If you’ve ever sat in a hospital waiting room gripping your phone a little too tightly, you know how terrifying it can feel to wait for answers. The wild thing is: behind those closed doors, medicine in 2026 looks nothing like it did even ten years ago. Treatments that sounded like sci‑fi are now routine, diagnoses take minutes instead of weeks, and conditions that once meant a lifetime of decline are becoming manageable, sometimes even reversible.
Some of these breakthroughs are obvious headliners, like gene editing and cancer immunotherapy. Others are quieter but just as life‑changing, from AI algorithms that catch strokes while you sleep to simple injections that prevent HIV. I still remember when a close family friend was told to “just manage” chronic pain; today, the options they’d have look almost unrecognizable. Let’s dig into ten of the biggest medical shifts actually changing lives right now – not someday, not in theory, but today.
1. Gene Editing: From Incurable to Treatable
Not long ago, a genetic disease was basically a life sentence: doctors could treat symptoms, but not the underlying typo in your DNA. That has started to flip with CRISPR-based therapies and related gene-editing tools, which can directly correct or silence faulty genes inside a patient’s cells. In late 2023, regulators in the United States and Europe approved the first CRISPR therapy for sickle cell disease, and by 2025 patients with once‑crippling pain crises were reporting normal lives for the first time. It’s not perfect, it’s not cheap, and it’s not risk‑free – but it’s a fundamentally different category of medicine.
The real emotional punch hits when you look at what this means for families. Instead of watching a child gradually lose muscle because of a mutation, there’s the real possibility of intervening early and preserving function. Researchers are now testing in vivo gene editing (editing directly inside the body) for conditions like high cholesterol and certain forms of blindness. There’s plenty to debate – ethics, access, long‑term safety – but for people living with brutal inherited conditions, the fact that “nothing can be done” is finally no longer true.
2. Cancer Immunotherapy: Turning the Body Into Its Own Drug
For decades, cancer treatment mostly meant poisoning fast‑growing cells and hoping healthy tissue survived the hit. Immunotherapy changed the rules by teaching the immune system to recognize and attack tumors directly. Drugs known as checkpoint inhibitors, once experimental, are now standard treatment for several cancers, including melanoma and some lung cancers, and they’ve pushed survival times far beyond what older chemo regimens could offer. In certain blood cancers, CAR‑T therapies – where a patient’s own immune cells are engineered and reinfused – have led to complete remissions in people who had run out of options.
None of this is a magic bullet; some patients respond dramatically, others hardly at all, and the side effects can be intense. But the shift in mindset is enormous: instead of blasting everything, we’re trying to aim, to be specific, to harness natural defenses. Newer work is exploring off‑the‑shelf CAR‑T cells (so you don’t have to engineer each patient’s cells), personalized cancer vaccines based on tumor DNA, and combinations of immunotherapy with targeted drugs. For many people, cancer is still terrifying – but increasingly, it no longer feels like an automatic death sentence.
3. mRNA Vaccines and the New Age of Rapid Response
The world met mRNA vaccines during the COVID‑19 pandemic, but what looked like a one‑off miracle has quietly turned into a powerful platform. Unlike traditional vaccines that rely on weakened viruses or proteins grown in eggs or cells, mRNA vaccines simply deliver genetic instructions that teach your cells to build a harmless piece of the target. That’s why scientists could design COVID vaccine candidates within days of getting the virus’s genetic sequence, and why updated boosters can roll out quickly as variants change. Today, that same technology is being used to develop vaccines for influenza, RSV, and even some cancers.
One of the most exciting shifts is how fast we can now respond to new threats. Instead of needing years of lab work, we can potentially move from sequence to candidate vaccine in weeks, which matters a lot in a world where outbreaks spread globally in days. Researchers are also exploring mRNA for treatments beyond vaccines, like delivering instructions to produce missing proteins in rare diseases or to stimulate targeted immune responses against tumors. There are still questions about storage, cost, and long‑term use, but the idea that our “medicine” can be written like software code and updated on the fly is a completely different way of thinking about health defense.
4. AI in Diagnostics: When Algorithms Spot What Eyes Miss

Artificial intelligence in medicine used to sound like marketing hype: big promises, vague results. That’s changed fast as real, clinically validated tools have appeared in hospitals and clinics. AI systems can now read certain scans – like retinal images, mammograms, and chest X‑rays – with accuracy comparable to experienced specialists, and sometimes they catch patterns humans routinely overlook. In stroke care, AI tools can quickly flag blocked vessels on CT scans and alert stroke teams directly, shaving off precious minutes when brain tissue is dying.
What’s striking is that AI is moving beyond imaging. Algorithms that scan electronic health records are being used to predict who is at high risk of sepsis, heart failure, or dangerous medication interactions, sometimes hours before symptoms explode. To be clear, this isn’t some robot doctor replacing humans; when it works well, it’s more like a relentless assistant that never gets tired or distracted. There are big concerns – bias in training data, privacy, overreliance – but when an algorithm spots a silent tumor or flags a failing heart in time to intervene, the abstract debate becomes deeply personal.
5. GLP‑1 Drugs: Rethinking Obesity and Metabolic Disease

