is often reduced to a neat diagram in a textbook: four chambers, arteries in red, veins in blue. In reality, it is a restless, humming engine of biology and electricity that scientists are still struggling to fully understand. Every beat is a negotiation between genes, environment, emotions, and even the time of day. Researchers are now mapping the heart with the same intensity once reserved for the brain, uncovering surprises in how it repairs, fails, and adapts. The more closely we look, the less it seems like a simple pump and the more it resembles a living ecosystem packed into a fist-sized space.
The Heart That Never Rests
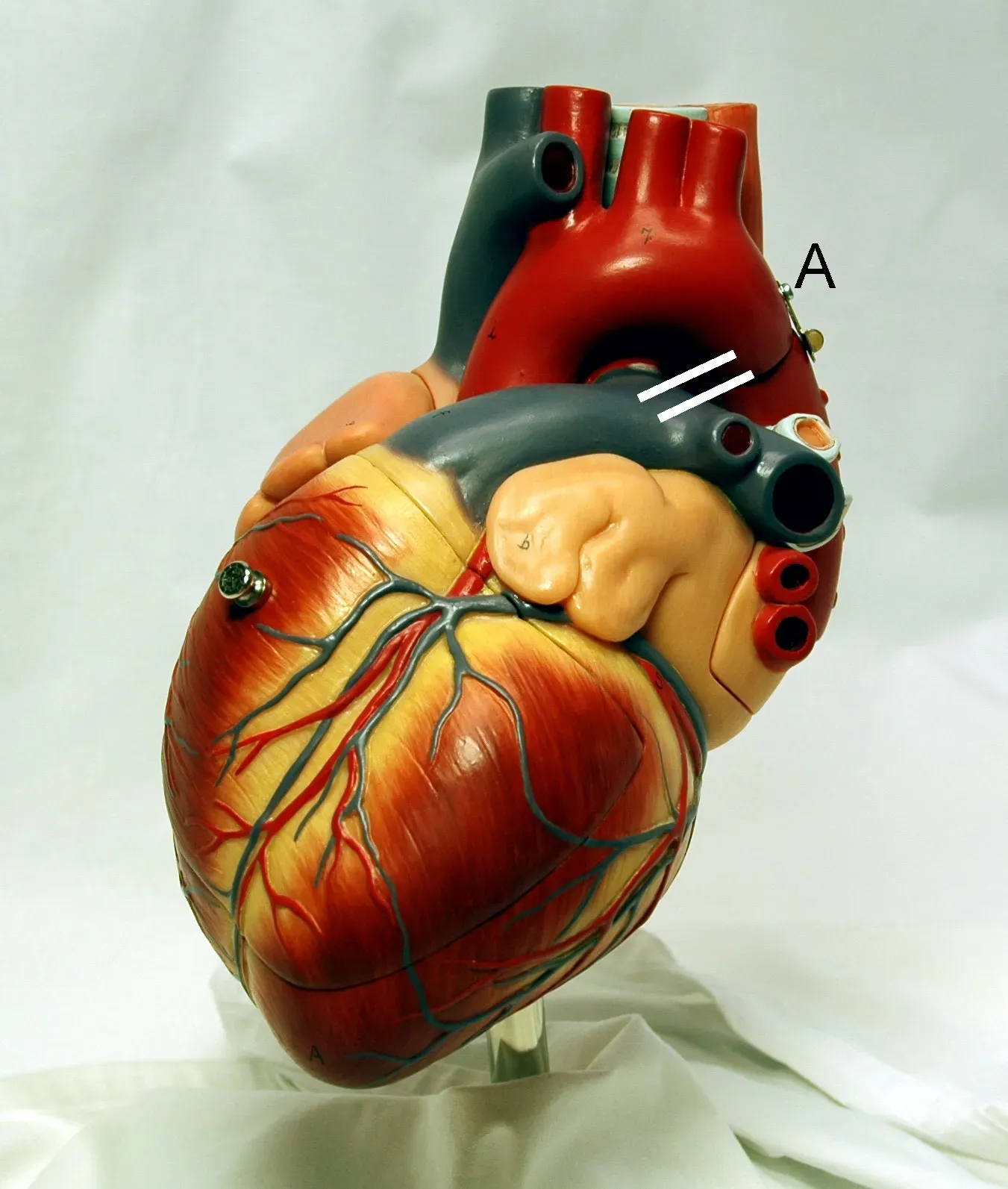
Imagine an engine that starts before you are born and, if all goes well, runs non‑stop for decades without a single scheduled shutdown. That is your heart: by the time you blow out the candles on your thirtieth birthday cake, it has already beaten more than a billion times. Each minute, it sends blood racing through a network of vessels so long it could wrap around the planet multiple times, delivering oxygen and nutrients with astonishing precision. This relentless work feels effortless only because the heart’s muscle cells are exquisitely specialized to contract in perfect synchrony. Behind the quiet thump in your chest is an enormous amount of coordinated microscopic labor.
