If you woke up tomorrow and your doctor could edit your DNA, spot disease years before symptoms, and prescribe a drug designed just for your body, it would feel like science fiction. Yet in 2026, you’re closer to that world than you might realize. Quietly, in labs and clinics around the globe, medicine is being rebuilt from the inside out.
This isn’t about shiny gadgets for their own sake. It’s about you living longer with less pain, catching deadly diseases when they’re still a whisper, and getting treatments that actually fit your biology instead of “average” data from decades ago. As you read through these breakthroughs, you’ll probably notice a pattern: medicine is moving from reactive and one‑size‑fits‑all to proactive and personal. And that shift will change almost everything about how you experience being a patient.
Gene Editing: From Treating Disease to Rewriting Its Rules
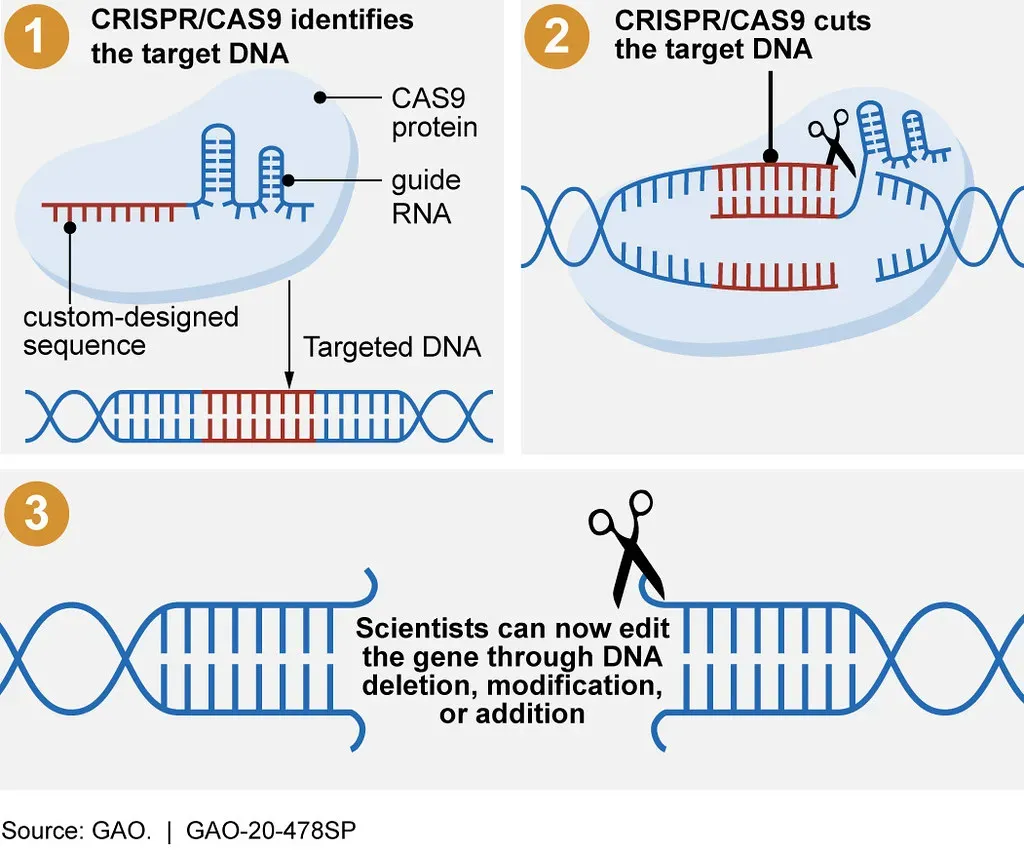
Imagine sitting across from a specialist who doesn’t just manage your genetic disease, but edits it at the source so it stops causing damage in the first place. That’s not a fantasy anymore. With tools like CRISPR, base editing, and prime editing, doctors can now change specific letters in your DNA, and regulators in the United States and Europe have already approved the first CRISPR-based therapies for blood disorders like sickle cell disease and beta thalassemia. You’re living at the moment when “incurable” inherited diseases are starting to get their first real cures instead of endless symptom control.
