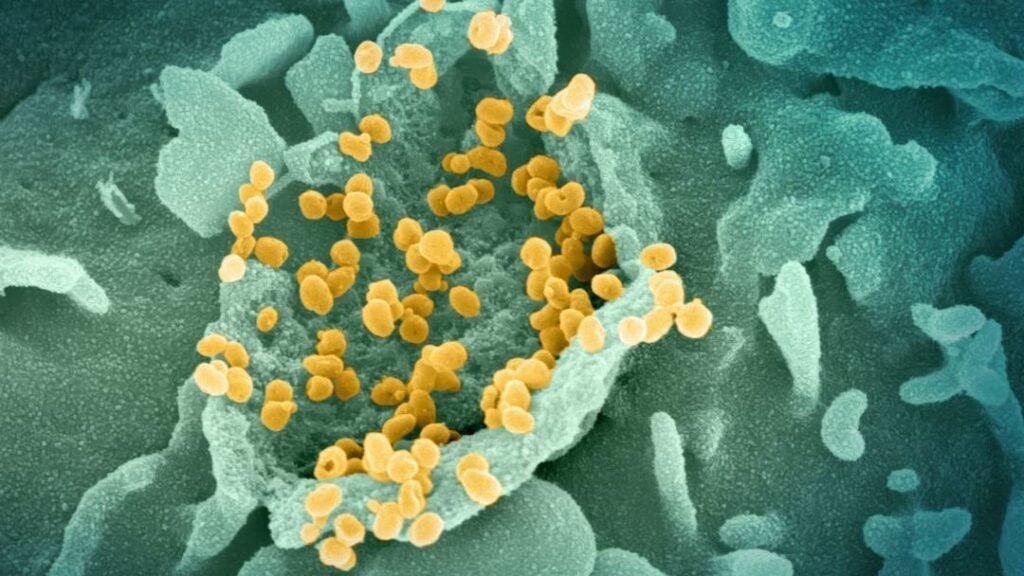
Your body is, honestly, one of the most sophisticated defense machines ever conceived. Every single second of every day, without your conscious permission, it is waging war against invaders you cannot see. Bacteria. Viruses. Rogue cells. Fungi. The sheer volume of threats your body handles silently – while you make coffee or scroll your phone – is staggering.
Yet most people only think about their immune system when something goes wrong. A nasty cold. A lingering infection. And that is a shame, because the layers of protection built into your biology deserve far more appreciation. From the surface of your skin to the deepest corridors of your gut, your body has hidden defense systems that are breathtakingly complex. Ready to be amazed? Let’s dive in.
Your Skin: The Fortress You Never Think About
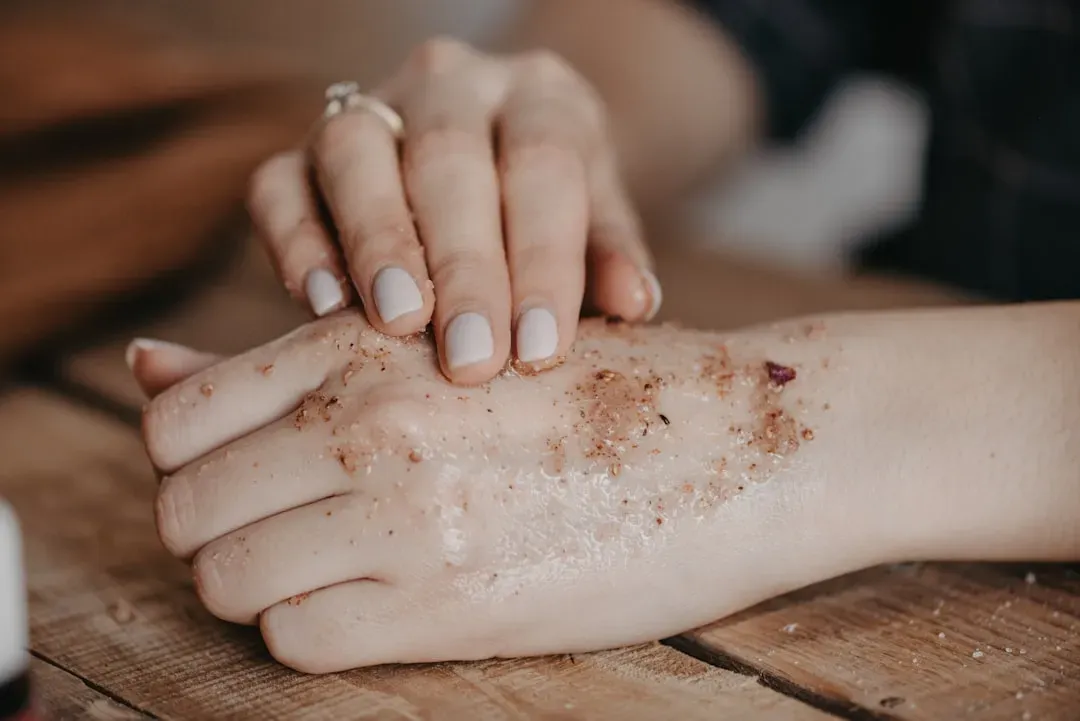
You probably think of your skin mostly in terms of appearance. Here’s the thing, though – it is your single most important physical shield against the outside world. Your skin is the outermost barrier of your organism, and scientists’ view of it has evolved dramatically: from being seen as an inert mechanical wall to being recognized as an active organ that can sense danger signals and mount perfectly adapted defense responses against invading pathogens.