Physiologists calculate that over an average lifetime, the heart pumps enough blood to fill multiple Olympic‑sized swimming pools, a mental image that makes a single skipped beat feel suddenly dramatic instead of trivial. To keep this up, cardiac cells are packed with mitochondria, the tiny power plants of the cell, far more densely than most other tissues in the body. That energy demand is one reason why even a brief interruption in blood flow during a heart attack can cause lasting damage. The heart’s apparent simplicity hides a delicate dependence on constant fuel, oxygen, and timing that has to be maintained every moment you are alive.
An Electrical Storm in Your Chest
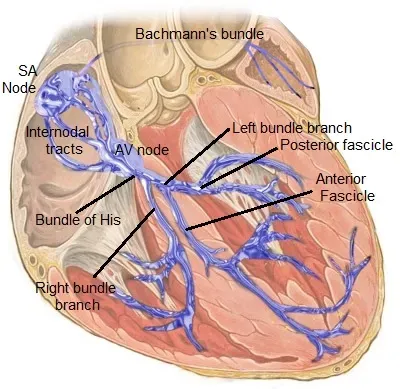
Every heartbeat begins not with muscle, but with electricity. Deep in the right atrium, a small cluster of cells called the sinoatrial node quietly generates rhythmic electrical impulses, acting as the body’s natural pacemaker. These signals travel in carefully choreographed waves through the heart’s wiring system, telling each chamber exactly when to contract. If you have ever seen an electrocardiogram on a hospital monitor, those spiky lines are the visible trace of this internal lightning show. When the timing is precise, the heart’s four chambers act like a well‑rehearsed team passing blood from one to the next with minimal backflow.
Problems start when that electrical system falters, something doctors call arrhythmia. Sometimes the misfire is brief and harmless, other times it can turn the heart’s usually organized contraction into chaotic quivering that can no longer move blood effectively. Modern cardiology has turned this invisible process into something treatable: pacemakers can overwrite faulty signals, and defibrillators can shock a failing heart back into a stable rhythm. There is a surprising elegance to the idea that a few milliamps of electricity, delivered at just the right instant, can restore order to an organ on the brink of collapse. It is a vivid reminder that the heart is as much an electrical machine as it is a mechanical pump.
