There is something quietly radical about the idea that your thoughts, your worries, your deepest fears and your most joyful moments are not just events in your head. They are events in your body too. Every flicker of emotion sets off a cascade of chemistry, hormones, and nerve signals that ripple through your organs, your blood, your immune cells. Most of us were never taught this. We were raised to think of the mind as something separate, hovering somewhere above the shoulders, disconnected from the flesh and blood below.
Science, however, has been building a very different picture for decades. The link between mental life and physical health is not soft or speculative anymore. It is measurable, documented, and increasingly impossible to ignore. If you have ever felt your stomach drop with anxiety or noticed your heart lift with excitement, you already know something that researchers are still trying to fully map. Let’s dive in.
Two Systems, One Body: The Science Behind the Connection

We talk about the mind and body like they are separate all the time. But they are not. They have evolved to work together as one system, constantly feeding back into each other. Think of it like a conversation happening inside you, around the clock, that you are barely even aware of. Every mental state has a physical partner, and every physical state has a mental echo.
The mind-body connection involves the dynamic relationship between mental processes and physical health. It refers to the complex interactions between psychological states, physiological processes, and neural activities and how these impact health and behavior. In simple language, it is about how thoughts, emotions, and behaviors influence bodily functions, and vice versa. That two-way street is what makes this topic so compelling. You are not just a passenger in your body. You are also, in many ways, its architect.
A History as Old as Healing Itself

Although the understanding that emotions affect physical health dates as far back as the second-century physician Galen and the medieval physician and philosopher Moses Maimonides, modern medicine has largely continued to treat the mind and body as two separate entities. For centuries, healers knew what laboratories are only now confirming. Honestly, it makes you wonder how much time was lost by keeping these two worlds apart.
Most ancient healing practices, such as traditional Chinese medicine and Indian Ayurvedic medicine, have long held that the mind and body are closely linked. Modern science is bringing a new perspective to this connection. Today, the field of integrative medicine is working to bridge that ancient wisdom with hard data. In the medical field, this approach is known as integrative medicine, a type of healthcare that seeks to treat the whole person, not just the person’s disease or condition. It involves evidence-informed approaches to managing mental factors such as stress and anxiety that can impact other aspects of health, including disease symptoms.
Stress: The Silent Physical Saboteur
When you perceive a threat or stressor, the brain activates the “fight-or-flight” response, releasing stress hormones like cortisol and adrenaline. While this response is essential for survival, chronic stress can have detrimental effects on your health, including increased risk of heart disease, weakened immune function, and mental health disorders. Here is the thing, your body does not distinguish between a lion chasing you and a difficult email from your boss. To your nervous system, a threat is a threat.
Mental and emotional stress often presents as anxiety, irritability, restlessness, racing thoughts, overwhelm, constant worrying, or difficulty concentrating. Physically, stress can lead to symptoms such as muscle tension, headaches, fatigue, sleep disturbances, and changes in appetite. Chronic stress can even contribute to more serious health issues like hypertension, cardiovascular problems, and compromised immune function. The picture it paints is stark. Prolonged stress is not just uncomfortable. It is genuinely dangerous.
Psychoneuroimmunology: When Your Thoughts Talk to Your Immune Cells

Psychoneuroimmunology, also referred to as psychoendoneuroimmunology or psychoneuroendocrinoimmunology, is the study of the interaction between psychological processes and the nervous and immune systems of the human body. It is a subfield of psychosomatic medicine. It takes an interdisciplinary approach, incorporating psychology, neuroscience, immunology, physiology, genetics, pharmacology, molecular biology, psychiatry, behavioral medicine, infectious diseases, endocrinology, and rheumatology. It sounds impossibly complex, but its core message is simple: your mental life and your immune system are in constant dialogue.
Research has shown that distress can slow wound healing, diminish the strength of immune responses to vaccines, enhance susceptibility to infectious agents, and reactivate latent viruses. Moreover, stress and depression can also substantially augment the production of proinflammatory cytokines that are associated with a spectrum of age-related diseases. Let that sink in for a moment. Your mindset can influence how well a vaccine works inside you. That is not a metaphor. That is biology.
The Astonishing Power of the Placebo Effect

