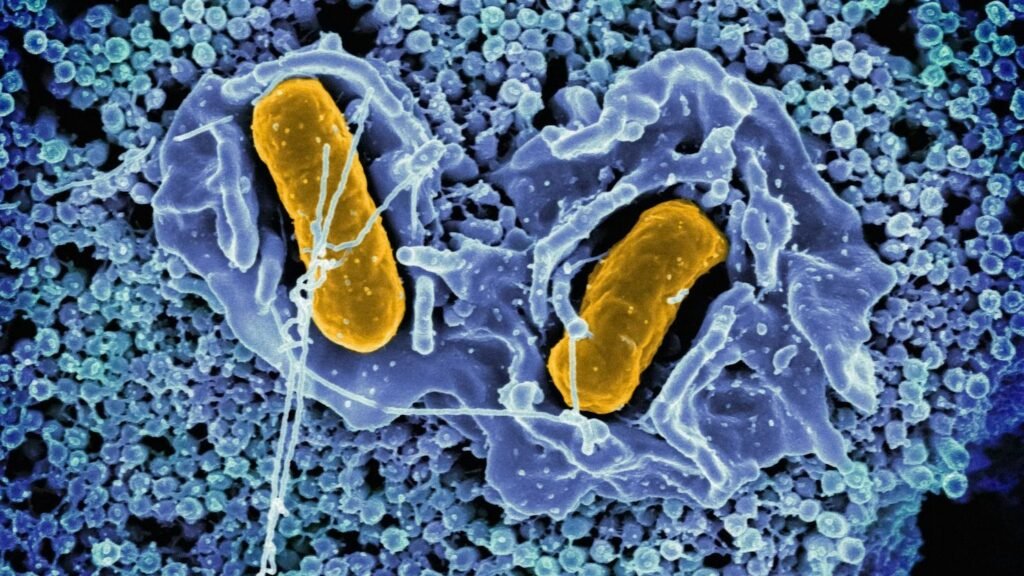
If someone told you that you’re mostly microbe, not human, it would sound like a bad sci‑fi plot. Yet right now, trillions of microscopic organisms are living all over you and deep inside you, quietly shaping your health, your mood, even how you respond to certain foods and medicines.
For years, I thought of germs as the enemy: things to scrub away, sanitize, and kill with harsh soap. Then I stumbled across research on the microbiome and realized I’d been waging war on some of my closest allies. Once you see your body as an ecosystem rather than a machine, everything from diet to antibiotics suddenly looks very different.
The Microbiome: An Invisible Super‑Organ
Imagine carrying around a rainforest, a coral reef, and a bustling city all at once, except they’re compressed into your gut, mouth, skin, and more. That’s essentially your microbiome: the vast community of bacteria, fungi, viruses, and other microbes that live in and on your body. They’re not freeloaders; they’re more like a tiny outsourced workforce that your body has evolved with over millions of years.
Researchers sometimes refer to the microbiome as a “forgotten organ” because it has its own complex roles: digesting food, producing vitamins, training the immune system, and more. The total number of microbial cells in and on us is in the same ballpark as our human cells, and their combined genes massively outnumber our own. In other words, the genetic code you walk around with is largely microbial, and your daily choices either feed or starve this hidden universe.