Your Heart Has Its Own “Little Brain”
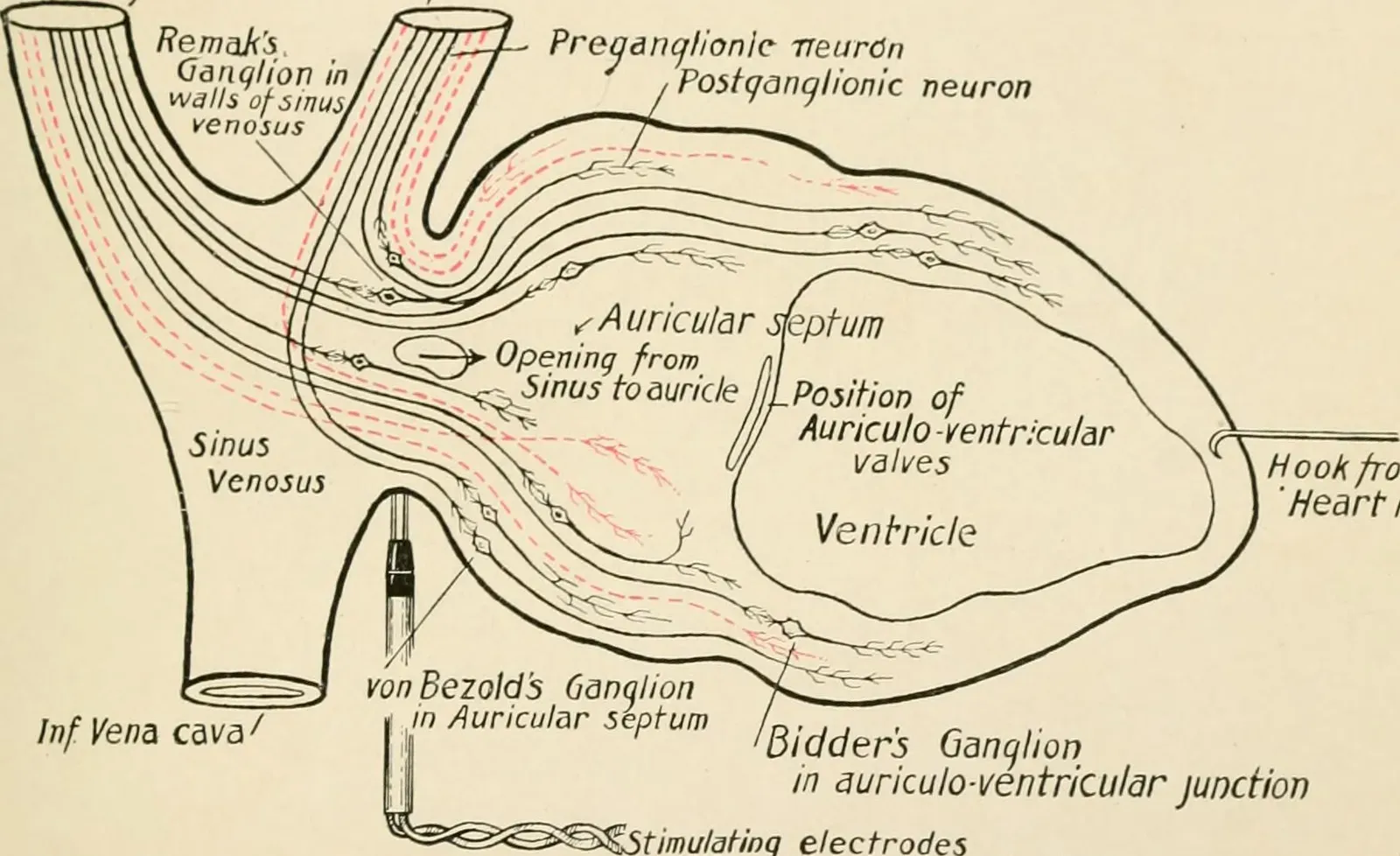
It is tempting to think of the heart as a passive servant of the brain, but that picture is only half true. Embedded in the heart’s tissue is its own dense network of neurons, sometimes nicknamed the cardiac “little brain.” This local nervous system helps fine‑tune heart rate, contraction strength, and response to changing demands faster than signals can travel from the brain and spinal cord. When you suddenly stand up, sprint, or get a fright, that local circuitry steps in instantly to stabilize blood flow before your conscious mind has even caught up. The heart, in other words, is not just listening to the brain; it is also making decisions on its own.
This autonomy has strange and sobering consequences. During organ transplantation, for example, a donor heart can be restarted in a recipient’s chest without any connection to the recipient’s nervous system, relying on its built‑in pacemaker and circuitry to keep beating. Researchers studying this cardiac “little brain” are uncovering how it may contribute to conditions like arrhythmias or even the way chronic stress reshapes heart function over time. It blurs the line between where the nervous system ends and the cardiovascular system begins. The idea that you carry a second, smaller decision‑making network in your chest makes the old metaphor of “thinking with your heart” feel a little less poetic and a little more literal.
