If you could shrink down and walk through your own body during a flu or stomach bug, you’d witness something that looks more like a sci‑fi war movie than everyday biology. Cells sending distress signals, chemical alarms blaring, microscopic “soldiers” swarming to the front lines – it’s loud and chaotic, but astonishingly well organized. We tend to think of feeling sick as our body failing, but in many ways, those miserable days on the couch are a sign the system is actually doing its job.
I still remember the first time a doctor told me that my fever was not the enemy, but part of the cure. It felt so backwards: I was shivering, exhausted, and he calmly explained that this was my body cranking up the heat to make life harder for invading microbes. That idea – that our symptoms are often part of an unseen strategy – changes how you see almost every sniffle and sore throat. Let’s pull back the curtain on what’s really happening when your body fights illness.
The First Line: Skin, Mucus, and Other Unsung Bodyguards

Before any dramatic immune “battle” begins, your body relies on the simplest, quietest defense of all: keeping things out. Your skin is not just a covering; it’s a tough, slightly acidic, constantly renewing barrier that blocks most bacteria, viruses, and fungi from ever getting in. Tiny natural oils and sweat on your skin create an environment that’s surprisingly hostile to many germs, even though you never feel it.
At every opening – your nose, mouth, eyes, and gut – your body adds another layer of defense. Sticky mucus in your nose and airways traps inhaled particles and microbes like flypaper, while tiny hair‑like structures called cilia sweep that mucus out. In your stomach, powerful acid and digestive enzymes break down not just food, but many would‑be invaders. Most of the time, illness never even starts because these quiet barriers do their job so well you don’t notice.
The Rapid Response Team: Innate Immunity Jumps In
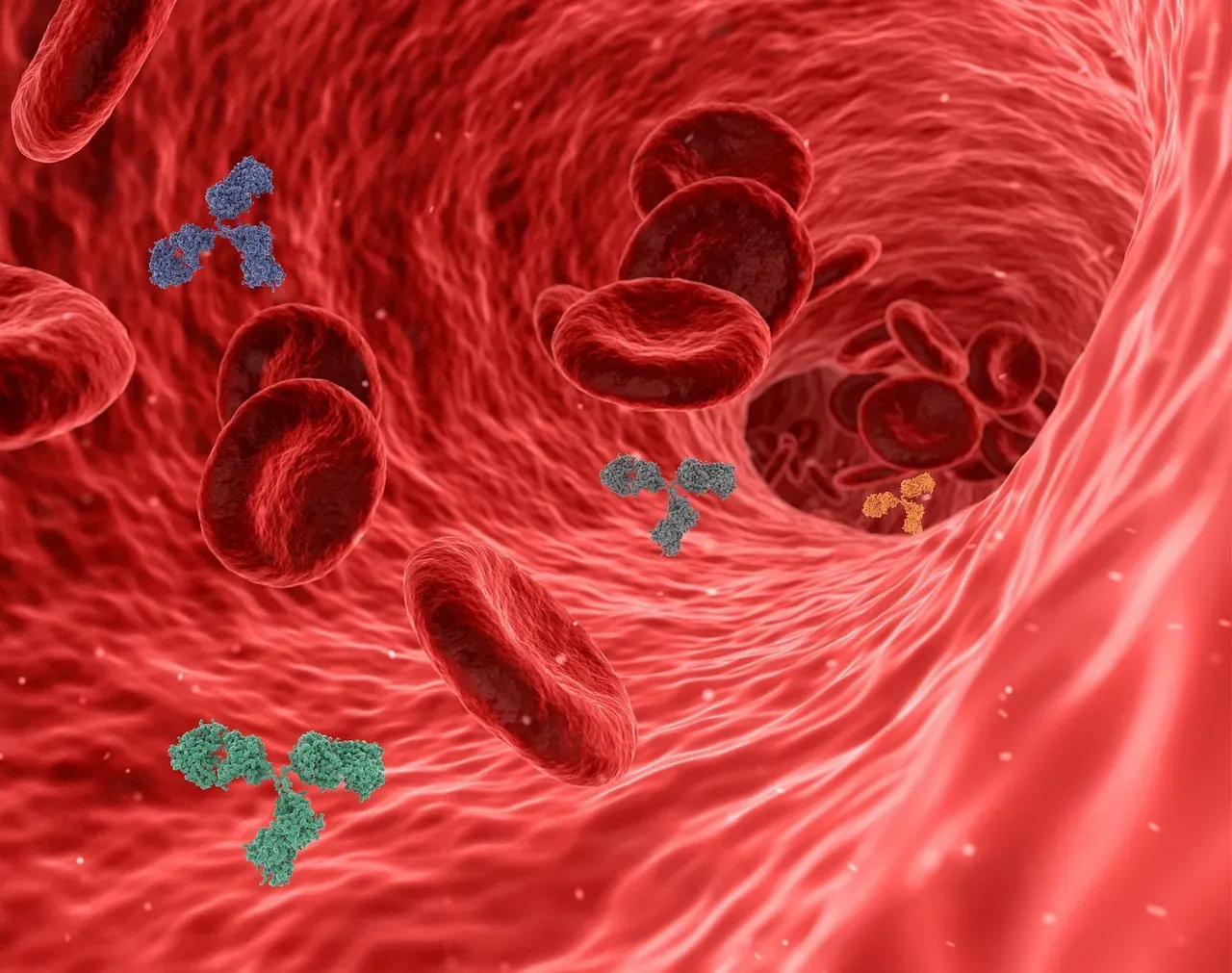
When something does slip past the barriers – say, a flu virus or bacteria in a small cut – your innate immune system is the first to respond. This system is ancient and fast, a bit like a neighborhood watch that doesn’t bother with sophisticated background checks: if something looks suspicious, it reacts. Cells like macrophages and neutrophils patrol tissues, looking for patterns that are common on microbes but not on your own cells.