Where Your Microbes Live (Spoiler: Basically Everywhere)
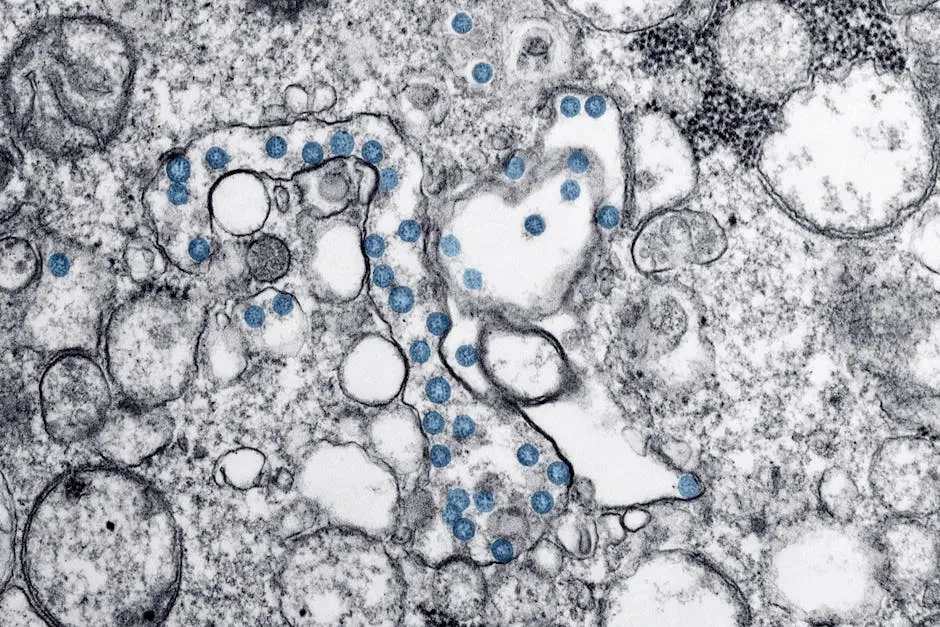
The gut microbiome gets most of the attention, and honestly, it deserves the spotlight. The large intestine is like a bustling metropolis of microbes, with dense communities that help ferment fibers, break down complex molecules, and create compounds your own cells can’t make. But microbes also colonize your mouth, nose, skin, lungs, and even the urogenital tract, each area with its own distinct ecosystem.
Your skin hosts dry, oily, and moist micro‑neighborhoods, each supporting different species, like different climates on Earth. The mouth is more like a crowded harbor, with communities on the tongue, teeth, and gums that constantly deal with what you eat and drink. Even your armpits and feet have their own microbial “signatures,” which is a polite way of saying that some of your personal smell is literally the scent of microbial chemistry in action.
How Your Microbiome Shapes Digestion and Nutrition
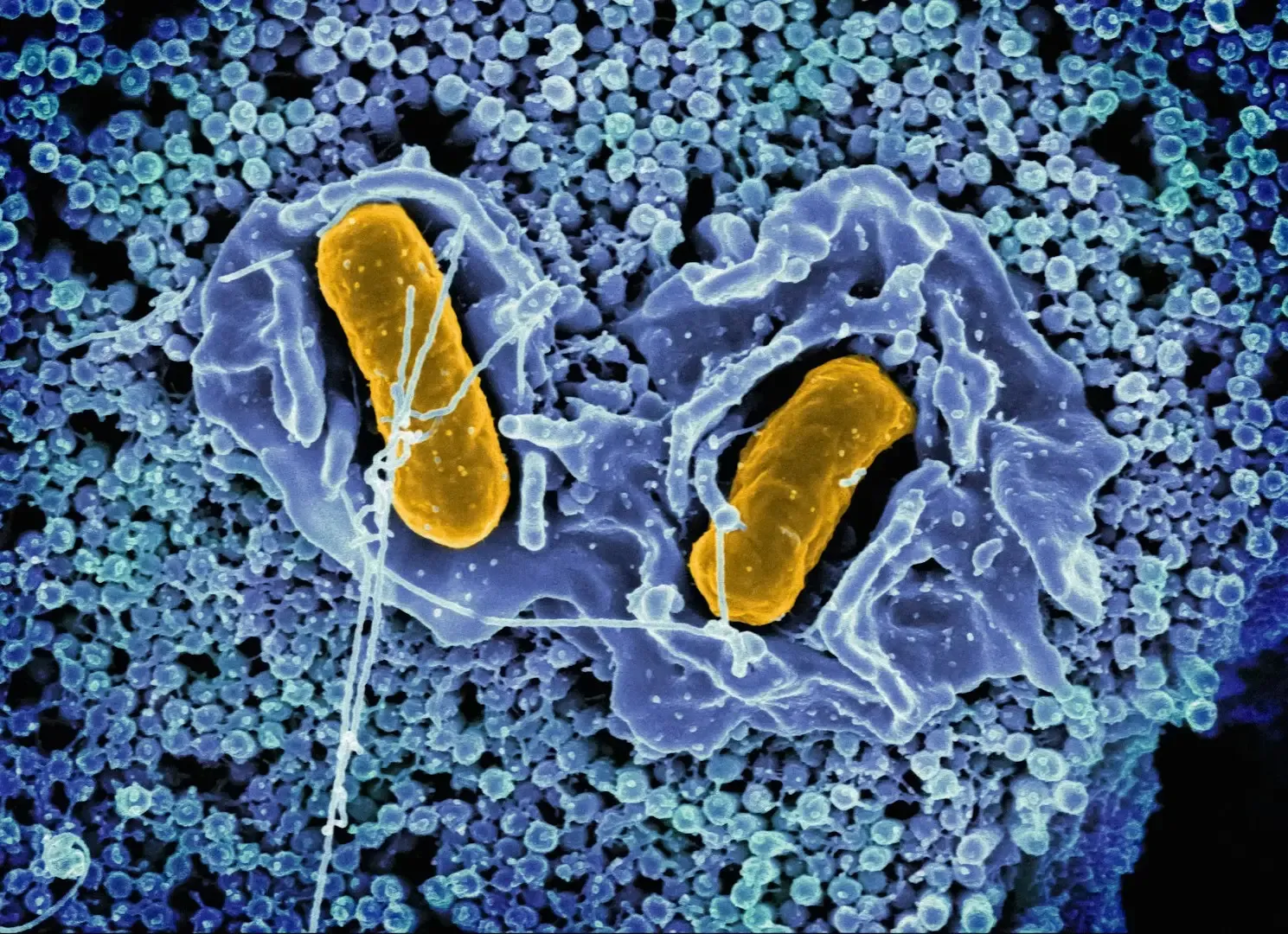
When you eat, you’re not just feeding yourself; you’re feeding your microbes too. They feast on different components of your food, especially dietary fibers and complex plant compounds that your own enzymes can’t handle. In return, they produce short‑chain fatty acids and other molecules that help nourish the cells lining your gut, support immune balance, and influence how much energy you extract from your meals.
Some people’s microbiomes are better suited to extracting calories from certain foods, which may help explain why two people can eat similarly but gain weight differently. Microbes also help synthesize certain vitamins, such as some B vitamins and vitamin K, adding an invisible bonus layer to your nutrition. When your diet lacks fiber and is overloaded with ultra‑processed foods, this microbial food chain gets disrupted, and over time that can ripple into bloating, irregular digestion, and broader health issues.
The Gut–Brain Connection: Mood, Stress, and Microbes
