Right now, trillions of microscopic organisms are living inside you, quietly making decisions that influence your mood, your energy, your immune defenses, and even your drive to exercise. You didn’t invite them. You can’t see them. Yet they may be running more of your biology than you ever imagined.
The gut microbiome, that vast internal universe of bacteria, fungi, and other microbes nestled in your digestive tract, has become one of the most electrifying frontiers in modern science. Researchers are discovering connections that feel almost impossible, links between your gut and your brain, your gut and your weight, your gut and your sleep. The deeper scientists look, the stranger and more fascinating it gets. So let’s dive in.
Your Gut Is More Than a Digestive Engine
Here’s the thing most people get wrong about the gut: they think it’s just a long tube that processes food. In reality, it’s something far more powerful. Your gut microbiome is made up of trillions of bacteria and other microbes living in your intestines, helping your body break down food, assisting your immune system, and sending chemical signals directly to your brain. Think of it less like a pipe and more like a city, teeming with activity, communication, and complex social dynamics.
The gut plays an obvious role in health by digesting what you eat and extracting nutrients, but there is a growing appreciation among scientists that your digestive system affects your general well-being in a much broader fashion. Honestly, once you start reading about what the gut microbiome actually does, it becomes hard to think of it as “just digestion” ever again.
The Gut-Brain Connection: Your Second Brain Is Speaking
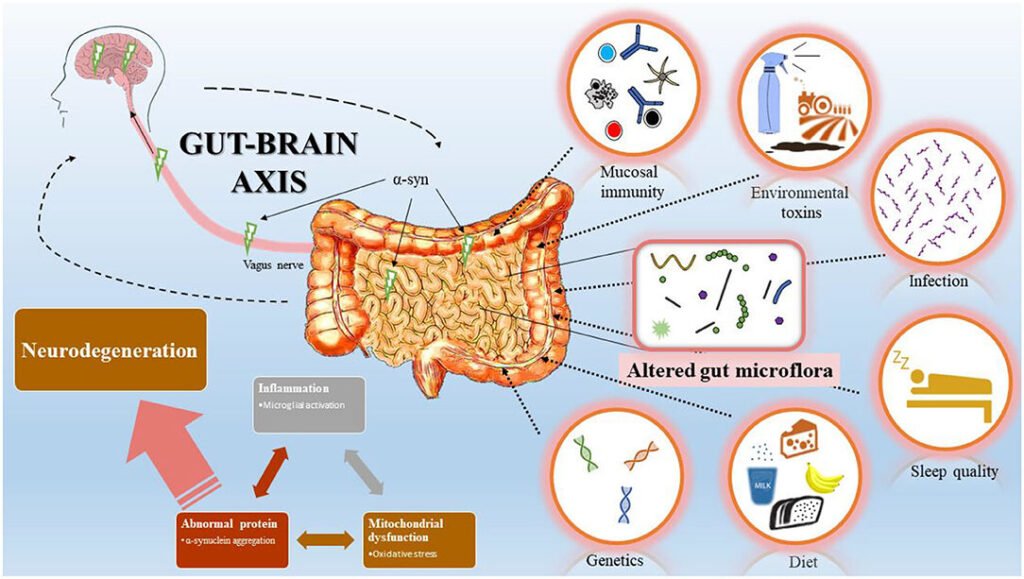
Did you know your gut contains more than 100 million neurons lining the digestive tract? That’s not a typo. One fascinating aspect of the gut’s widespread impact on health is its direct influence on and communication with the brain, a conduit known as the gut-brain axis, through direct signals from the vagus nerve as well as through molecules secreted into the bloodstream from gut microbes and immune cells. It’s a living telephone line running from your belly straight to your brain.