Even more striking, you’ve now seen the first personalized gene editing therapy used in a baby with a rare metabolic disorder, and early reports suggest it worked as intended. Researchers are also moving beyond classic CRISPR toward techniques like base and prime editing that can make ultra‑precise corrections with fewer unwanted changes. The big challenge for you and everyone else is no longer whether gene editing works at all, but how to make these therapies safer, cheaper, and accessible beyond a tiny group of patients in wealthy countries. The direction of travel is clear: your children or grandchildren might see genetic conditions treated as fixable glitches, not lifelong destinies.
AI Doctors and Smart Diagnostics at Your Fingertips

When you walk into a clinic a few years from now, there’s a good chance an AI system will have already scanned your records, flagged possible diagnoses, and prioritized what your doctor needs to check first. You’re already seeing AI tools read scans, analyze lab results, and summarize complex clinical notes with a level of speed no human can match. Large language models are being tested head‑to‑head against physicians for common internal medicine cases, and while they’re not perfect, they’re impressively capable in many tightly defined situations.
Outside the hospital, you’re also watching the rise of virtual “AI hospitals” and multi‑agent doctor systems that can evaluate thousands of simulated or real cases in days, offering decision support across hundreds of disease types. Still, every credible study and expert reminder tells you the same thing: AI is a powerful assistant, not a replacement for human judgment. The real future for you as a patient is a team where your clinician focuses on empathy, context, and nuanced decisions, while AI quietly handles the heavy lifting of pattern recognition, data crunching, and second opinions in the background.
mRNA and Next-Gen Vaccines That Adapt at Warp Speed
If you lived through the COVID‑19 pandemic, you saw mRNA vaccines go from obscure lab tech to global lifeline almost overnight. What you may not realize is that this platform has kept evolving ever since. Regulatory agencies have continued to approve updated formulas to match new variants, and companies are pushing mRNA-based shots against influenza and other serious respiratory viruses into late‑stage trials. Global health organizations are even training scientists around the world to manufacture mRNA vaccines locally, so future outbreaks do not leave entire regions waiting in line for doses.
For you, the deeper shift is that vaccines are becoming programmable. Instead of taking years to redesign and ship a new vaccine, researchers can update an mRNA sequence relatively quickly and slot it into established manufacturing pipelines. Beyond infectious disease, scientists are pushing mRNA toward cancer vaccines and therapies for rare conditions, where your immune system is trained to recognize exactly what is going wrong in your body. In practice, that means your future vaccines and immune‑based treatments could feel less like blunt shields and more like custom software patches tailored to your biology and the threats you face.
Continuous Health Monitoring: Turning Your Body Into a 24/7 Data Stream

Think about how you normally interact with healthcare today: you feel unwell, you book a visit, someone checks your vitals for five minutes, and then you go home. Future medicine wants to flip that model, and you can already see it happening on your wrist. Modern wearables track your heart rhythm, sleep patterns, activity, sometimes even blood oxygen and temperature around the clock. Researchers combine those streams with algorithms that can flag early signs of arrhythmias, respiratory issues, or metabolic problems, long before you would think to call a doctor.
In more advanced systems, your watch, phone, and even ambient sensors in your home can feed continuous data to AI models tuned for anomaly detection. Instead of a snapshot blood pressure reading in a clinic, your care team might see months of trends and subtle changes that cue early interventions. You’ll also see non‑invasive monitoring push into new territory, with companies chasing the holy grail of painless glucose tracking and more detailed cardiovascular metrics. The trade‑off for you will be balancing the convenience and safety of early detection with legitimate concerns about privacy, data security, and the constant psychological hum of being monitored.
Precision Medicine: Treatments Tailored Uniquely to You

Until recently, most of your care was based on what works “on average” for large groups of people. Precision medicine is about leaving that behind and designing prevention and treatment around your genetics, environment, lifestyle, and even the microbes living in your gut. Oncologists already test tumors for specific mutations before choosing therapies, and genetic panels are becoming routine for certain cancers and inherited conditions. In practice, that can mean you get a drug that targets the exact molecular pathway driving your disease, rather than a broad treatment with hit‑or‑miss outcomes.
