Imagine swallowing a pill that has literally no active ingredient, then watching your pain melt away, your sleep improve, or your blood pressure drop. It sounds like a trick, but it’s one of the most deeply studied and strangely powerful phenomena in medicine: the placebo effect. The idea that belief itself can change the body used to sound like fringe thinking. Today, it sits right at the center of how we test new drugs, understand pain, and even rethink what “real” treatment means.
The placebo effect isn’t magic, and it’s not simply “all in your head” in the dismissive sense people sometimes use. It’s your brain and body running a kind of internal pharmacy, mixing biochemistry with expectation, context, trust, and meaning. Once you start seeing how it works, you may never look at pills, doctors’ offices, or even your own symptoms the same way again.
The Strange Power of “Nothing”: What a Placebo Actually Is

At its core, a placebo is a treatment that looks real but doesn’t contain an active ingredient meant to directly affect the health condition being treated. Think sugar pills, saline injections, or fake surgeries where the skin is cut but no real procedure is done. On paper, they should do absolutely nothing. In real life, they sometimes trigger effects that rival actual medications, especially for pain, depression, anxiety, irritable bowel syndrome, and other symptom-heavy conditions.
What makes this so wild is that the benefit doesn’t come from the substance; it comes from the entire situation: the ritual of taking a pill, the authority of the doctor, the hope that this might finally work. The placebo isn’t the sugar pill itself, it’s the meaning wrapped around it. Once you see that, you realize medicine is never just chemistry – it’s also story, expectation, and trust.
Belief, Expectation, and the Brain’s “Inner Pharmacy”

When someone expects relief, their brain doesn’t just sit back and wait; it starts releasing its own powerful chemicals. In pain, for example, believing a pill will help can lead the brain to pump out endorphins and other neurotransmitters that act a lot like morphine. Brain imaging studies have shown changes in pain-processing areas when people respond to placebos, which means the effect is literally visible in the brain, not just subjective in the mind.
Something similar can happen with dopamine in movement disorders, or with stress hormones in anxiety and blood pressure. It’s as if expectation hands your brain a toolkit, and your brain decides to get to work. The body listens closely to what the mind predicts, like a nervous stage crew changing the lights and sound cues according to how it thinks the show should go.
The Clinical Setting: Why the White Coat and the Room Matter

The placebo effect doesn’t happen in a vacuum; it thrives in context. A confident doctor, a calm clinic, clean equipment, and a sense of ritual all feed into the brain’s calculation that “this is real treatment.” When the environment looks serious and professional, the brain leans toward expecting improvement, and that expectation itself can start shifting symptoms. Even the color and size of pills can influence how strong people think they are.
On the flip side, a rushed appointment, a distracted provider, or cold, confusing communication can blunt or even undermine that same effect. It’s like the difference between watching a movie in a gorgeous theater with great sound versus on a cracked phone with bad speakers. The story might be identical, but how your brain responds feels completely different. The setting amplifies or muffles the placebo effect in powerful ways.
Placebo vs Nocebo: How Expectations Can Harm, Too

The placebo effect has a darker twin called the nocebo effect. Just as positive expectations can ease symptoms, negative expectations can actually make them worse. If someone is told a drug has a long list of nasty side effects, they’re more likely to report some of those effects even if they’re secretly given a placebo. The mind can amplify discomfort, trigger headaches, tighten muscles, and raise anxiety simply because it’s bracing for something bad.
This isn’t about people “faking it”; it’s the nervous system reacting to perceived threat. Pain might sharpen, nausea might appear, fatigue might deepen, not because of the pill itself, but because of what the person believes it will do. That’s why the way risks and side effects are explained really matters. Clear, honest information is essential, but the tone – fearful or calm, hopeless or hopeful – helps shape how the body reacts.
Open-Label Placebos: When Patients Know It’s a Sugar Pill
Here’s one of the most surprising twists: placebos can sometimes work even when people are told, openly, that they’re taking a placebo. In several clinical trials, patients with conditions like irritable bowel syndrome, chronic low back pain, or migraine were given pills clearly labeled as placebos and told that their bodies might still respond. Many of them reported real relief in symptoms compared to those who got nothing at all.
This “open-label placebo” idea shakes up the old belief that you have to deceive patients to get a placebo effect. It suggests that the ritual, the supportive explanation, and the possibility of benefit may be enough to kickstart the brain’s internal pharmacy, even when everyone knows there’s no active drug involved. It’s like going to a magic show while fully aware it’s all illusion, and still feeling amazed.
Ethics and Deception: Is Using Placebos Ever Okay in Practice?