The human gut microbiome has emerged as a pivotal modulator of brain function and mental health, acting through intricate bidirectional communication along the gut-brain axis, with microbial communities influencing neurodevelopment, neurotransmission, and behavior via pathways involving the vagus nerve, immune signaling, and microbiota-derived metabolites. The wildest part? This relationship runs both ways. Psychological stress has been shown to impact the makeup of the gut microbiome, either indirectly through stressed people turning to comfort-food-heavy diets, or directly through molecular signals that travel from the brain to the gut and cause certain bacterial species to grow or die back.
Your Mood May Live in Your Gut, Not Just Your Head
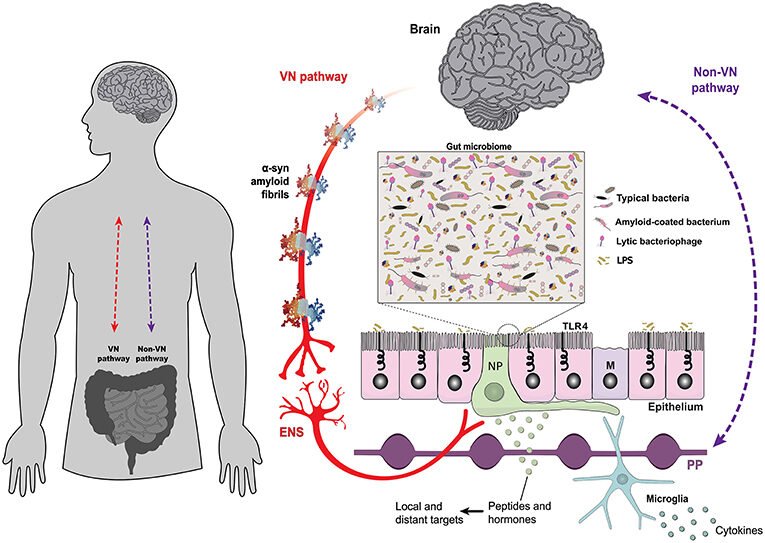
I know it sounds crazy, but your gut bacteria may have more to say about how you feel emotionally than your own thoughts do. A reduction in serotonin-producing microbes can negatively impact mood regulation, potentially contributing to the onset of depressive and anxious symptoms. When you consider that serotonin is often called the “feel-good” chemical, this connection suddenly feels very personal.
The effects on mood are thought to arise through several interconnected mechanisms: by enhancing gut barrier integrity and reducing leaky gut, by downregulating proinflammatory cytokine production and modulating immune responses, and by influencing the synthesis and availability of key neurotransmitters such as serotonin, dopamine, and GABA. It’s like your gut is running its own pharmacy. Gut dysbiosis affects the HPA axis, increasing cortisol production and perpetuating a cycle of chronic stress and inflammation. In other words, an imbalanced gut can make stress worse, which makes the gut worse, which makes stress worse still. A truly uncomfortable loop.
Immunity Starts in the Gut, Not in a Pill
Most people reach for a vitamin C supplement when they want to boost immunity. But the real powerhouse is sitting right in your intestines. The microbiome is essential for the induction, regulation, and function of both systemic and local immune responses, including innate and adaptive immunity, making the gut-immune-brain connection critical to overall health. Your microbiome is, in many ways, your immune system’s training ground.
Research indicates that gut bacteria produce metabolites, including short-chain fatty acids, which affect mucosal immunity, antigen presentation, and immune responses, thereby influencing cognitive functions. What’s more, the gut microbiota is considered an important biological barrier against viral infections and may serve as a promising target for adjuvant antiviral therapy. Recent research even found that a correlation exists between the severity of COVID-19 hospitalization and the fecal microbiome, with patients in severe conditions showing an enrichment of opportunistic pathogenic bacteria and a significant reduction in beneficial symbiotic bacteria.
