Imagine waking up in ten years and realizing that hospitals feel almost unrecognizable. Checkups happen in your living room, doctors use algorithms as confidently as stethoscopes, and incurable diseases from your childhood are now routine to manage – or even prevent. That future isn’t sci‑fi anymore; it’s quietly being built in labs, startups, and clinics around the world right now.
Some of the most powerful technologies in human history are finally colliding with medicine, and the impact could be as dramatic as the invention of antibiotics or vaccines. Not every promise will come true, and there will definitely be missteps, but the direction of travel is clear: health care is shifting from reactive and one‑size‑fits‑all to predictive, personalized, and always‑on. Let’s dig into five breakthroughs that could genuinely reshape how long – and how well – we live.
1. AI‑Powered Diagnostics and Clinical Decision Support
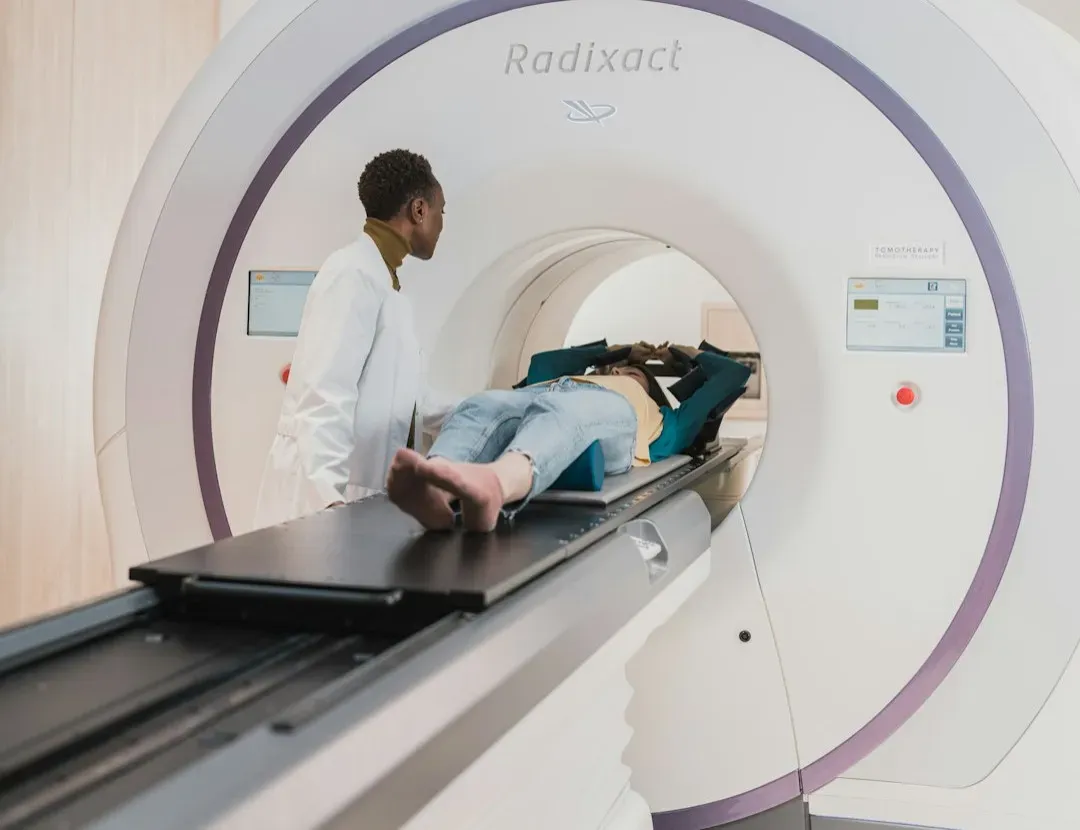
The idea that software can spot disease better than a trained specialist sounds outrageous until you look at what’s already happening. Deep learning systems can now detect diabetic eye disease, certain skin cancers, and early lung abnormalities in imaging scans with accuracy that rivals, and in some cases slightly surpasses, human experts. In hospitals, AI tools are being tested to flag sepsis hours earlier than usual, to read ECGs in seconds, and to predict who is at risk of sudden deterioration long before visible symptoms appear.