Once these cells detect trouble, they move in aggressively. Macrophages “eat” invaders and dead cells, breaking them down inside themselves, while neutrophils can release toxic chemicals that kill bacteria but also damage nearby tissue. That damage is partly why an infected area becomes red, swollen, and painful. From the outside it feels like everything is going wrong, but on the inside, this is your body buying time and containing the threat before it spreads too far.
The Chemical Alarm: Inflammation and Fever Explained
Inflammation often has a bad reputation, but in the context of an infection, it’s basically your body pulling the fire alarm. When immune cells notice invaders or tissue damage, they release signaling molecules that tell nearby blood vessels to open wider and become a little leaky. That’s why an infected area can look red and puffy: more blood is rushing in, bringing extra immune cells and nutrients needed for repair.
On a whole‑body level, those same signals can reach your brain and reset your internal thermostat, leading to a fever. Higher body temperature can slow down the growth of some viruses and bacteria and makes your immune cells work more efficiently, like turning up the heat in a workshop so the tools perform better. The chills and body aches feel awful, but they’re part of a coordinated response to tilt the odds in your favor. It’s uncomfortable, but it’s not random or pointless.
The Elite Forces: Adaptive Immunity Learns the Enemy
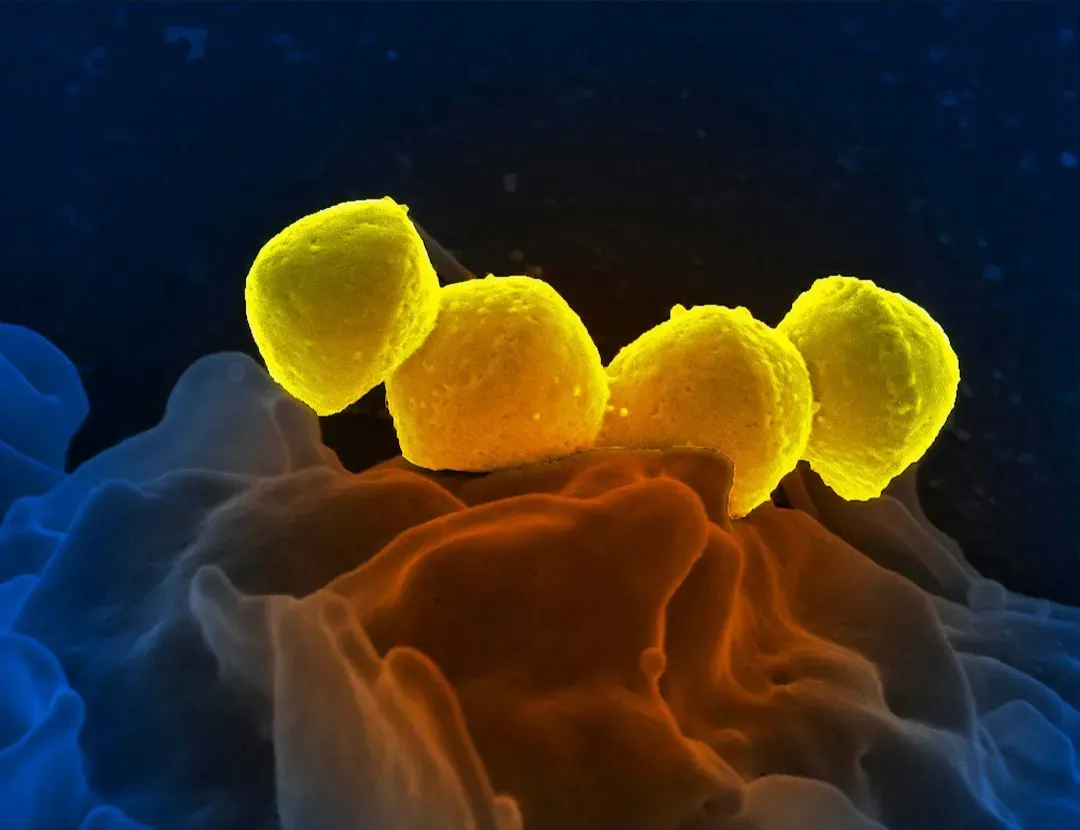
If the innate system is your quick‑and‑dirty neighborhood watch, the adaptive immune system is more like a specialized intelligence agency. It doesn’t just attack; it studies each invader and builds a custom response. Two main types of white blood cells lead the way here: B cells, which make antibodies, and T cells, which can coordinate attacks or directly kill infected cells.
