tissue types, are already being tested to repair damaged hearts, treat blood cancers, and tackle diseases like macular degeneration that rob people of sight.
Alongside stem cells, scientists are making striking progress with lab-grown tissues and early attempts at 3D-printed organs. Miniature organ-like structures, sometimes called organoids, are being used to model diseases and test drugs in more realistic ways than petri dishes ever could. While we’re not mass-printing replacement kidneys yet, several groups have produced functional pieces of liver, cartilage, and skin in controlled settings. If even a fraction of this becomes clinical reality, future older adults might repair injuries and organ damage in ways that feel almost routine, instead of life-defining events.
Gene Editing And Gene Therapy: Rewriting The Rules Of Risk

Gene editing used to sound like a plot device; now it’s in actual patients. Tools like CRISPR-based systems and other gene-modifying technologies are being trialed for diseases such as sickle cell disease, certain inherited blindnesses, and high-risk cholesterol disorders. For some people, a single genetic tweak has turned a lifelong, disabling disease into something dramatically milder – or in the best cases, seemingly resolved.
When it comes to longevity, the most intriguing question is whether we can gently edit away some of the risk factors that drive age-related diseases. For example, modifying how the body handles cholesterol or processes harmful proteins in the brain could reshuffle the deck for heart disease or dementia decades down the line. This area is moving carefully, though; editing the genome has lasting consequences, and off-target effects are not just a theoretical worry. Still, if we can safely and precisely correct the worst genetic hand-me-downs, longer, healthier lives become much more plausible.
AI-Driven Drug Discovery And Personalized Treatment
Artificial intelligence isn’t just recommending movies; it’s helping design new drugs and treatment plans at speeds that would’ve sounded ridiculous a decade ago. Machine learning systems can sift through mountains of biological data, from protein structures to clinical records, and spot patterns that humans would miss. That’s how some AI-designed molecules have already moved from digital prediction to real-world trials, including drugs targeting fibrosis, cancer, and metabolic diseases.
On the clinical side, AI is starting to help physicians tailor treatments to individual patients rather than relying on one-size-fits-most guidelines. By analyzing lab results, genetic data, medical images, and even wearable device information, algorithms can flag who’s at high risk of certain age-related conditions long before symptoms appear. If this is done responsibly and with strong safeguards against bias and privacy abuse, it could mean that future sixty- or seventy-year-olds get precisely tuned interventions that keep them thriving instead of gradually sliding into frailty.
Metabolic Reprogramming: Mimicking Fasting And Exercise In A Pill

One of the most consistent findings in aging research is that how our bodies handle energy – food, fat, sugars – has a huge impact on lifespan. In many animal models, periods of calorie restriction or intermittent fasting extend life and delay diseases, likely by triggering repair mechanisms and stress responses that keep cells in better shape. Of course, strict calorie restriction is miserable and not realistic for most people over decades.
So scientists are trying to capture the benefits without the suffering, developing drugs that mimic some of the cellular effects of fasting or intense exercise. Compounds that tweak nutrient-sensing pathways such as mTOR or AMPK are being studied for their potential to improve metabolic health, protect organs, and possibly slow components of aging. At the same time, the explosion of new drugs for obesity and diabetes – some of which produce large, sustained weight loss – could indirectly extend healthy lifespan by sharply cutting risks of heart disease, kidney failure, and more. We’re still figuring out the long-term trade-offs, but the direction of travel is clear: targeting metabolism is central to any credible lifespan expansion story.
Brain Health, Neuroprotection, And The Battle Against Dementia

A longer life without a healthy brain is a hollow victory, which is why neurodegeneration is one of the biggest bottlenecks for truly expanded lifespans. In the last few years, there have been new drugs that target abnormal protein buildup in the brain, particularly in Alzheimer’s disease. Some of these therapies modestly slow cognitive decline in certain patients, though they bring side effects and plenty of debate about risk versus benefit.
Beyond drugs, researchers are exploring ways to protect and regenerate the brain itself, from stem cell approaches to brain-computer interfaces designed for conditions like paralysis. High-resolution imaging and fluid biomarkers are allowing earlier and more accurate detection of neurodegenerative changes, often years before obvious memory problems appear. If we can catch the earliest sparks of dementia and intervene before the fire spreads, living to one hundred or beyond with a sharp mind becomes a lot less far-fetched.
Longevity Clinics, Biomarkers, And The Rise Of Preventive Medicine

Around the world, a new type of medical service is popping up: longevity clinics that offer deep testing, monitoring, and lifestyle coaching focused on delaying aging. Some of these clinics are experimental and expensive, catering to wealthy early adopters who undergo frequent lab tests, imaging scans, sleep tracking, microbiome analyses, and more. The goal is to detect small deviations from optimal health long before they become diagnosable disease.
Central to this movement is the search for reliable biomarkers of biological age – measures that reflect how “old” your body truly is, not just how many birthdays you’ve had. DNA methylation clocks, inflammatory markers, and composite scoring systems are being refined to predict risk of mortality and age-related illness with growing accuracy. While not perfect, they’re getting good enough that people can see whether certain diets, exercise regimens, or medications might be nudging their biological age down. Over time, what’s now a niche service for the few could evolve into standard preventive care for many.
Ethical Fault Lines: Who Gets To Live Longer, And On What Terms?

Even if the science delivers on a fraction of its promises, there’s a hard ethical question we can’t dodge: who gets access? If powerful life-extending therapies are expensive and limited, then longer lifespans could initially be a privilege of the wealthy, widening health gaps in ways that feel deeply unfair. It’s not hard to imagine a world where some people routinely reach one hundred and twenty in comfort while others still struggle to reach seventy in good health.
There are also social and psychological questions that don’t have easy answers. How do careers, family planning, retirement systems, and even our sense of identity change if “middle age” stretches well into our seventies? Some cultures may eagerly embrace extended lifespans; others might worry about overpopulation, generational stagnation, or pressure to work longer. These aren’t reasons to halt progress, in my view, but they are reasons to insist that conversations about equity, consent, and quality of life keep pace with the technology.
Why A Longer Life Only Matters If We Make It A Better One

When people talk about life extension, the conversation often jumps straight to numbers: ninety, one hundred, one hundred and twenty. But the most important breakthroughs we’re seeing now are really about compressing suffering – shrinking the years spent in disability and pain, and expanding the years in which we can hike with friends, learn new skills, or simply wake up without dread. In that sense, the true promise of modern medicine is not just longer life, but a different shape of life, where the cliff of old age becomes more of a gentle slope.
Personally, the possibility that my generation might see real, tangible changes in how long and how well we live feels both thrilling and grounding. It reminds me that no pill or procedure will ever replace the basics: movement, connection, purpose, and some measure of joy. The breakthroughs coming down the pipeline could give us more time; what we choose to do with that time is still entirely on us. If the future really does hand us extra decades of good health, how do you imagine using yours?