What makes AI so disruptive is not just accuracy, but scale and speed. A radiologist can read a limited number of scans a day; an algorithm can screen thousands without getting tired, distracted, or emotionally drained. That doesn’t mean doctors become irrelevant – in reality, they become more like pilots using sophisticated autopilot systems, still fully responsible but supported by constant, data‑driven guidance. There’s a catch, though: biased training data, black‑box models, and overconfident use can genuinely harm patients if we’re careless. My own skeptical side thinks the biggest revolution won’t be “doctor replaced by AI,” but “doctor plus AI outperforms everything we used to accept as normal care.”
2. Gene Editing and Curative Genetic Therapies
There’s something almost unsettling about being able to edit the code of life itself, but that’s exactly what modern gene editing tools allow. Technologies like CRISPR have moved from experimental curiosity to real treatments, with the first gene‑editing therapies for conditions like sickle cell disease and certain blood disorders already approved or in late‑stage trials. Instead of managing symptoms forever, these approaches aim to tackle the root genetic cause once, then let the body run on the corrected instructions.
If this approach scales, it could completely flip the logic of chronic disease care. Think about inherited blindness, muscular dystrophy, or some forms of high cholesterol: these are conditions where just one faulty gene can wreak havoc over a lifetime. Editing or replacing that gene is like fixing the software bug instead of constantly rebooting the system and hoping for the best. I find it both thrilling and a bit terrifying, because the line between therapy and enhancement could blur quickly, and mistakes at the DNA level aren’t as easy to roll back as a bad app update. But for families living with genetic diseases today, this isn’t an abstract ethical puzzle; it’s a chance at a normal life that once felt impossible.
3. Personalized Medicine Driven by Big Data and Omics

For decades, medicine has been oddly generic: people with the same diagnosis get more or less the same drug at the same dose, even though bodies obviously don’t behave like identical machines. Now, as it gets easier and cheaper to read genomes, track proteins, and map the chemistry in our blood and tissues, that blunt approach starts to look almost primitive. Personalized medicine uses this ocean of data – genomics, proteomics, metabolomics, and more – to tailor treatments to the unique biology of each person.
You can already see this happening in oncology, where tumors are analyzed for specific mutations to decide which targeted drug, or combination, might actually work. Cardiology, psychiatry, and auto‑immune diseases are following the same path, where your genetic variants, lifestyle factors, and even microbiome can influence which therapy gives you the best odds with the fewest side effects. It reminds me of moving from buying a “small, medium, or large” T‑shirt to getting one custom‑fitted: once you’ve tried the tailored version, the old system feels lazy. The risk, of course, is that access may skew toward wealthier patients and well‑resourced health systems unless we’re very deliberate about making these tools widely available, not just a luxury add‑on.
4. Regenerative Medicine, Stem Cells, and Lab‑Grown Organs
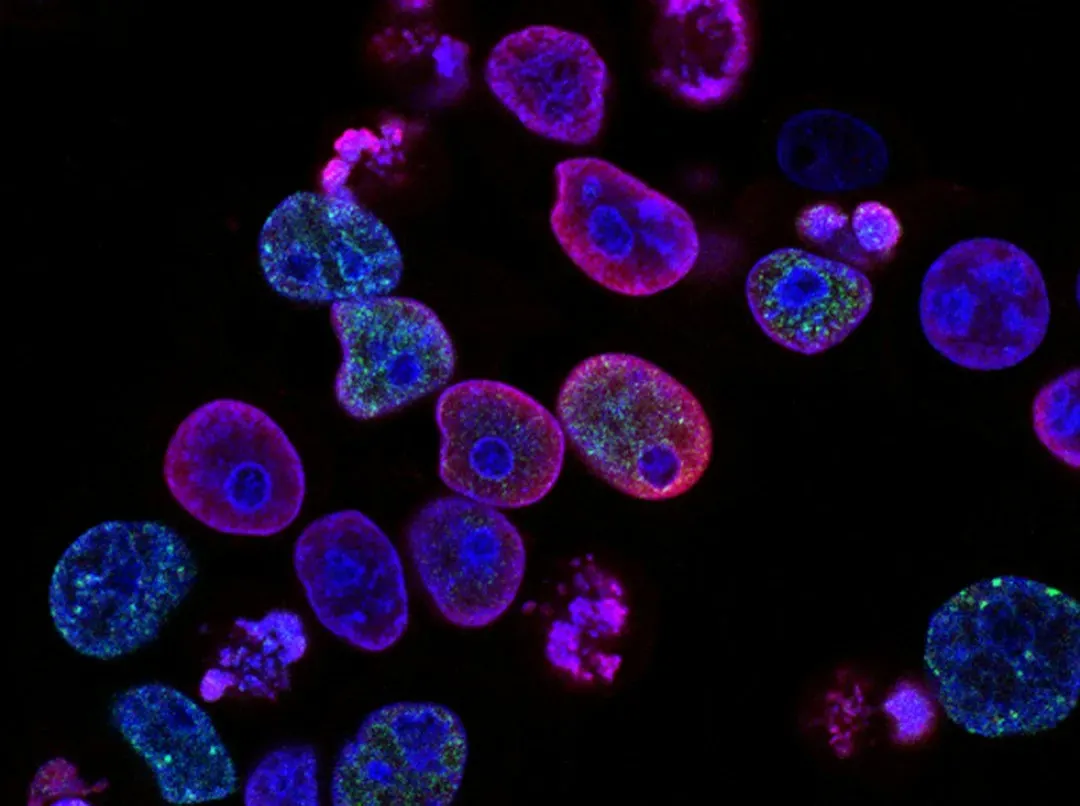
For most of medical history, damaged organs were basically a dead end: if your heart tissue or spinal cord was destroyed, there was only so much doctors could do. Regenerative medicine flips that script by trying to repair, replace, or even regrow what has been lost. Stem cell therapies are being tested for conditions like heart failure, Parkinson’s disease, and certain types of blindness, where injecting or coaxing new cells to develop could restore function that was written off as permanently gone.