If you’ve noticed more conversations about new “weight loss injections,” you’re seeing one of the most disruptive shifts in metabolic medicine in decades. Drugs that mimic a hormone called GLP‑1 (and related molecules) were originally developed for type 2 diabetes but turned out to dramatically reduce appetite and improve blood sugar control. Newer versions, some targeting multiple pathways, have led to significant weight loss, better blood pressure, and improved cholesterol in many patients. For people who have struggled for years with diets and exercise alone, often while being blamed or shamed, this feels like someone finally admitting that biology plays a huge role.
These medications are also changing how doctors talk about obesity – from a supposed failure of willpower to a chronic, treatable disease influenced by hormones, genetics, environment, and brain signaling. Studies are showing benefits beyond the scale, like reducing the risk of heart attacks and kidney disease in high‑risk patients. The hard part? Access and affordability: in many places, the people who might benefit the most can’t get them covered or sustained. Still, the simple fact that we now have powerful, biologically targeted tools is reshaping the landscape for millions living with obesity and diabetes.
6. HIV Prevention and Treatment: From Fatal Illness to Managed Condition

There’s a surreal quality to comparing the early years of the HIV epidemic to the present. What was once a near‑certain death sentence is now, for many, a manageable chronic illness with near‑normal life expectancy – if they can access treatment. Modern antiretroviral therapy can suppress the virus to levels where it’s effectively undetectable in the blood, which also means it’s not sexually transmissible. That single fact has transformed intimate relationships, parenting decisions, and the level of stigma for people living with HIV who have reliable care.
On the prevention side, long‑acting injectable medications are quietly rewriting the rules. Instead of taking a daily pill for pre‑exposure prophylaxis (PrEP), some people can now get an injection every couple of months to dramatically reduce the chance of infection. There’s still a long way to go, especially in regions where access to testing and treatment is low, and where stigma remains brutal. But scientifically, we now have the tools to realistically talk about controlling, and in some communities nearly eliminating, new infections. That’s a sentence that would have sounded wildly optimistic a generation ago.
7. Regenerative Medicine and Organ Repair
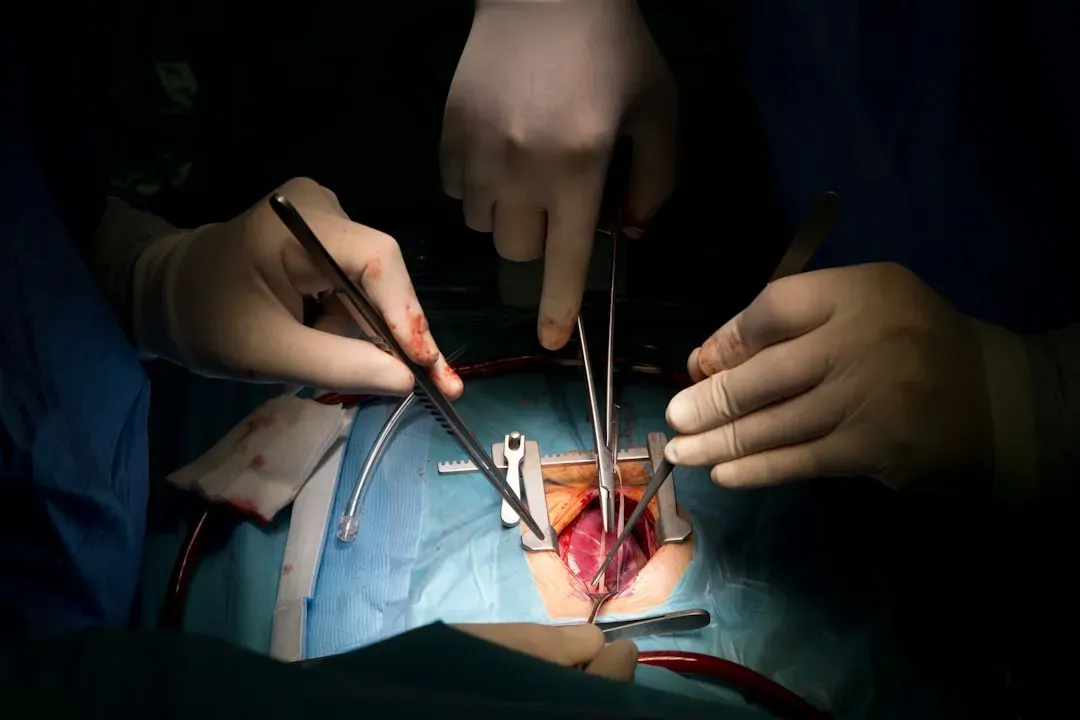
For most of modern medicine, when an organ failed badly enough, you either replaced it with a transplant or tried to work around it. Regenerative medicine is trying to rewrite that narrative by helping the body rebuild and repair its own tissues. Stem‑cell‑based therapies are being tested for conditions like spinal cord injury, heart damage after a heart attack, and degenerative eye diseases, with some patients showing regained function that would have been considered impossible not long ago. In orthopedics, techniques that use a patient’s own cells and scaffolds to regenerate cartilage and bone are already in clinical use in some centers.
Parallel to that, researchers are growing mini‑organs – organoids – in the lab that model human tissues and diseases. While these are not transplantable hearts or livers yet, they’re powerful tools for testing drugs and understanding what goes wrong at a cellular level. On the transplant front, efforts like 3D‑printed scaffolds seeded with cells and genetically modified animal organs are inching forward to address the brutal shortage of donor organs. The progress is uneven and sometimes overhyped, but when someone with severe heart damage can actually regain pumping function rather than just be told to wait for a transplant, it feels like the future has cracked open a bit early.
8. Precision Medicine: Matching the Right Drug to the Right Person