The Heart Remembers Your Lifestyle
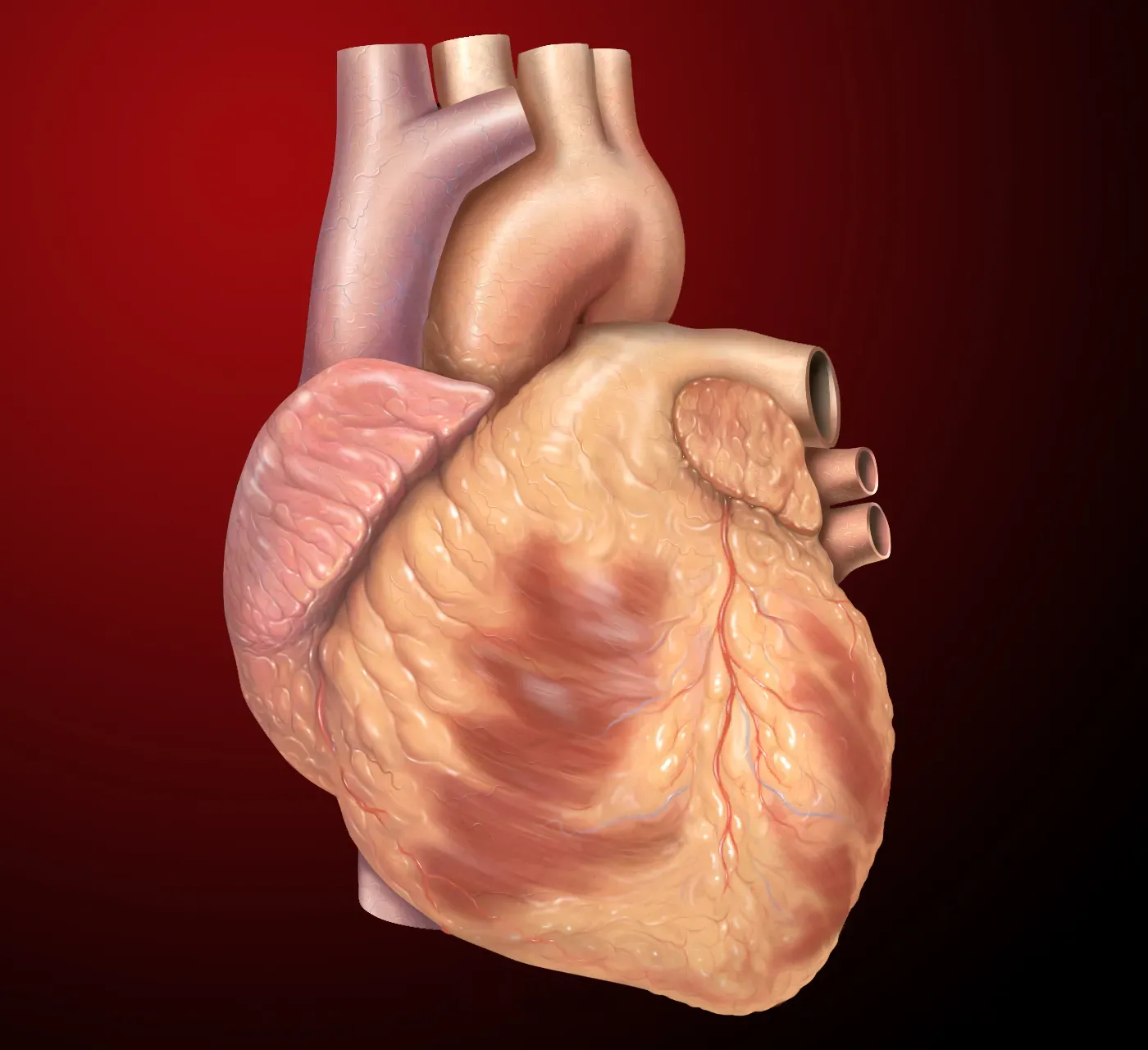
If you want to know how someone has lived, a cardiologist might argue you can often read it in their heart. Long‑term habits like smoking, high‑salt diets, or constant stress do not just cause temporary spikes in blood pressure or heart rate; they literally change the heart’s structure. Over years, the muscle walls can thicken, chambers can stretch, and delicate valves can begin to stiffen or leak. Physicians call some of these changes remodeling, a word borrowed from architecture that hints at how the organ is continuously rebuilding itself in response to the strains placed upon it. A heart that has spent decades under pressure simply looks and behaves differently from one that has not.
