Getting older is one of the few guarantees in life, yet most of us barely understand what’s actually happening under the surface as the years go by. We notice the gray hairs, the slower recovery after a late night, the aches that didn’t used to be there, but the real story of aging is unfolding quietly in our cells, our DNA, and our immune system every single day. The wild part? Scientists are starting to figure out not only why we age, but which parts of the process might be flexible, maybe even reversible.
We’re living in a moment where “aging research” sounds less like science fiction and more like a serious, fast-moving field that pulls in biologists, doctors, tech founders, and billionaires with private longevity labs. That doesn’t mean immortality is around the corner, and there’s a lot of hype and nonsense mixed in with genuine breakthroughs. But if you’ve ever wondered whether aging is inevitable, how much we can slow it, or what it might mean to live healthily into your nineties or beyond, the science has some surprising, and sometimes unsettling, answers.
The Surprising Truth: Aging Is Not One Single Thing

Most of us talk about aging like it’s one big, monolithic process, as if everything simply “wears out” at the same rate. In reality, aging is more like a messy orchestra with many instruments drifting out of tune at different times: DNA damage, immune dysfunction, hormonal changes, and cellular stress all piling up in overlapping waves. This is why one person may have strong bones but a failing heart, while another keeps a sharp mind but struggles to move easily. Aging is less a single program and more a tangled result of biology trying to maintain balance under constant pressure.
Scientists often break aging down into “hallmarks,” such as genomic instability, telomere shortening, loss of protein quality control, stem cell exhaustion, and chronic inflammation. Think of these like the main plot lines in a complicated series: they influence each other, amplify each other, and sometimes make things worse even when your body is trying to repair the damage. That’s also why there’s probably not going to be one magic pill; slowing aging likely means nudging several of these systems at once rather than flipping a single switch.
DNA Damage and the Slow Erosion of Our Genetic Blueprint

