You have probably cut your finger, watched it close up in a few days, and moved on without giving it a second thought. Routine. Unremarkable. Except, honestly, it is anything but. What just happened inside your skin was a perfectly orchestrated biological performance involving hundreds of cellular actors, chemical signals, and repair mechanisms that have been refined over billions of years of evolution.
We tend to hand over our trust to pharmaceuticals and medical procedures, sometimes forgetting that the body was already running an astonishing internal repair operation long before the first drug was ever invented. Science is now catching up, and what researchers are discovering in labs around the world is nothing short of jaw-dropping. Let’s dive in.
The Ancient Blueprint: Your Body’s Built-In Repair System
Think of your body as a city that never goes offline. The moment damage occurs, a response team is dispatched. The human self-healing power refers to the ability of an organism to restore health through self-repair mechanisms when subjected to external damage or internal dysfunction, and this concept has a solid biological foundation in medicine. This isn’t poetic metaphor. It is hardwired biology.
At a microscopic level, when skin tissue is damaged, platelets quickly aggregate to form clots for hemostasis, followed by macrophages clearing necrotic tissue and fibroblasts secreting collagen for repair, ultimately leading to epidermal cell regeneration and completion of healing. This precise repair mechanism is a valuable legacy from billions of years of biological evolution. You didn’t earn it, you inherited it from every ancestor who ever survived a wound.
Self-healing is the main bridge between treatment and health. It goes beyond traditional medicine, from back-end disease treatment models to front-end disease prevention and health promotion, and evokes an individual’s power of self-recovery. That shift in framing alone is enormous for how we think about wellness.
Inflammation: The Misunderstood Hero of Healing
Inflammation has an image problem. Most people hear the word and think of swelling, pain, and something to be suppressed as fast as possible. Here’s the thing though: inflammation is actually your body’s first and most critical defense move. When the body is injured or encounters harmful pathogens, the first response is often inflammation. This process involves white blood cells rushing to the affected area, triggering the release of chemical signals that enhance blood flow and create a barricade against invaders. While inflammation can sometimes be uncomfortable, it’s a vital part of the healing process.
The cellular and molecular mechanisms underpinning tissue repair and its failure to heal are still poorly understood, and current therapies are limited. Poor wound healing after trauma, surgery, acute illness, or chronic disease conditions affects millions of people worldwide each year and is the consequence of poorly regulated elements of the healthy tissue repair response, including inflammation, angiogenesis, matrix deposition, and cell recruitment. So the real problem is not inflammation itself, but when it misfires or stays switched on too long.
The Liver’s Extraordinary Superpower
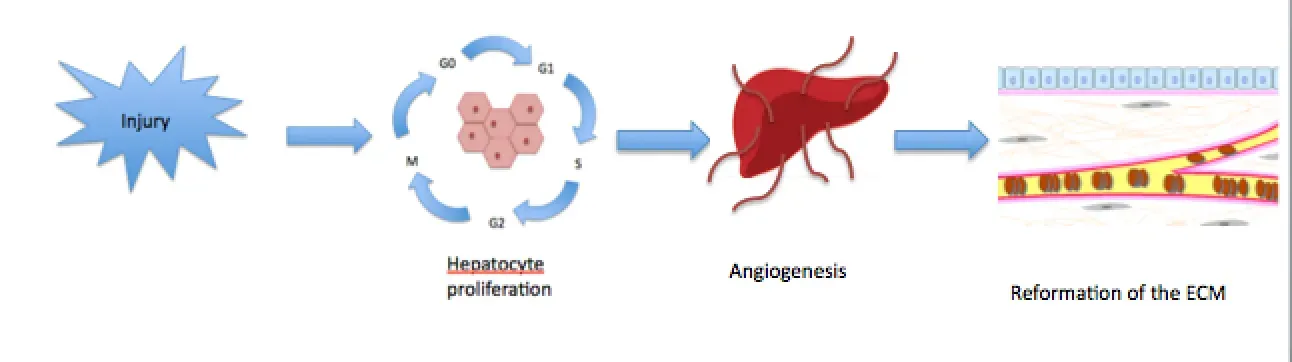
Of all the organs in your body, the liver may be the most quietly extraordinary. It can regenerate itself in a way no other organ can, and scientists are only now beginning to fully understand why. The liver is the only human organ in which differentiated cells, cells that have become fully specialized to perform specific tasks in a specific tissue type, can proliferate. In other organs, once cells become differentiated, they stop being able to divide and proliferate. Without a stem cell reserve or the ability to return to a proliferative state, these tissues have no options for regeneration.
This is why if a person suffers injury to part of their heart, or brain, the organ can’t replace the missing cells. But if a person injures part of their liver, some of the liver cells begin to proliferate, dividing and generating replacement liver. That difference right there is the reason liver transplant science looks so radically different from cardiac care. Researchers like Whitehead Institute Fellow Kristin Knouse are working to decode exactly what gives the liver this edge, hoping to one day extend that capability to other organs.