The flip side is just as important: positive habits leave physical fingerprints too. Regular aerobic exercise encourages the heart to grow slightly larger and more efficient, able to pump more blood with each beat so it can rest at a lower rate. Eating in a way that protects blood vessels from inflammation and plaque buildup helps preserve the flexibility of arteries that the heart depends on. Some large studies suggest that if people adopt healthier habits by midlife, they can significantly reduce their risk of heart failure and heart attack, even if they spent earlier years on a less‑than‑ideal path. In that sense, the heart is forgiving but not forgetful; it records your choices, but it also rewards course corrections.
The Hidden Clues Doctors Can Now Read
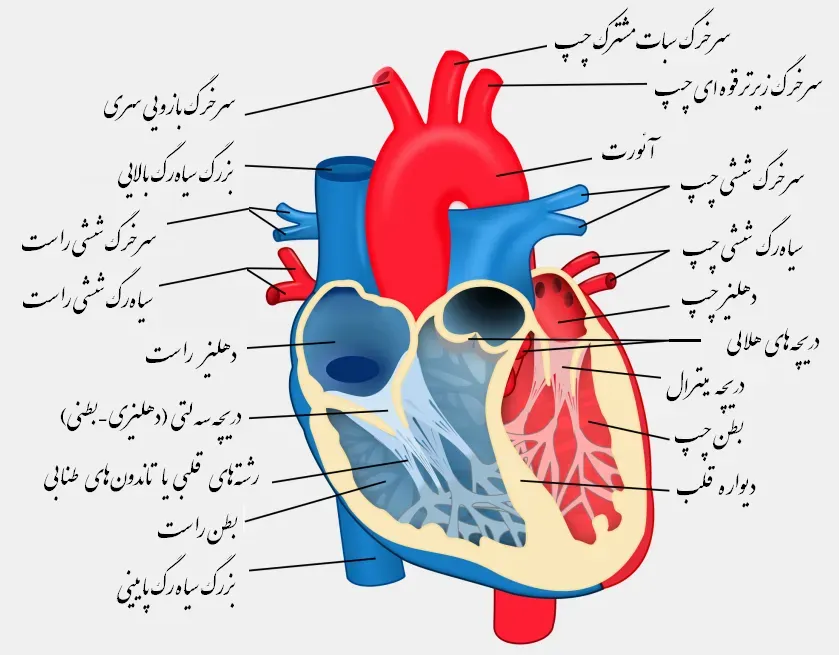
Modern cardiology has turned the heart into an open book for anyone who knows how to read the pages. Imaging technologies, from ultrasound to advanced magnetic resonance scans, can now track how blood flows through each chamber in real time. These tests reveal subtle leaks in valves, areas of weakened muscle, or scar tissue from silent heart attacks that a person might never have noticed. Blood tests add another layer, measuring chemical markers that rise when heart cells are stressed or damaged, sometimes hours before major symptoms appear. For doctors in emergency rooms, these hidden clues can mean the difference between catching a heart attack early and missing a narrow window for treatment.
Wearable devices have added a new, almost science‑fiction layer to this picture. Smartwatches and patches can continuously track heart rate, rhythm, and sometimes even detect irregular patterns that hint at conditions like atrial fibrillation. Some people discover dangerous arrhythmias only because a device on their wrist quietly flagged something unusual. While these gadgets are not perfect diagnostic tools, studies have shown they can be surprisingly good at spotting patterns that deserve a second look. In effect, they turn the pulse – once checked occasionally by a doctor with a hand on the wrist – into a continuous stream of data that can surface problems long before the first chest pain or fainting spell.