The idea that your brain can convince your body that a fake treatment is the real thing, the so-called placebo effect, and thus stimulate healing has been around for millennia. Now science has found that under the right circumstances, a placebo can be just as effective as traditional treatments. A sugar pill making pain disappear. A saline injection calming inflammation. It sounds like magic, but it is neuroscience in action. Your expectation becomes a physiological event.
How the placebo effect works is still not fully understood. Researchers believe it involves a complex neurobiological reaction that increases feel-good neurotransmitters, like endorphins, serotonin, and dopamine, and greater activity in specific brain regions linked to mood, emotional responses, and self-awareness. While the placebo effect demonstrates how positive expectations can lead to improvements in symptoms, even when the treatment is inactive, the nocebo effect shows the other side of this phenomenon. In other words, your thoughts can heal you. They can also, if dark enough, hurt you.
Neuroplasticity: Your Brain Can Literally Rewire Itself
Neuroplasticity refers to the brain’s ability to change and adapt. Positive thought patterns can rewire neural pathways, fostering better physical and mental health outcomes over time. Imagine your brain as a city of roads. Every time you think a thought or feel an emotion, you are either driving down an existing road or slowly carving out a new one. Repeat a thought often enough and that road becomes a highway. This is not self-help. This is neuroscience.
Research has shown that mindfulness and meditation induce neuroplasticity, increase cortical thickness, reduce amygdala reactivity, and improve brain connectivity and neurotransmitter levels, leading to improved emotional regulation, cognitive function, and stress resilience. Applying the principles of these findings in everyday life means cultivating positive expectations and consciously reshaping belief systems. Techniques from cognitive behavioral therapy, for instance, can be instrumental in reframing negative thought patterns to enhance the brain’s plasticity and adaptability, fostering new, healthier patterns of thinking and behavior.
The Gut-Brain Axis: Your Second Brain Is in Your Belly
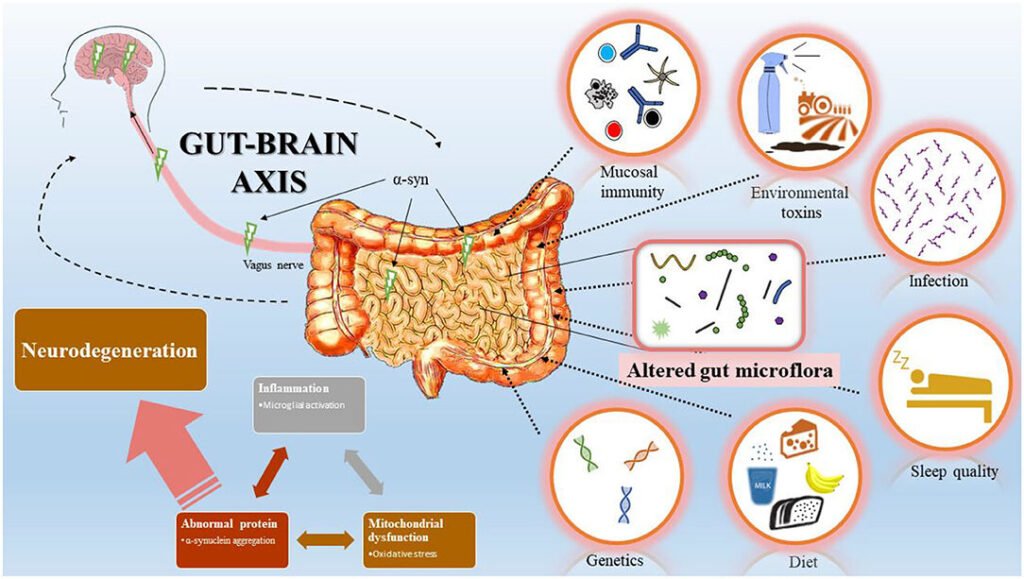
Mindfulness, a scientifically supported strategy for managing anxiety, has shown promise in improving both physical and mental health. Its benefits may be partly explained through its effects on the gut-brain axis, a bidirectional communication link between the gastrointestinal system and the central nervous system. Here is something I find genuinely mind-bending: your gut sends more signals to your brain than your brain sends to your gut. That tight feeling in your stomach before a job interview is your second brain talking back.
Stress is a well-known aggravator of gut dysfunction, impacting gut motility, barrier function, and the microbiome. Meditation, through its stress-reducing effects, can positively influence gut health by modulating these stress-related changes. It helps to restore the balance of gut bacteria, improving gut barrier function and reducing inflammation. Tibetan Buddhist monks who practiced daily meditation for years showed a gut microbiome composition that might promote anti-inflammatory pathways and better metabolism, along with lower levels of cardiovascular disease markers. A calmer mind, it seems, makes for a healthier gut.
Harnessing the Connection: Practical Tools That Actually Work

Science has validated that positive mind-training practices like meditation, mindfulness, and cognitive-behavioral therapy can reduce stress, alleviate symptoms of anxiety and depression, and even enhance the body’s immune response. These are not fringe ideas anymore. They are evidence-backed tools that hospitals, clinics, and mental health practitioners are integrating into mainstream care right now, in 2026.
New research is informing how mindfulness meditation contributes to improvements in cognitive health and may have relevance to treating a range of degenerative brain conditions. A study published in the journal Proceedings of the National Academy of Sciences applied novel neuroimaging methods to evaluate how focused-attention mindfulness meditation affects the flow of fluids within the brain, finding that meditation may serve as a noninvasive way to stimulate fluid circulation and removal of harmful proteins in a manner similar to sleep. Think about that the next time someone dismisses meditation as simply sitting quietly. It is doing cleaning work inside your brain while you breathe.
Conclusion: Your Mind Is Not Just in Your Head

The mind-body connection is not a soft concept for wellness blogs and yoga retreats. It is one of the most compelling areas of modern science, backed by decades of research from immunologists, neurologists, and psychologists working together to understand how the human system actually operates. Your thoughts are biological events. Your emotions are chemical signals. Your fears, your hope, your gratitude, your chronic worry: all of them are writing instructions to your body every single moment of every day.
The good news is that this works in both directions. It is not possible to wish cancer away or think hard enough to make diabetes disappear, but it is possible to manage your thoughts and train your mind to develop a more intentional focus. By doing so, you can address worries and even create new pathways in your brain that help you experience less stress and anger. Experiencing fewer negative thoughts and emotions makes room for a more positive mindset and more meaningful actions, all of which can facilitate healthy habits, ease the burden of disease on your body, and make your overall quality of life better. That is not a small thing. That is actually everything.
So here is the question worth sitting with today: if your thoughts are shaping your health right now, what kind of health are you quietly building? What do you think? Tell us in the comments.