Inside every cell, your DNA is constantly under attack from the environment and from normal metabolism, like a library whose books are slowly being smudged, torn, and scorched. Ultraviolet light, pollution, cigarette smoke, and even just breathing and eating generate reactive molecules that nick, break, or chemically alter DNA. Your cells do have repair systems that jump into action, fixing most of the damage before it causes trouble, but those systems aren’t perfect and seem to become less efficient with age.
Over decades, small errors accumulate, like typos in an instruction manual, sometimes pushing cells toward malfunction, senescence, or even cancer. There’s also growing interest in epigenetics, the chemical tags that sit on top of DNA and decide which genes are turned on or off. These tags drift with time, a phenomenon some researchers call “epigenetic drift” or “epigenetic aging,” and you can now measure biological age by reading these patterns. The big question, which labs around the world are racing to answer, is how much of this drift we can safely reverse without causing chaos.
Telomeres: The Biological Fuses at the Ends of Our Chromosomes
Telomeres are often called the “caps” at the ends of chromosomes, but a better picture is to imagine the plastic tips on your shoelaces that keep them from fraying. Every time a cell divides, its telomeres get a little bit shorter, and when they become too short, the cell either stops dividing or self-destructs. This acts as a safety mechanism against runaway cell growth, which is helpful for preventing cancer, but it also means that our cells have a kind of division countdown clock built in.
In some tissues, like the bone marrow or the gut, an enzyme called telomerase can rebuild these telomeres, giving stem cells more “lives” to keep the system going. However, most normal cells don’t have much telomerase activity, so telomere shortening continues across the years. Shorter telomeres have been linked with higher risks of heart disease, weaker immune function, and earlier death, but it’s still debated how direct that cause-and-effect really is. Interestingly, lifestyle factors like chronic stress, sleep quality, and physical activity seem to influence telomere length, suggesting that how we live can subtly change how fast our biological fuse burns down.
Cellular Senescence: Zombie Cells That Refuse to Die
Imagine a group of workers in a factory who can no longer do their jobs properly but refuse to retire and instead stand around yelling and throwing tools; that’s not far off from what cellular senescence looks like. When cells accumulate too much damage or stress, they can enter a senescent state: they stop dividing, but they don’t disappear. Instead, they linger and start secreting a stew of inflammatory molecules, growth factors, and enzymes that can damage nearby tissues. Over time, these “zombie cells” build up in organs like fat tissue, joints, and blood vessels.
In small numbers, senescent cells are actually useful, helping with wound healing and cancer suppression. The problem is the chronic accumulation with age, which many researchers now see as a major driver of age-related disease. This is why there’s so much buzz around “senolytic” drugs, designed to selectively kill senescent cells and clean up the cellular neighborhood. Early animal studies show improved physical function and delayed onset of some diseases, but translating this safely to humans is tricky, and no one yet knows the long-term trade‑offs of wiping out cells that are both harmful and, in some contexts, protective.
Mitochondria and Energy: When the Body’s Power Plants Falter
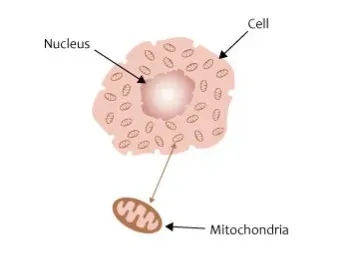
Mitochondria are often described as the power plants of the cell, turning nutrients into usable energy, but they’re more like a combination of battery, furnace, and control center. As we age, mitochondrial function tends to decline, leading to less efficient energy production and more leakage of reactive byproducts that can damage proteins, lipids, and DNA. You feel this in everyday life as fatigue, slower recovery, and the sense that your body just doesn’t have the same “spark” it used to. Muscle cells, brain cells, and heart cells, which are extremely energy-hungry, are particularly vulnerable when mitochondria falter.
There’s evidence that exercise, especially activities that challenge both strength and endurance, can stimulate mitochondrial biogenesis, essentially telling your cells to build more and better-functioning mitochondria. Certain dietary patterns, such as time-restricted eating or mild caloric reduction, may also nudge mitochondria toward more efficient energy use. Researchers are exploring compounds that might fine-tune mitochondrial performance, but the line between helpful enhancement and harmful overstimulation is delicate. In my own life, the difference in energy between a week of regular movement and a week of pure sitting is stark enough that I don’t really need a lab test to be convinced this system matters.
Inflammation and the Immune System: When Defense Turns Destructive
Inflammation is one of the body’s most powerful defense tools, rushing cells and signals to sites of injury or infection, like an emergency crew racing to a fire. The problem is that with age, the immune system starts sending out low-level alarm signals almost all the time, even when there’s no real emergency. This chronic background inflammation, often called “inflammaging,” slowly erodes tissues, damages blood vessels, and makes many organs more vulnerable. It also contributes to insulin resistance, joint pain, and a higher risk of cardiovascular disease.
At the same time, other parts of the immune system weaken: there are fewer fresh, naive immune cells to respond to new pathogens, and memory cells can become unbalanced. This combination of chronic overreaction and reduced precision is one reason older adults are more prone to infections and respond less strongly to some vaccines. Lifestyle does matter here; steady sleep, regular movement, avoiding smoking, and a diet rich in unprocessed foods all help dial down needless inflammation. But there is still a hard biological ceiling, and no anti-inflammatory supplement can fully erase the deep, structural changes that decades of living carve into the immune system.
The Longevity Levers We Actually Control Right Now