Why It Matters More Than You Think
Heart disease remains one of the leading causes of death worldwide, which alone would be reason enough to care about the biology beating inside your chest. But the story goes deeper than mortality statistics. The heart is tied into almost every other system you rely on: when it falters, the brain, kidneys, lungs, and even the immune system feel the impact. That is why people living with chronic heart conditions often describe a kind of whole‑body exhaustion that goes far beyond a single failing organ. It is not just about avoiding a dramatic heart attack; it is about preserving the quality of the ordinary days between medical crises.
Compared with diseases that attract more public attention, such as certain cancers or neurological disorders, cardiovascular problems can seem familiar and therefore strangely easy to ignore. Yet many of the major risks are modifiable through policy and personal action, from air pollution control to food access and urban design that encourages physical movement. Investing in heart health pays dividends across society: workplaces lose fewer days to illness, healthcare systems face less strain, and families experience fewer sudden, devastating losses. When we talk about taking care of the heart, we are really talking about protecting the engine of daily life for entire communities. That makes the science of the heart not just a medical issue, but a social and economic one as well.
The Future Landscape of Heart Science
The next decade of heart research is poised to be radically different from the last. Scientists are using gene‑editing tools to explore inherited forms of heart disease, hoping one day to correct faulty DNA before it can cause damage. Lab‑grown heart tissue, created from stem cells, is letting researchers test drugs on miniature beating models instead of relying solely on animal studies or risky first‑in‑human trials. Engineers are refining artificial hearts and ventricular assist devices so smaller, more reliable machines can support patients for longer while they wait for a transplant or even as a long‑term alternative. What once sounded like speculative fiction – wearable hearts or bioengineered patches that repair damaged muscle – is edging closer to clinical reality.
These advances come with serious challenges. Ethical questions around genetic editing, access to costly new therapies, and the risk of widening global health gaps are already being debated. There is also the practical challenge of turning complex, cutting‑edge tools into treatments that work safely outside elite research hospitals. Still, every new insight into how the heart grows, fails, and heals offers another lever to pull in the fight against cardiovascular disease. If the last century was about learning to reopen blocked arteries and manage blood pressure, the coming one may be about personalized, predictive care that prevents catastrophic events before they ever happen. The heart is becoming not just an object of treatment, but a system we can monitor, model, and, in some cases, redesign.
How You Can Listen to Your Own Heart
For all the high‑tech science swirling around cardiology, some of the most powerful tools for protecting your heart are deceptively simple. Paying attention to basic signals – shortness of breath on mild exertion, unusual fatigue, chest discomfort that feels more like pressure than pain – can prompt conversations with a doctor before problems escalate. Regular checkups that include blood pressure, cholesterol, and blood sugar testing give a quiet snapshot of how hard your heart is working behind the scenes. Small daily choices, from taking the stairs to choosing fiber‑rich foods and carving out time for real rest, gently nudge your cardiovascular system toward resilience. None of these actions feel dramatic in the moment, but they accumulate in the heart’s long memory.
There are also ways to support the broader scientific effort. Participating in clinical research, when appropriate and safe, helps doctors refine treatments and understand how well they work in diverse populations. Supporting organizations that fund heart research or advocate for healthier environments contributes to change at a scale no individual can manage alone. Even something as basic as learning your family history of heart disease and sharing it with your healthcare team can guide earlier screening and prevention. In a world where the heart is both a deeply personal organ and a major public health concern, individual awareness and collective action reinforce each other. The question is not just how long your heart will beat, but what kind of life you will build around those beats.

Suhail Ahmed is a passionate digital professional and nature enthusiast with over 8 years of experience in content strategy, SEO, web development, and digital operations. Alongside his freelance journey, Suhail actively contributes to nature and wildlife platforms like Discover Wildlife, where he channels his curiosity for the planet into engaging, educational storytelling.
With a strong background in managing digital ecosystems — from ecommerce stores and WordPress websites to social media and automation — Suhail merges technical precision with creative insight. His content reflects a rare balance: SEO-friendly yet deeply human, data-informed yet emotionally resonant.
Driven by a love for discovery and storytelling, Suhail believes in using digital platforms to amplify causes that matter — especially those protecting Earth’s biodiversity and inspiring sustainable living. Whether he’s managing online projects or crafting wildlife content, his goal remains the same: to inform, inspire, and leave a positive digital footprint.