The skin is the primary barrier to the entrance of microorganisms into your body. Not only is it covered with a layer of dead, keratinized epithelium that is too dry for most bacteria to grow in, but as these cells are continuously shed from the surface, they carry bacteria and other pathogens away with them. Think of it like a constant, silent self-cleaning system running 24 hours a day.
Your skin also has tight junctions that block pathogen entry and antimicrobial peptides – like cathelicidins and beta-defensins – that are activated by proteolytic cleavage and combat pathogens in a variety of ways. Even the pH of your skin surface is strategically hostile to most invaders. You carry around your own chemical defense shield, and you never had to ask for it.
Mucous Membranes and Chemical Traps: The Second Gate
Once past the skin, your body still has extraordinary backup systems ready to stop pathogens in their tracks. Your natural barriers include the skin, mucous membranes, tears, earwax, mucus, and even stomach acid. These are not passive walls – they are active, chemically aggressive environments designed to kill anything that does not belong.
Typically, mucous membranes are coated with secretions that actively fight microorganisms. For example, the mucous membranes of your eyes are bathed in tears, which contain an enzyme called lysozyme that attacks bacteria and helps protect your eyes from infection. That tiny teardrop rolling down your face during a sad movie? It is also a bactericidal weapon. I find that remarkably poetic, honestly.
Your digestive tract has a series of powerful barriers, including stomach acid, pancreatic enzymes, bile, and intestinal secretions – all substances capable of killing bacteria or preventing them from multiplying. In your upper respiratory tract, ciliated epithelial cells move potentially contaminated mucus upward to the mouth, where it is then swallowed into the harsh acidic environment of the stomach. Your body is essentially recycling threats into harmlessness, continuously.
The Innate Immune System: Your Body’s Rapid Response Force
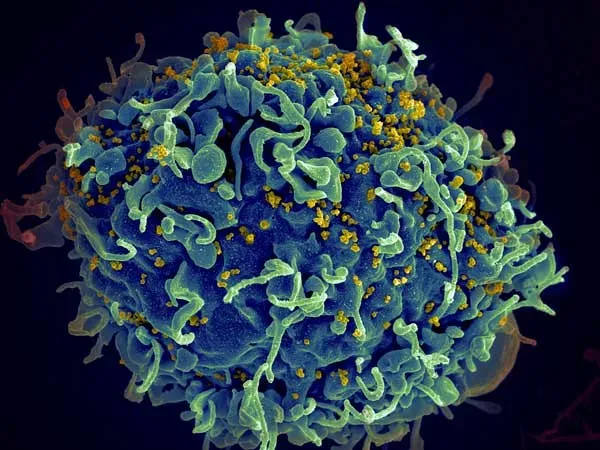
When pathogens breach your barriers, the response that fires up first is breathtakingly fast. The innate immune system is your body’s first internal line of defense against intruders. It responds in the same way to all germs and foreign substances – which is why it is sometimes called the non-specific immune system – and it acts very quickly, making sure that bacteria that have entered through a small wound are detected and destroyed on the spot within hours.
The innate immune system utilizes pattern recognition receptors – like Toll-like receptors – to detect pathogens and initiate rapid response mechanisms. Think of these receptors like molecular bouncers stationed at every door, trained to recognize the “wrong kind” of molecular ID badge. Macrophages and neutrophils of the innate immune system provide this first line of defense against many common microorganisms and are essential for the control of common bacterial infections.
Neutrophils arrive first and can even produce fibers to physically trap microbes, while macrophages phagocytose – meaning they engulf and digest – enormous numbers of invaders. Macrophages hunt for microbes and damaged cells, almost like a biological Pac-Man. It sounds almost too simple to be real, but that is what is happening inside your bloodstream right now.
Fever and Inflammation: Pain With a Purpose

Most people reach for fever-reducing medicine the moment their temperature climbs. That instinct is understandable. But here is the fascinating part: your fever is not the enemy – it is your body fighting back on your behalf. Body temperature increases as a protective response to infection and injury. An elevated body temperature enhances your body’s defense mechanisms, although it can certainly cause discomfort.
Cytokines increase your core body temperature, causing a fever. Those elevated temperatures inhibit the growth of pathogens and speed up cellular repair processes. For these reasons, suppression of fevers should generally be limited to those that are dangerously high. Mild fevers, it turns out, are your body’s fever dream of a defense strategy – literally.