At the same time, scientists are learning to grow miniature versions of organs – so‑called organoids – in the lab, and to print or bioengineer tissues that might one day serve as transplant material. Imagine reducing the brutal waiting lists for donor kidneys or livers by growing compatible tissue from a patient’s own cells, dramatically lowering both rejection risk and the need for lifelong immune suppression. When I first read about lab‑grown organ patches for damaged hearts, it sounded like science fiction fan service, yet animal studies show real promise. The journey from petri dish to routine surgery is long and messy, but if even a portion of this field matures, our idea of what is “irreversible” injury could change completely.
5. Continuous Health Monitoring and Digital Twins of the Human Body

We’ve already normalized wearing devices that count steps and measure heart rate, but that’s just the warm‑up act. The next wave of health tech is moving toward continuous, multi‑sensor monitoring: wearables that track blood pressure, heart rhythm, glucose levels, sleep stages, breathing, and maybe even early signs of infection around the clock. Instead of a few data points from an annual physical, your health record could become a high‑resolution, living timeline that reveals subtle shifts long before they turn into crises.
Layered on top of that is a more futuristic idea: the digital twin. In this concept, your data – medical history, imaging, lab tests, genetics, and real‑time sensor feeds – feed into a virtual model of your body or specific organs. Doctors and algorithms could then test “what if” scenarios on the twin before touching the real you: What if we increase this medication? What if we change your exercise routine? I like to think of it as having a high‑fidelity flight simulator for each patient, reducing guesswork and trial‑and‑error. It does raise big questions about data privacy and who controls these detailed models of our bodies, but if handled well, the payoff could be fewer surprises, fewer emergency admissions, and care that finally feels anticipatory instead of constantly playing catch‑up.
Conclusion: A Future of Health We Actually Want to Live In

Looking across these five technologies, a pattern emerges: we’re moving from seeing the body as something we patch up occasionally, to a system we can continuously understand, predict, and intentionally reshape. AI makes sense of complexity at a scale no human can manage, gene editing rewrites faulty instructions, personalized medicine tailors our treatments, regenerative techniques repair what was once lost, and always‑on monitoring lets us spot trouble while it’s still a whisper instead of a scream. None of these advances is guaranteed to deliver on all of its promises, and each comes with its own ethical and social knots we’ll have to untangle in real time.
Still, it’s hard not to feel a cautious kind of optimism when you step back and see the whole picture. If we choose carefully – prioritizing equity, privacy, and real patient benefit over hype and profit – this next era of medicine could mean not just longer lives, but healthier, more independent ones. Maybe the most radical shift won’t be the technologies themselves, but the way they let us think differently about illness, aging, and what’s possible for our bodies. When you imagine your own health ten or twenty years from now, which of these revolutions would you most want by your side?