Everyone secretly asks the same question at some point: is aging just an unavoidable slide downhill, or is it a biological process we can actually control? You see it in the booming market for supplements, anti-wrinkle serums, and biohacking gadgets, but underneath the hype there’s a very real, very serious scientific effort to understand why we age at all. The surprising part is that biology is increasingly treating aging not as a mysterious curse, but as a complex but modifiable system.
We are now living in a moment where decades of lab research are finally colliding with powerful tools like gene editing, AI-driven drug discovery, and continuous health tracking. That does not mean immortality is around the corner, and a lot of bold claims are still way ahead of the evidence. But step by step, scientists have shown in animals – and are starting to hint in humans – that some aspects of aging can be slowed, and possibly even partially reversed. The question is not just whether we can live longer, but whether we can stay truly healthy for more of those years.
What Actually Is Aging, Biologically Speaking?

At its core, aging is not just about gray hair and sore knees; it is a gradual loss of resilience in almost every system in the body. Over time, our cells accumulate damage to DNA, proteins, and cell structures, and their ability to repair and clean up that mess slowly weakens. Imagine running a busy restaurant where the cleaning staff gets smaller and more tired each year – eventually the kitchen starts breaking down no matter how good the chef is. Aging looks a lot like that when you zoom in at the cellular level.
Scientists sometimes talk about a set of “hallmarks” of aging: genomic instability, mitochondrial dysfunction, senescent cells that refuse to die, chronic low-grade inflammation, changes in how genes are switched on and off, and more. None of these hallmarks act alone; they feed into each other like a bad feedback loop. What makes this exciting, though, is that these are not mystical forces. They are biological processes with knobs and switches, and in animal models, tweaking some of those knobs really does change how fast aging plays out.
Genes, Families, and the Limits of Longevity

If you look at families where many people live into their nineties or past one hundred, it is pretty clear that genes matter. Studies of twins suggest that genetics accounts for a meaningful but not overwhelming fraction of how long we live; lifestyle and environment still play a huge role. You can think of your genes like the hardware of a phone: some models are built more robustly, but how you use and maintain them matters a lot too. Even with “average” hardware, careful use and regular updates can go a long way.
Researchers have identified genetic variants associated with exceptional longevity, many of them involved in lipid metabolism, insulin signaling, and how cells respond to stress. But having those variants does not make anyone invincible, and not having them does not doom you to a short life. From a practical standpoint, we are still far from editing our genomes to perfectly tune lifespan, and many gene therapy approaches carry serious risks or are only in very early human trials. So yes, genes create a ceiling and a starting point – but they are not the final word on whether you can meaningfully slow your own aging.
Cellular Senescence: The “Zombie Cells” We Want to Clear Out
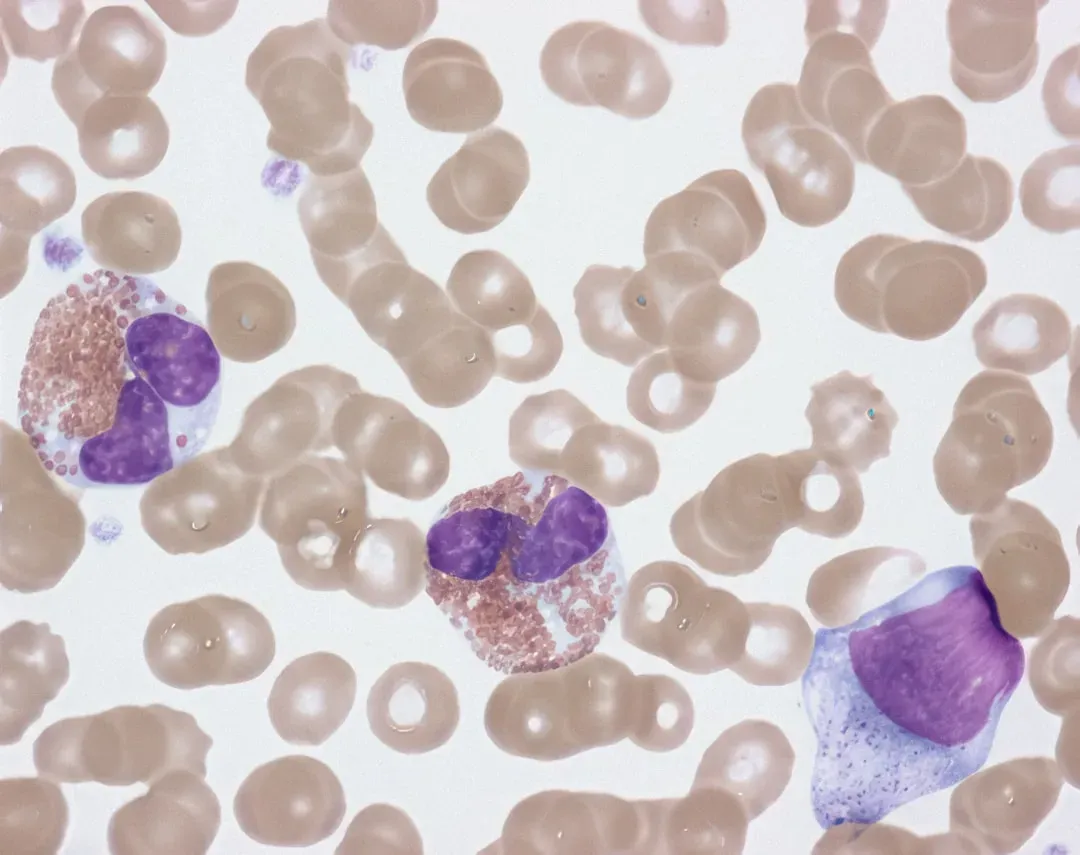
One of the most fascinating aging villains is the senescent cell: a cell that has stopped dividing but stubbornly hangs around, secreting inflammatory and tissue-disrupting molecules. These have been nicknamed “zombie cells” because they are not fully alive in the usual sense but refuse to quietly disappear. As we get older, these cells accumulate in tissues like fat, cartilage, blood vessels, and even the brain, nudging nearby healthy cells into dysfunction. It is like having a few toxic coworkers in an office poisoning the workplace mood day after day.
In mice, drugs called senolytics – which selectively kill senescent cells – have shown striking results, improving physical function and extending healthy lifespan in some experiments. That has launched a wave of early human trials, targeting conditions like osteoarthritis, lung fibrosis, and age-related frailty. Still, clearing senescent cells in humans is not yet a proven fountain of youth; there are open questions about long‑term safety, proper dosing, and which patients truly benefit. But if senolytics pan out, they would be one of the clearest examples of directly modifying a core aging mechanism instead of just treating a downstream disease.
Metabolism, Calories, and the Longevity Signaling Pathways