It sounds wild, but your gut talks to your brain constantly, and microbes are part of that conversation. The gut and brain are linked through nerves, hormones, and immune signals, creating what scientists call the gut–brain axis. Many gut microbes produce or influence the production of neurotransmitters and signaling molecules that can affect mood, stress response, and even sleep.
People often notice that periods of intense stress show up in their digestion: stomach knots, cramping, or changes in appetite. That road goes both ways; emerging research suggests that a disrupted microbiome is associated with higher rates of anxiety and low mood in some people. The data is still evolving and far from simple, but one thing seems clear: when your gut ecosystem is inflamed or out of balance, your brain often feels it too, even if it just shows up as crankiness, brain fog, or poor sleep.
Microbes and Immunity: Your Inner Training Camp
Your immune system grows up learning the difference between friend and foe, and microbes are some of its first teachers. Early in life, exposure to a wide range of harmless microbes helps the immune system calibrate, so it doesn’t overreact to every little thing. When this training is disrupted, the immune system may lean toward chronic inflammation or allergic overreactions.
The gut lining is a busy border crossing where microbes, food particles, and immune cells constantly interact. Helpful microbes compete with potentially harmful ones for space and resources, produce substances that calm inflammation, and help maintain a strong but selective barrier. When microbial diversity drops and certain species dominate, that balance can tilt toward inflammation, which is increasingly linked to conditions ranging from inflammatory bowel disease to metabolic and cardiovascular problems.
Antibiotics, Sanitizers, and the Collateral Damage Problem
Antibiotics have saved countless lives, but they’re also like carpet bombing for your microbiome. A single course can dramatically shift your gut community, wiping out helpful bacteria along with the dangerous ones. In some cases, the microbiome bounces back; in others, the balance changes long‑term, opening space for more harmful species to take hold.