Stem Cells: The Body’s Wildcards
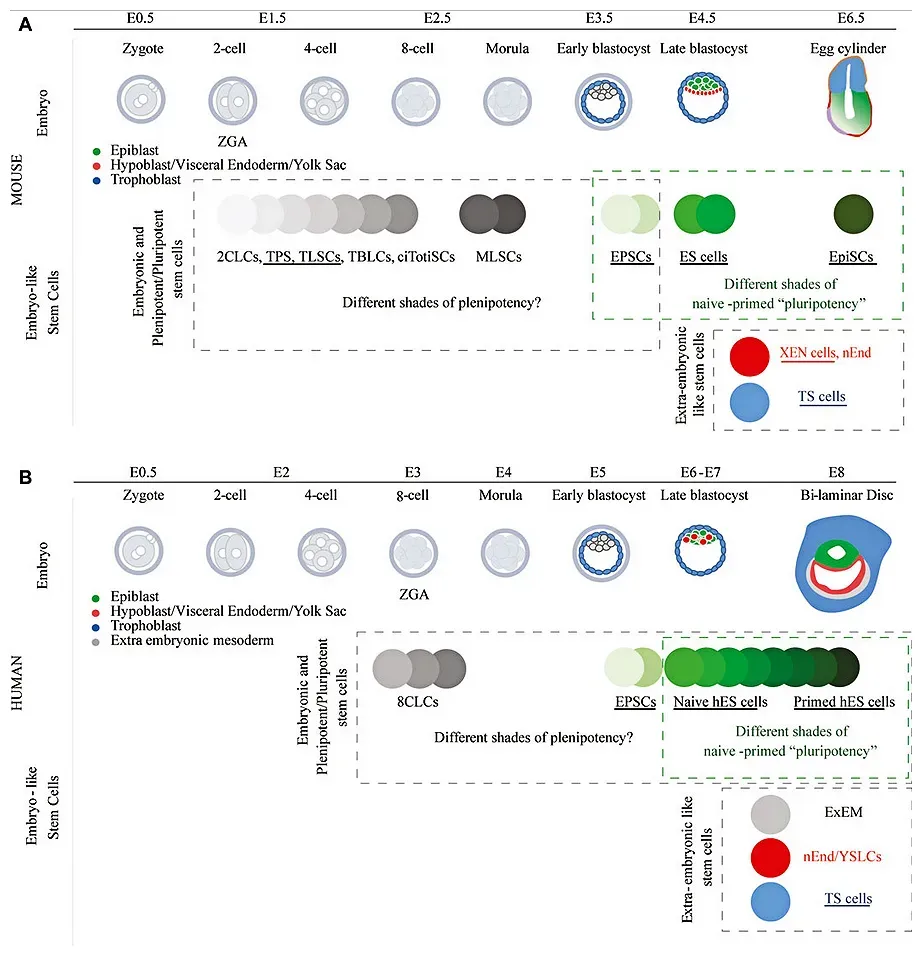
Anyone who’s healed from a cut or a scrape has witnessed the incredible regenerative power of stem cells. These cells can create identical copies of themselves, creating new cells and tissues that replace damaged ones. Stem cells are active in some areas of our body throughout our lives, like the skin and blood. They are, in the simplest terms, your body’s reserve workforce.
In many critical organs, including the heart and kidneys, stem cells are absent. When such tissues are damaged due to aging, injury or disease, they don’t regenerate, leading to devastating health consequences. USC researchers are at the forefront of an emerging field called “clinical regenerative medicine,” which taps stem cells’ restorative powers to tackle some of the hardest-to-treat diseases, ranging from heart failure to blindness. It’s a field still in its early chapters, but the momentum behind it is striking. As the body ages, stem cells are less efficient at regenerating the cells and tissues that make up skin, bone or muscle. Researchers are studying whether old stem cells can be made as effective as young stem cells, and how the regenerative power of stem cells can be harnessed in treatments. The aim is to one day transplant stem cells to rebuild muscle, whether after injury or as a consequence of disease such as muscular dystrophies.
The Mind-Body Connection: Your Brain Is Healing You Right Now

I know it sounds crazy, but your brain may be one of the most powerful healing instruments your body has. The placebo effect is not just a psychological illusion – it is a biological reality that highlights the brain’s capacity to regulate healing, pain, immunity, and mood. That sentence deserves a moment to land. Decades of dismissing the placebo as a nuisance in drug trials have given way to something far more interesting.
The placebo effect can influence the autonomic nervous system, altering heart rate, blood pressure, and immune function. Placebo treatments have been shown to reduce inflammation by triggering the release of anti-inflammatory molecules such as cortisol. These effects are mediated through conditioned responses and learned associations, where the body responds to the expectation of relief or healing as if an active treatment were administered. Thus, placebo effects can lead to genuine, organic changes in the body, driven largely by neurobiological processes involving the brain’s reward, pain, and stress regulatory systems. Your thoughts, quite literally, change your biology.