When people think about living longer, they often jump straight to exotic ideas like gene editing, stem cell therapies, or futuristic age-reversing injections. Ironically, the best-supported tools for increasing healthy years are still almost boring: not smoking, staying physically active, maintaining a healthy weight range, eating mostly whole, minimally processed foods, managing blood pressure and blood sugar, sleeping enough, and nurturing genuine social connection. Large, long-term population studies keep pointing back to these same factors as the foundation for both longer life and better life quality. None of them guarantee anything, but together they tilt the odds in a meaningful way.
On a more experimental edge, researchers are studying drugs like metformin and rapamycin, as well as patterns like intermittent fasting, as potential life‑extending strategies. Some early human and animal data are encouraging, particularly around metabolic health and delayed onset of age-related diseases, but the long-term picture is far from settled. It’s easy to get pulled into the promise of a “longevity hack,” but most experts caution that stacking simple, proven habits still beats chasing the latest miracle compound. The unglamorous truth is that a daily walk, consistent sleep, and real relationships probably do more for your future self than any pill currently sold as a fountain of youth.
Cutting‑Edge Longevity Research: Reprogramming, CRISPR, and Beyond
Beyond lifestyle, the frontier of aging research looks like something pulled from a sci‑fi script: partial cellular reprogramming, gene editing, organ regeneration, and lab‑grown tissues. Partial reprogramming experiments in animals have shown that you can dial back some markers of cellular age by temporarily activating certain developmental genes, essentially nudging old cells to behave more youthfully. The challenge is doing this without pushing cells all the way back to a stem‑like state, which raises the risk of cancer and uncontrolled growth. It’s like trying to renovate an old house without knocking it back into a bare foundation.
CRISPR and other gene-editing tools add another layer of possibility, allowing targeted changes to genes that influence longevity, disease risk, or resilience to cellular stress. There have been intriguing experiments in animals where tweaking single genes extends lifespan or delays age-related decline, but humans are far more complex, and every gene sits in a vast network of interactions. There’s also a serious ethical question around who gets access to such tools and what happens if we start editing traits tied to aging and risk tolerance. For now, much of this work is still preclinical, fascinating and hopeful but nowhere near the level where you’d want it casually offered at a clinic on a beach somewhere.
Immortality, Ethics, and the Question of a Life Well Lived

The phrase “quest for immortality” sounds dramatic, but it’s not completely off the mark for some of the wealthiest and most ambitious people investing in longevity science. Yet even if we could halt biological aging tomorrow, the social and ethical questions would be staggering. How would ultra‑long lives reshape work, family, and generational turnover? What would it mean for resource use, inequality, and political power if a small group could extend their healthy years far beyond everyone else’s? It’s not hard to imagine ways this could go wrong if left to pure market forces and personal desire.
On a more personal level, stretching out life raises deep questions about meaning, motivation, and what counts as a good life rather than just a long one. Many philosophers, and frankly many ordinary people, have worried that endless time might dull urgency and purpose, turning life into an overlong movie that has lost its emotional edge. When I think honestly about the future, I’m less interested in living forever and more interested in maximizing the number of years in which I can move easily, think clearly, and enjoy the people I love. Immortality makes for great headlines, but learning how to compress sickness into the shortest possible slice at the end might be the more humane and realistic goal.
Conclusion: Aging as a Story We Can Help Shape

Aging is often painted as a slow, unavoidable slide downhill, but the science tells a more complex, and oddly empowering, story. We do carry biological clocks in our DNA, mitochondria, immune system, and telomeres, yet those clocks do not all tick at the same rate, and our choices can nudge them faster or slower. No one can opt out of aging completely, at least not with anything available today, but we can tilt the odds toward a longer “healthspan,” the stretch of years where we can live on our own terms. The emerging tools of reprogramming, gene editing, and senolytic drugs hint that the next few decades could radically redefine what it feels like to be seventy, eighty, or ninety.
At the same time, chasing eternal life without asking what it’s for risks missing the point of being alive in the first place. The real power of longevity science might not be in defeating death, but in giving us more time to love, create, and contribute while we’re here, with bodies and minds that still feel like our own. The question, then, isn’t just how long we can stretch the line of our life, but how deeply we can fill it while we have the chance. If you knew you could add more healthy years, how differently would you live the ones you already have?