Weight, Metabolism, and the Microbes Pulling the Strings
If you’ve ever tried everything to lose weight and wondered why it isn’t working, your gut microbiome might deserve a closer look. It turns out that gut microbiota is involved in metabolic health, such as blood glucose control and food intake behavior, explaining why not all people lose weight when they change their lifestyle, with scientists suggesting that an imbalanced gut microbiome composition and metabolites are causally involved in inappropriate food behaviors. Your gut bacteria, in a sense, can shape what you crave.
Research at the University of Utah recently identified a specific gut bacterium called Turicibacter with remarkable implications. Research identified Turicibacter as a type of gut bacteria that improves metabolic health and reduces weight gain in mice on a high-fat diet, with Turicibacter levels affected by how much fat the host eats, since the bacterium won’t grow if there’s too much fat in its environment. Meanwhile, the Western diet, characterized by excessive intake of processed foods, saturated animal fats, and refined sugars coupled with low fiber consumption, drives gut dysbiosis, with clinical evidence demonstrating significant reductions in microbial diversity and depletion of beneficial SCFA-producing taxa.
Sleep, Circadian Rhythms, and a Tired Microbiome

Here’s something your sleep tracker probably isn’t measuring: the health of your gut bacteria. The composition and diversity of the gut microbiome is associated with sleep quality and duration in animal models and humans, with peptides released from bacterial growth interacting with receptors in the brain to trigger sleep-associated responses, while other microbial metabolites such as butyrate and those linked to melatonin synthesis can directly or indirectly influence sleep. Your gut is basically co-authoring your nightly sleep schedule.
A reciprocal relationship exists: while disrupted sleep patterns can disturb the gut microbiota and lead to dysbiosis and subsequent health implications, an imbalance in the microbiome can also exacerbate sleep issues, perpetuating a detrimental cycle, highlighting the criticality of a balanced gut microbiome to overall health. It’s hard to say for sure which comes first, the bad sleep or the bad microbiome, but one feeds the other in a relentlessly circular way. These findings highlight the intricate relationship between diet, the gut microbiome, and sleep, suggesting the potential for microbiome-targeted interventions to improve sleep health.
How You Can Actually Support Your Gut Microbiome

Let’s be real, all of this is only useful if you can actually do something about it. The good news is that your microbiome is remarkably responsive to the choices you make daily. Interventions to improve gut microbiota include dietary changes, probiotics and prebiotics supplementation, careful antibiotic use, and lifestyle changes like exercise and stress management, with these strategies enhancing both gut and brain health and promoting overall physical and mental well-being. You don’t need expensive supplements to get started.
The Mediterranean diet synergizes olive oil polyphenols with complex carbohydrates, elevating Bifidobacterium abundance and reducing inflammatory markers such as C-reactive protein and interleukin-6. On the flip side, research found that 141 common drugs altered the microbiome of samples, and even short-term treatments created enduring changes, entirely wiping out some microbial species. So being thoughtful about medications, especially unnecessary antibiotics, matters just as much as eating well. Prebiotics, which are non-digestible substrates selectively chosen to target host microorganisms enabling beneficial microbes to thrive, can be found in a wide variety of foods including fruit, vegetables, whole grains, and human milk.
Conclusion: The Universe You’re Already Carrying
What’s striking about the gut microbiome is how profoundly it defies the old idea that our bodies are just our own. You are, in a very real sense, a walking ecosystem. Your mood, your sleep, your immune resilience, your body weight, and even your motivation to get off the couch all have a gut-level connection. Science in 2026 is only beginning to map the full extent of that territory.
The discoveries of recent years have strengthened the foundation for a more mechanistic, clinically meaningful understanding of the gut microbiome, with studies across metabolic health, gastrointestinal disease, and neurogastroenterology highlighting the microbiome’s central role in shaping health and guiding future therapeutic innovation. The most empowering takeaway here is simple: the way you eat, sleep, move, and manage stress isn’t just about calories or steps counted. It’s about tending to an inner world that, in turn, tends to you.
So, knowing all of this, which part of your daily life do you think your gut microbiome might be influencing the most? It might be worth thinking about.