As data builds from biobanks, electronic health records, and population‑scale genomic studies, you’ll see more risk scores and tailored recommendations enter everyday care. Your doctor might combine your family history, genome, cholesterol patterns, and wearable data to predict your risk of heart disease decades before your first symptom. At its best, this lets you act early, adjusting diet, exercise, or medication to dodge a future heart attack or stroke. But precision medicine also raises deep equity questions: if you live in a community underrepresented in research, your data and risks may be less well understood. Part of the future will be making sure your “precision care” is actually precise for you, not just for people who look like the original study group.
Regenerative Medicine and Lab-Grown Tissues
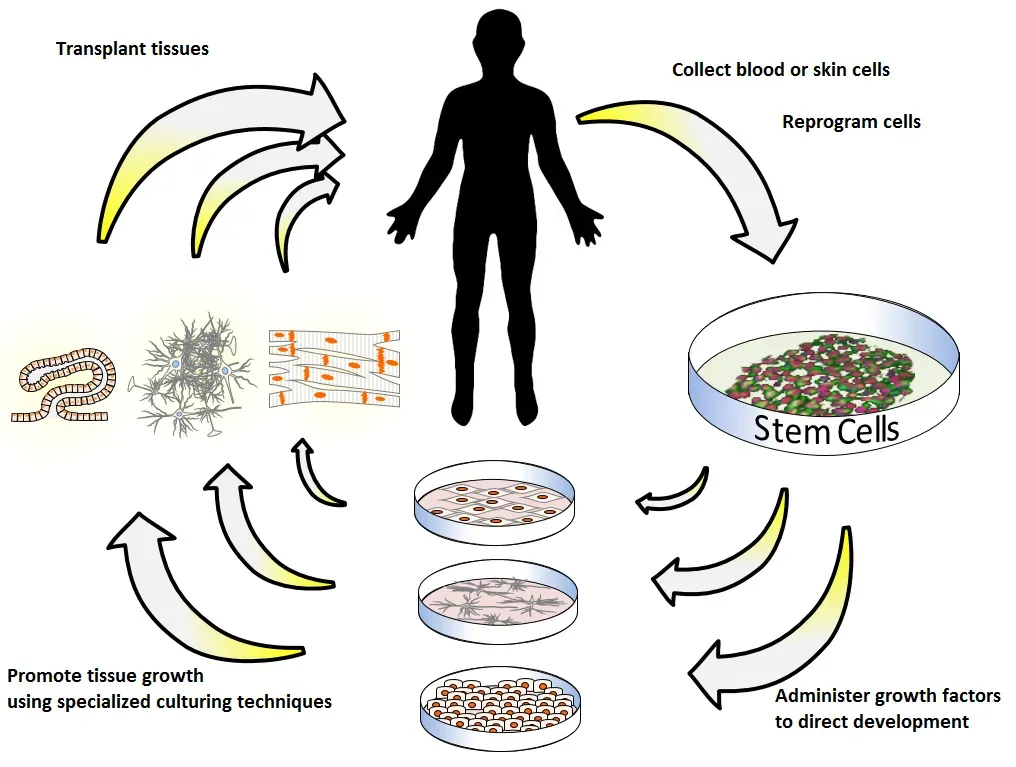
Picture tearing a knee ligament or burning a patch of skin and, instead of being told to accept permanent damage, you’re offered a way to regrow healthy tissue. That’s the promise driving regenerative medicine, and pieces of it are already in clinical use. Surgeons transplant lab‑grown skin, use stem‑cell‑based therapies for certain blood and eye conditions, and experiment with engineered cartilage and bone. Scientists are also refining organoids – tiny, organ‑like structures grown from your own cells – which can be used to study your disease in a dish and, eventually, could help repair or replace failing organs.