Our obsession with constant sanitizing adds another layer to the story. Over‑using strong antimicrobial soaps and surface disinfectants in everyday life may reduce healthy everyday microbial exposure without real benefit for most people. It doesn’t mean you should never use antibiotics or forget hand‑washing; it means using them wisely: antibiotics only when truly needed, routine soap instead of harsh antibacterial products, and a bit less fear of everyday dirt and normal life microbes.
Food for Your Microbes: Fiber, Ferments, and Variety

If you think of your microbiome as a garden, your daily diet is the watering can and fertilizer. Microbes especially love diverse plant fibers: vegetables, fruits, whole grains, legumes, nuts, and seeds. These fibers act as prebiotics, feeding beneficial bacteria that, in turn, create compounds associated with better gut and metabolic health.
Fermented foods like yogurt with live cultures, kefir, sauerkraut, kimchi, and some traditionally fermented soy products can introduce or support beneficial bacteria. No single food is magic, but regularly rotating a wide variety of whole, minimally processed foods gives your microbial community more to work with. On the flip side, diets heavy in added sugars, ultra‑processed snacks, and low in fiber tend to starve helpful microbes and encourage a narrower, less resilient ecosystem.
Probiotics, Prebiotics, and Hype vs. Reality

Walk down any supplement aisle and you’ll see shelves full of probiotic pills promising better digestion, stronger immunity, and a brighter mood. The reality is more nuanced. Some specific probiotic strains have solid evidence for certain conditions, like preventing some antibiotic‑associated diarrhea or helping with specific digestive issues, but many products simply haven’t been rigorously tested in humans.
Prebiotics, which are fibers or compounds that feed beneficial microbes, have more consistent support for nurturing a healthier microbiome overall, especially when they come from whole foods. In practice, that means most people will get more reliable benefit from changing what they eat than from swallowing random capsules. Supplements can be helpful in specific situations, but they’re more like small tools than a magic reset button for a microbiome that’s been neglected for years.
Microbiomes Across Life Stages: From Birth to Old Age
Your microbiome story starts even before you’re born and changes throughout life. How you enter the world, your early feeding (breast milk, formula, or both), your environment, pets, siblings, and diet all contribute to how your microbial ecosystem gets seeded and shaped. Early childhood is a time of intense microbiome development, and that early pattern can influence immune tendencies later in life.
As we age, diversity in the gut microbiome often drops, especially when diet becomes more limited or physical activity declines. Reduced diversity is linked to frailty and poorer health in many older adults. On the other hand, people who stay relatively active, eat a variety of fiber‑rich foods, and maintain social and lifestyle engagement tend to have more robust microbiomes into older age, suggesting that it’s never completely too late to nudge things in a better direction.
Simple Daily Habits to Support a Healthier Microbiome

You don’t need a lab or a fancy test to start caring for your hidden universe of microbes. A practical approach is to build your plate around plants most of the time: think colorful vegetables, fruits, beans, lentils, and whole grains, plus nuts and seeds. Aim for variety over perfection; trying one new plant food a week is enough to start nudging your microbes in a more diverse direction.
Other small shifts add up: move your body regularly, sleep reasonably well, manage stress in ways that work for you, and be conservative but not fearful with antibiotics and harsh antimicrobials. I’ve noticed that even a week of heavy takeout and poor sleep can leave my digestion and mood off, which now feels less like a mystery and more like my microbes filing a complaint. When you act as a caretaker for this inner ecosystem instead of fighting it, you often feel the difference in more stable energy, digestion, and resilience.
Conclusion: Living as an Ecosystem, Not a Lone Individual
Once you see yourself as an ecosystem instead of a solo human, it’s hard to unsee it. Your microbiome isn’t a side character; it’s woven into your digestion, immunity, mood, and how your body responds to the modern world. Every meal, every course of antibiotics, every late‑night stress spiral is, in some small way, a nudge to this invisible universe.
The encouraging part is that ecosystems can heal and adapt when you give them time, diversity, and fewer unnecessary shocks. You don’t have to chase perfection or obsess over every bite; you just have to consistently feed the right tiny partners and stop treating all microbes like the enemy. So next time you sit down to eat or reach for the extra‑strong sanitizer, will you think a little differently about the billions of quiet lives depending on your choice?