For most of history, medicine has quietly treated people like averages. You’d get the standard drug at the standard dose, and if it didn’t work, well, you were just unlucky. Precision medicine flips that by tailoring prevention and treatment based on an individual’s genetics, lifestyle, and environment. In cancer care, it’s become routine to sequence tumor DNA and pick therapies that specifically target its mutations, which means two people with “the same” cancer might receive very different drugs. This approach can improve effectiveness and reduce side effects by avoiding treatments that are unlikely to work for a particular person.
Outside oncology, pharmacogenomic testing is starting to guide which antidepressant, blood thinner, or pain medication is most likely to work safely for a given patient based on their genetic makeup. It’s not that every visit turns into a sci‑fi DNA consultation; often, it’s just another lab test that quietly informs decision‑making. You still see trial and error, but less blind guessing. There’s a risk of overpromising – genes are only one piece of the puzzle – but as data piles up, the idea of prescribing powerful drugs without at least considering someone’s biological individuality is starting to feel old‑fashioned.
9. Digital Health and Remote Monitoring: The Clinic in Your Pocket

You can roll your eyes at yet another health app, but some digital tools are genuinely changing how care is delivered, especially for chronic conditions. Wearables can continuously track heart rate, rhythm, sleep, and activity, and some smartwatches are now cleared to detect irregular heart rhythms like atrial fibrillation. For someone at risk of sudden arrhythmias, a device on the wrist that quietly flags a dangerous pattern can literally be life‑saving. Blood pressure cuffs, glucose sensors, and even spirometers are connecting to phones and sending data directly to clinics, turning snapshots into ongoing stories.
Telemedicine, which exploded during the pandemic, has stuck around as a normal part of care. Follow‑up visits, mental health check‑ins, medication adjustments – these can now happen from a kitchen table instead of a waiting room chair. For people living far from specialists or juggling multiple jobs or caregiving responsibilities, that’s not a minor convenience; it’s the difference between getting care and skipping it. Of course, this all raises issues about data security, equity, and the digital divide, but the trend is clear: more of medicine is coming to where people actually live their lives, instead of forcing everyone into the same fluorescent‑lit exam room.
10. Mental Health Innovations: Faster Relief and Less Stigma

Mental health has gone from whispered side note to front‑page concern, and the innovations reflect that shift. Newer fast‑acting antidepressant options based on ketamine‑like compounds have given hope to people with severe, treatment‑resistant depression who didn’t respond to traditional medications. In controlled, supervised settings, some of these treatments can relieve symptoms within hours or days rather than the usual weeks, which matters enormously when someone is on the edge. Deep brain stimulation and transcranial magnetic stimulation are offering non‑drug options for certain patients who’ve tried everything else.
At the same time, digital mental health tools have made therapy and support more accessible, especially to younger people who might never set foot in a traditional clinic. Apps offering guided cognitive‑behavioral techniques, text‑based counseling, and crisis support are far from perfect, but for many they’re the first, crucial step away from isolation. The cultural shift might be just as important as the technical one: it’s increasingly normal to talk about anxiety, burnout, trauma, and medication without immediate judgment. For a field that was neglected for so long, seeing real investment, better science, and more honest conversation feels like a breakthrough in its own right.
A New Baseline for What’s Possible

Looking across these breakthroughs, a pattern emerges: medicine is moving from blunt to precise, from reactive to proactive, and from “live with it” to “maybe we can fix this.” Gene editing, AI diagnostics, mRNA platforms, regenerative therapies, and digital tools are not abstract concepts; they’re already reshaping daily life for people with sickle cell disease, cancer, obesity, HIV, heart problems, depression, and more. At the same time, they raise hard questions about fairness, access, privacy, and what it even means to be healthy when so much can be measured, predicted, and tweaked.
If there’s one grounding thought, it’s this: the gap between what’s scientifically possible and what’s actually available is now the real battleground. The science is racing ahead; policy, ethics, and equity are scrambling to catch up. Ten years from now, many of today’s miracles may feel routine, and new ones will have taken their place. The uncomfortable question, and maybe the most important one, is this: when the next breakthrough arrives, will it reach everyone who needs it – or only the few who can afford to stand closest to the future?