The dream scenario for you might sound almost magical: a damaged organ scanned in detail, a patch of tissue or even a whole replacement grown from your own cells, and then surgically implanted without the rejection risks of traditional transplants. You’re not there yet, and there are stubborn hurdles in scaling, safety, and cost. But every year brings more proof that your body is not a static machine; it can be coached, supported, and supplemented to repair itself in ways that would have seemed impossible to your grandparents. Over time, this could redefine what “irreversible” injury really means.
Virtual, Augmented, and Remote Care: The Clinic Comes to You

If you’ve had a telehealth visit from your couch, you’ve already felt the first wave of virtual care. The next wave goes much further. Surgeons are training and planning operations in detailed virtual reality environments, and some interventional procedures blend real‑time imaging with augmented reality overlays to guide instruments inside the body. For you, that can mean shorter procedures, fewer complications, and doctors who practice with lifelike simulations instead of learning mainly from real‑world trial and error.
At the same time, remote care is expanding beyond simple video calls. In some systems, AI-enhanced virtual assistants triage your symptoms, help collect structured histories, and route you to the right level of care. Wearables or home devices can stream your data to remote monitoring centers, where clinicians step in quickly if early signs of trouble appear. You benefit from less travel, more continuity, and faster feedback, especially if you live far from major medical centers. But this shift also forces you and society to wrestle with digital access: if high‑quality care requires reliable internet and smart devices, then closing the digital divide becomes a health issue, not just a tech problem.
Ethics, Access, and the Fight to Keep Medicine Human

All of these breakthroughs sound exciting until you ask a simple question: will you actually get access to them? Gene therapies can cost more than a house, AI systems may work better for some populations than others, and mRNA manufacturing capacity is still unevenly distributed around the world. If the future of medicine only reaches wealthy urban patients, the gap between the health haves and have‑nots will quietly widen. That’s why you’re already seeing fierce debates about pricing, insurance coverage, public funding, and intellectual property surrounding these technologies.
There’s also a subtler risk: in the rush to automate and optimize, you could lose the human connection that makes care feel safe and dignified. No algorithm can replace the feeling of being listened to by someone who knows your story, your fears, and your values. The best version of the future is one where technology fades into the background, serving as scaffolding that lets clinicians spend more time looking you in the eye instead of staring at a screen. Your voice – as a patient, voter, and community member – will matter in shaping regulations, funding priorities, and ethical norms so that medical progress actually feels like progress in your own life, not just in press releases.
How You Can Prepare for the Medicine of Tomorrow
You might be wondering what you’re supposed to do with all of this. After all, you can’t personally run a gene editing trial or redesign the global vaccine supply chain. But you can start by becoming a more informed, active participant in your own care. That means asking your doctor when genetic or molecular testing is appropriate, understanding what your wearable data can and cannot tell you, and being cautious about health claims from unverified apps or AI chatbots. The more you understand the tools, the harder it is for hype or fear to push you into bad decisions.
You can also think of yourself as a stakeholder in the system, not just a customer. Supporting policies that expand clinical trial diversity, fund public health infrastructure, and regulate data privacy directly shapes the world you and your family will age into. If you’re comfortable with it, participating in research studies or data‑donation projects can help ensure that future algorithms and treatments actually work for people like you. The future of medicine is not something that simply happens to you; it’s something you influence, choice by choice, conversation by conversation.
Conclusion: A Future That’s Closer Than It Looks
When you step back and look at the big picture, the future of medicine is not defined by one flashy invention but by a deep shift in how health is understood and protected. Instead of waiting for disease to roar into your life, emerging tools aim to sense its earliest whispers, correct its roots, and support your body’s own repair systems. Gene editing, AI diagnostics, mRNA platforms, wearables, precision therapies, regenerative tricks, and virtual care are all pieces of the same puzzle: giving you more healthy years with better control and less guesswork.
None of this is guaranteed; cost, ethics, bias, and politics will shape how quickly and fairly these breakthroughs spread. But for the first time in human history, you’re watching medicine move from averaging across millions of people to genuinely tailoring care around the individual – around you. As these technologies mature, the question will not just be what they can do, but how wisely you choose to use them. Looking ahead, which of these changes do you most want to see in your own lifetime?