Inflammation is a response triggered by a cascade of chemical mediators that occurs when pathogens successfully breach the innate immune system or when an injury occurs. Although inflammation is often perceived as a purely negative consequence, it is actually a necessary process that recruits cellular defenses needed to eliminate pathogens, remove damaged cells, and initiate repair mechanisms. It is, in short, constructive chaos. If inflammation is not properly controlled, the immune system stays on high alert – leading to chronic inflammation that can damage organs and tissues and may contribute to conditions like asthma and cardiovascular disease. The balance matters enormously.
The Adaptive Immune System: Your Body’s Genius Memory
If the innate system is your body’s rapid response unit, the adaptive immune system is your long-term strategic command. It is slower, yes. More deliberate. The adaptive immune system is slower to respond than the innate system but far more accurate, and it has the extraordinary advantage of being able to remember germs – so the next time it faces a pathogen it has already met, it can start fighting it faster.
Unlike the innate immune system, which is pre-programmed to react to broad categories of pathogen, your adaptive immune system is highly specific to each particular pathogen your body has encountered. It creates immunological memory after an initial response, leading to an enhanced reaction in future encounters. This is the biological principle behind vaccines – and it is genuinely brilliant when you think about it.
Your body carries roughly two trillion lymphocytes, which represent twenty to forty percent of all white blood cells, with a total mass roughly equivalent to that of the brain or liver. That is an army of almost incomprehensible scale, quietly patrolling your entire body at all times. Effective immune defense against viruses relies on the coordinated actions of both the innate immune system and B and T cells, with T cells playing pivotal roles not only in eliminating established infections but also in stopping viral replication without relying on antibodies.
Regulatory T Cells: The Immune System’s Internal Security Guards
Here is where things get truly mind-blowing. Your immune system is powerful enough to destroy almost anything – but that same power, turned inward, could destroy you. So how does it know when to stop? The answer earned scientists the Nobel Prize in 2025. Mary E. Brunkow, Fred Ramsdell and Shimon Sakaguchi were awarded the Nobel Prize in Physiology or Medicine 2025 for their groundbreaking discoveries concerning peripheral immune tolerance – the mechanism that prevents the immune system from harming your own body – discoveries that have laid the foundation for a new field of research and spurred the development of new treatments for cancer and autoimmune diseases.
Sakaguchi’s 1995 discovery of a new class of immune cells called regulatory T cells, or Tregs, revealed another layer of protection called peripheral tolerance. These cells act as security guards of the immune system, patrolling your body and suppressing rogue immune responses that could lead to autoimmunity. Without them, your immune system would essentially tear itself apart. These cells prevent other T cells from mistakenly attacking your own tissue, and they also ensure the immune system calms down after it has eliminated an invader, so it does not continue working at full intensity.
A single signaling pathway controls whether immune cells attack or befriend cells they encounter while patrolling your body. Manipulating this pathway could allow researchers to toggle the immune response to treat many types of diseases, including cancers, autoimmune disorders, and those requiring organ transplants. It is hard to say for sure exactly when clinical applications will be fully realized, but the trajectory is extraordinary.
Your Gut Microbiome: The Hidden Army Within
Perhaps the most surprising discovery in modern immunology is just how much your gut bacteria determine your immune health. With roughly seventy to eighty percent of immune cells present in the gut, there is an intricate interplay between your intestinal microbiota, the intestinal epithelial layer, and the local mucosal immune system. Your digestive tract is not just processing food – it is running immune command operations.
Your gut microbiome plays a crucial role in regulating immune responses, influencing your susceptibility to viral infections, shaping disease progression, and its outcomes. Emerging research demonstrates that dysbiosis – an imbalance in your gut microbial communities – can compromise your antiviral defenses, while a balanced microbiome enhances immune resilience. This is why what you eat matters far more than just your waistline.
The intestinal microbiota has a pervasive influence on innate immunity, fortifying your defenses against infection in tissues throughout your entire body. The microbiota plays a fundamental role in the induction, training, and function of your immune system. In return, the immune system has largely evolved as a means to maintain this symbiotic relationship with diverse and evolving microbes. When operating optimally, this immune system and microbiota alliance allows the induction of protective responses to pathogens and the maintenance of regulatory pathways involved in tolerance to harmless antigens.
Conclusion: A Defense System More Powerful Than You Imagined
Your body is not waiting for you to get sick before it acts. Right now, your skin is shedding pathogens, your mucus is trapping invaders, your macrophages are hunting down bacteria, your T cells are memorizing every threat they encounter, your regulatory T cells are keeping the whole system from going haywire, and your gut microbiome is training your immune forces from the inside. All of it. Simultaneously. Without your awareness.
The 2025 Nobel Prize in Medicine brought well-deserved global attention to just how sophisticated – and still mysterious – these systems truly are. Continuing to unlock the secrets of immune regulation could lead to a future where the immune system can be precisely tuned like a thermostat – turned down in autoimmunity or revved up against cancer. That future is closer than many people realize.
The body you live in is extraordinary. Not because it never fails – it does, sometimes. Rather, it is extraordinary because of how rarely it fails, given everything it quietly faces. The next time you brush off a minor cold or recover from an infection faster than expected, consider what really happened. Your hidden defenses did their job, and they did it brilliantly. So, what part of your body’s hidden defense system surprised you the most?