The Brain-Immune Axis: Expectation as Medicine
Taking the mind-body connection even further, cutting-edge research is revealing that your brain can actually train your immune system. A study published in Nature Medicine found that increasing activity in a deep-brain region can boost the immune system’s response to vaccines – and people can be trained to do it themselves using the power of brain scans and positive thinking. The findings could help explain the so-called placebo effect. Think about that. Your reward circuitry, activated by positive expectation, can amplify how strongly your body defends itself.
In people, the brain’s reward circuitry becomes active when we anticipate recovering from depression or banishing pain, as brain imaging has shown. That circuitry then activates neurons that wend their way from the brain to organs, including those of the immune system. Expecting to recover from infection or illness triggers an immune response that makes expectation reality. This is not wishful thinking. This is neuroscience. There are several lines of research suggesting that our mental perception of the world constantly informs and guides our immune system in a way that makes us better able to respond to future threats.
Sleep: The Night Shift Your Body Can’t Skip

Here is something that should make you reconsider your late-night scrolling habits. Sleep isn’t just rest. It is an active, biological repair session that your body absolutely depends on. Sleep is required to consolidate memories, regenerate tissue, and build up energy for emotional regulation and alertness during the day. Sleep deprivation disrupts these processes, increases stress, and predisposes people to heart, psychiatric and neurological problems. Every hour you shave off is an hour your cellular maintenance crew can’t finish the job.
Sleep and circadian rhythms regulate various aspects of human physiology and behavior, including memory, attention, hormone balance, immunity, and metabolism. Compromised sleep quality and quantity, as well as misalignment of sleep and circadian rhythms with the external environment, have been implicated in an increased risk of various chronic diseases, including cognitive impairment, cardiometabolic disorders, and mental disorders. Think of your sleep schedule the same way you’d think about charging your phone. Miss a night and things still work. Miss many, and everything starts to break down faster than you expect.
Your Gut Microbiome: A Hidden Healing Army

Honestly, the gut microbiome research of the last decade reads like science fiction. The trillions of microorganisms living in your digestive system are not just helping you digest food. They are also quietly influencing your bones, your immune system, your sleep, and potentially your ability to heal from injury. Researchers at the CU Anschutz School of Medicine say microorganisms living in the gut may hold the key to improving symptoms of osteoarthritis, help heal stubborn fractures, and more.
A growing body of evidence has revealed a compelling relationship between gut microbiota composition and musculoskeletal injury recovery, highlighting its potential as a novel therapeutic target. Musculoskeletal injuries, including fractures, post-traumatic osteoarthritis, and tendon or ligament injuries, commonly lead to changes in the community structure of the gut microbiota, intestinal permeability, and systemic inflammation, processes known to negatively influence tissue repair. It’s as though an injury in your knee sends ripples all the way down to your gut, and what lives in your gut sends signals back about how well you’ll recover. A more diverse microbiome is generally correlated with increased sleep efficiency and total sleep time – which, as you now know, is tied to healing in its own right.
The New Frontier: Science Supercharging Your Natural Healing
Science is no longer just studying your body’s healing powers. It is beginning to amplify them. NSF-powered researchers at the University of California, San Francisco have engineered molecules that act like “cellular glue,” allowing them to direct in precise fashion how cells bond with each other. The engineered cells contain customized adhesion molecules that bind with specific partner cells in predictable ways to form complex multicellular ensembles. The implication of this? Regrowing tissue, healing wounds, and potentially regrowing nerves on demand.
A study from the Weizmann Institute of Science, published in Nature Communications, reveals that the very enzymes responsible for cellular destruction – caspases – may also render certain cells resistant to death, enabling damaged tissue not only to regenerate but even to become more resilient. Unfortunately, this same mechanism may be hijacked by many types of cancer and may help explain why some tumors recur in a more aggressive and treatment-resistant form. The new findings could open avenues for therapies that speed up wound repair and help prevent cancer relapse. Researchers are also exploring electromagnetic fields and vibrations as healing tools. The possibility of using physical energies to boost regenerative processes has been strongly suggested by the ability of electromagnetic fields and mechanical vibrations to drive efficient in situ reprogramming of the differentiating and regenerative potential of our endogenous stem cells. Your body, it turns out, responds to far more than just pills.
Conclusion

Your body has been doing something remarkable every single day of your life, often without your awareness or credit. From the split-second clotting response when you nick your finger, to the nightly cellular maintenance during sleep, to the quiet microbiome army shaping how your bones heal, you are walking around in one of the most sophisticated self-repair systems ever produced by nature.
Science is no longer just observing these powers from a distance. It is learning to speak the body’s own language, to amplify, redirect, and unlock healing capacities that most of us never knew existed. The exciting truth is that we are still in the early chapters of this story. Breakthroughs in stem cell research, gut microbiome medicine, neuro-immune science, and regenerative technologies are rewriting what it means to heal.
The real question isn’t whether your body can heal. The evidence shows it wants to, it’s designed to. The question worth sitting with is: what are you doing in your daily life to support the process or work against it? What surprised you most about the healing powers already living inside you?