For decades, one of the most robust lifespan‑extending interventions in animals has been some version of eating less – usually called caloric restriction. From worms to mice, reducing calorie intake without causing malnutrition can extend lifespan and delay age-related diseases. The point is not to starve yourself, but to signal to the body that times are lean, prompting it to flip into a more protective, repair-focused mode. You can think of it as going from “growth and spend” to “maintenance and savings” in metabolic terms.
Researchers have identified several nutrient-sensing pathways – such as mTOR, AMPK, and sirtuins – that appear to act like master switches for this maintenance mode. Drugs like rapamycin (which inhibits mTOR) and compounds that activate sirtuins have extended lifespan in multiple animal models, sometimes quite dramatically. Human data is still mixed and early; rapamycin, for example, is approved for specific medical uses and carries non-trivial side effects. Here’s where we have to be careful: the biology is exciting, but copying high-dose mouse protocols in healthy humans is not smart. A more grounded approach uses these findings to refine how we eat and live, rather than chasing a magic pill.
Can Lifestyle Really Slow Aging, Or Is That Just Wellness Marketing?

It is easy to roll your eyes at advice like “eat well, move more, sleep better,” but in longevity science, those boring basics keep showing up as the heavy hitters. Regular physical activity does far more than burn calories; it boosts mitochondrial function, improves insulin sensitivity, reduces chronic inflammation, and helps preserve muscle and brain health with age. I have personally seen older adults who lift weights and walk daily move with a lightness that some people in their thirties have already lost. It is not glamorous, but it is powerful biology in action.
Nutrition tells a similar story. Diets rich in whole foods, fiber, healthy fats, and a wide variety of plants are consistently linked with better aging outcomes, from heart health to cognitive function. Sleep and stress management, too, have concrete physiological footprints, shaping hormone levels, immune function, and how well our cells repair nightly damage. None of this guarantees an extra decade of life, but it heavily influences whether later years are marked by independence or constant medical crisis. Lifestyle is not a side dish in the longevity conversation; it is the main course that all the fancy interventions get layered on top of.
Longevity Drugs, Supplements, and the Biohacking Hype
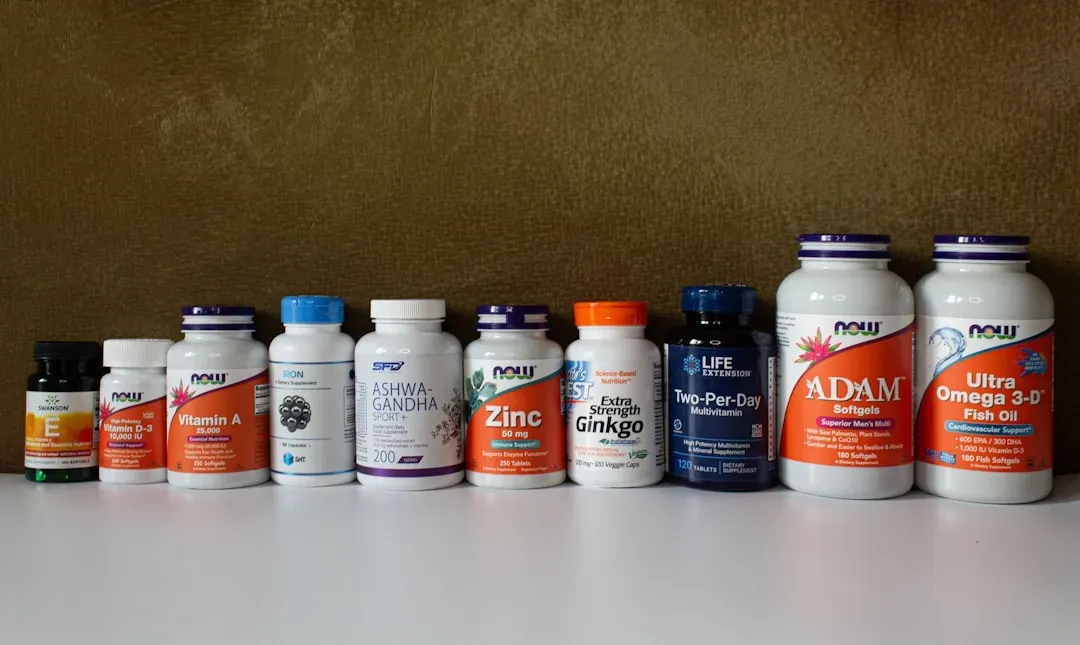
In the last few years, there has been an explosion of interest in potential “longevity molecules” such as metformin, rapamycin, NAD+ boosters, and various plant compounds. Some of these have promising animal data and reasonable mechanistic explanations, especially around improving metabolic health or supporting cellular repair pathways. Others are riding mostly on anecdotes, marketing, and very thin human data. The supplement aisle can feel like a casino: lots of bright lights, a few chances to win, and a serious risk of walking out lighter in the wallet.