For decades, placebos have raised tough ethical questions. Is it acceptable for a doctor to give a patient an inert pill and imply it’s a real treatment, just to harness the placebo effect? Many medical guidelines say no, because trust is fundamental in healthcare, and deliberate deception damages that trust. Patients need accurate information to make informed decisions about their own bodies.
That’s why the rise of open-label placebos is so interesting – it offers a possible middle ground. If you can be transparent about what a placebo is and still see benefit, you may preserve honesty while tapping into the mind–body connection. But even then, there’s debate about consent, expectation, and how much hope crosses the line into subtle pressure. The power of suggestion is real, and that makes it something to handle carefully, not casually.
Beyond Pills: Placebo Effects in Surgery, Devices, and Everyday Life
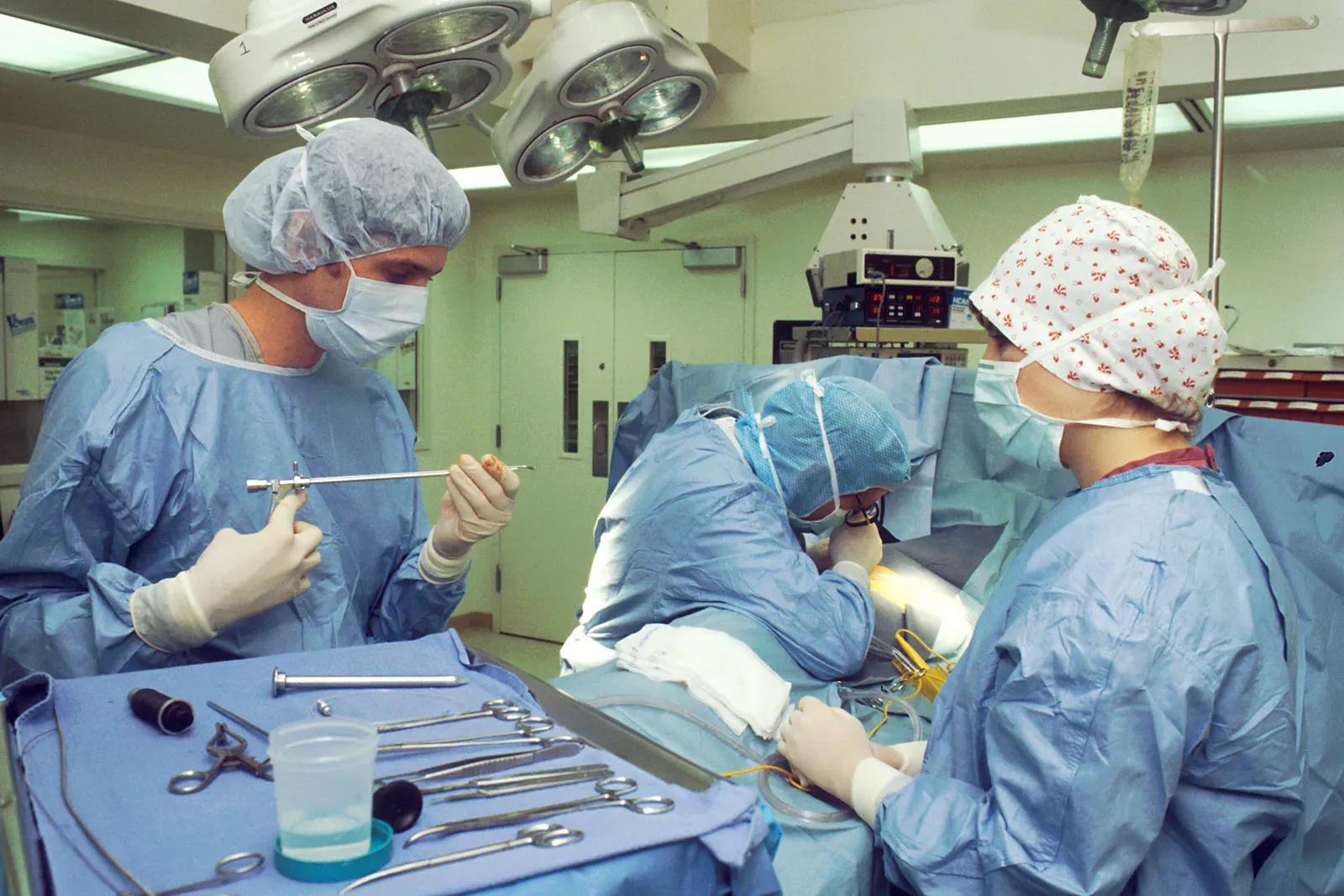
The placebo effect is not just about tablets. In some trials, people randomized to “sham surgery” (where incisions are made but the full procedure isn’t performed) showed improvements similar to those receiving the actual surgery for certain conditions, especially where pain and function are the main outcomes. The act of going under anesthesia, being wheeled into an operating room, and waking up stitched can send a powerful message to the brain that something serious has been fixed.
Even medical devices – like fake acupuncture needles that don’t pierce the skin, or machines that don’t actually deliver stimulation – can trigger strong placebo responses. And outside medicine, you can see softer versions everywhere: energy from a “lucky” object, confidence after a ritual, calm from a familiar routine. None of these are identical to a clinical placebo trial, but they rhyme with the same idea that meaning and expectation quietly sculpt our bodily experience.
What the Placebo Effect Teaches Us About Healing
Underneath all the weirdness, the placebo effect is a reminder that healing is not just about attacking a disease; it’s also about how safe, hopeful, and supported a person feels. It doesn’t cure infections, shrink tumors, or replace insulin, and it should never be used as an excuse to avoid real treatment. But for symptoms like pain, fatigue, nausea, or mood, the mind can sometimes nudge the body in a gentler direction than we once believed possible.
Personally, the more I’ve learned about placebo effects, the less I see them as “fake” and the more I see them as part of how humans are wired. The challenge is to respect that power without slipping into hype or dishonesty. Maybe the real question isn’t whether the mind can influence the body – it clearly can – but how we choose to use that knowledge. What possibilities does that open up in how you think about your own health?