From a scientific standpoint, the most honest position right now is cautious curiosity. A few drugs originally developed for other conditions, like metformin for diabetes, are being studied in large human trials to see if they actually delay age‑related diseases when used preventively. That is a big shift: targeting aging itself instead of treating each disease separately. But until results come in, self‑experimentation with unproven stacks is more of a gamble than a guaranteed edge. If you are going to experiment at all, it should be with medical supervision, conservative dosing, and a clear understanding that lifestyle will almost always deliver a safer and more reliable return on investment than any capsule.
Regenerative Medicine and the Talk of “Reversing” Aging
Some of the boldest claims in aging research today revolve around regeneration: restoring youthful function to old tissues. Stem cell therapies aim to replenish or support exhausted cell populations in organs like the heart or joints. Even more radical are approaches using partial cellular reprogramming, where old cells are nudged back toward a younger state by briefly activating certain developmental genes. In animals, carefully controlled versions of this have rejuvenated specific tissues and improved function, which understandably has everyone’s attention.
But here is the catch: full reprogramming turns cells into a sort of stem-like state and can easily trigger cancer or wipe out tissue identity, so there is almost no room for error. Most of what you hear about “reversing aging” is either oversimplified or taken from early-stage lab work that may never translate cleanly to humans. What is more realistic in the near term is targeted regenerative medicine for particular problems – like joint degeneration or damaged heart muscle – rather than whole‑body age reversal. The long‑term vision is thrilling, but it is a marathon of careful safety testing, not a quick sprint to eternal youth.
So, A Clear‑Eyed Opinion

Here is where I land: yes, we absolutely can slow aspects of aging, but not in the magical, movie-style way many people secretly hope for. The strongest evidence right now supports something a little less dramatic but far more achievable: significantly extending healthspan – the number of years you stay functional, clear‑minded, and independent – even if maximum lifespan only nudges upward. In practice, that means fewer years spent battling multiple chronic diseases and more years where you can hike, laugh, work, travel, and enjoy the people you love. That is not immortality, but it is a profound upgrade in quality of life.
At the same time, we should be honest: most of the dramatic breakthroughs people post about online are still early, fragile, or only proven in animals. It is tempting to chase the newest pill or injection while ignoring the unsexy basics that actually move the needle for almost everyone. My own bias is to treat frontier longevity science as a bonus layer, not the foundation: nail your sleep, movement, food, relationships, and mental health first, then cautiously consider advanced interventions as the evidence matures. If we treat aging as a system we can influence – but not yet fully control – we stay both hopeful and grounded. And maybe the real question is not “How long can I live?” but “How much of my life can I live fully?”