B cells produce antibodies that recognize very specific shapes on a virus or bacterium, like a key fitting a particular lock. Once those antibodies are circulating, they can neutralize viruses by coating them so they can’t enter your cells, or mark bacteria for destruction by other immune cells. T cells, meanwhile, check the “ID badges” that all your cells constantly display on their surface; if a badge shows evidence of a virus hiding inside, certain T cells can destroy that cell before the virus multiplies further. This takes a little longer to ramp up than the innate response, which is why you don’t feel better instantly, but once it kicks in, it can be incredibly precise and powerful.
Memory Cells: How Your Body Remembers Past Battles
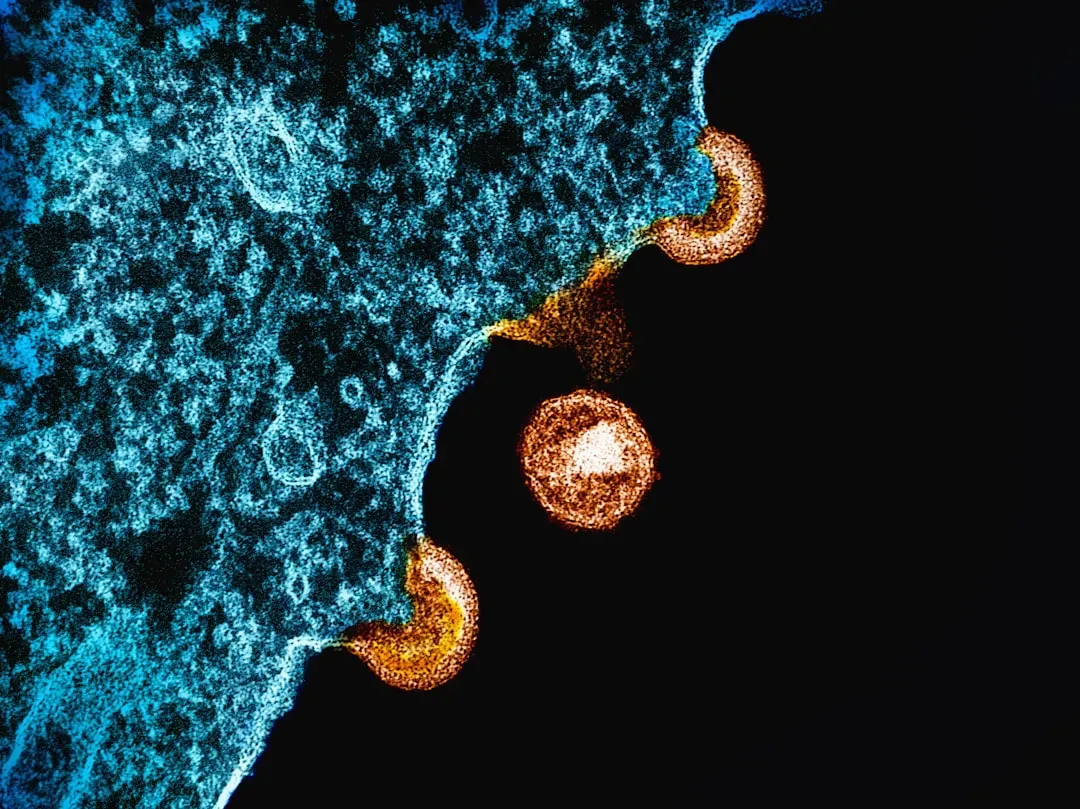
One of the most astonishing features of the adaptive immune system is its memory. After you’ve fought off an infection, some of your B cells and T cells don’t retire; they stick around as memory cells, almost like veterans who keep their training sharp. If the same germ tries to invade again, these cells recognize it much faster than the first time and can launch a response before you even realize anything is happening.
This is exactly the principle behind vaccines: your body is safely introduced to a weakened or partial version of a germ so that it can train memory cells without you having to endure the full‑blown disease. That’s why, for many infections, people either don’t get sick again or have a much milder illness the next time. It’s like having your own personalized defense manual filed away, ready to be pulled out at the first sign of a familiar enemy trying to sneak back in.
Friendly Microbes: Your Microbiome as a Hidden Ally
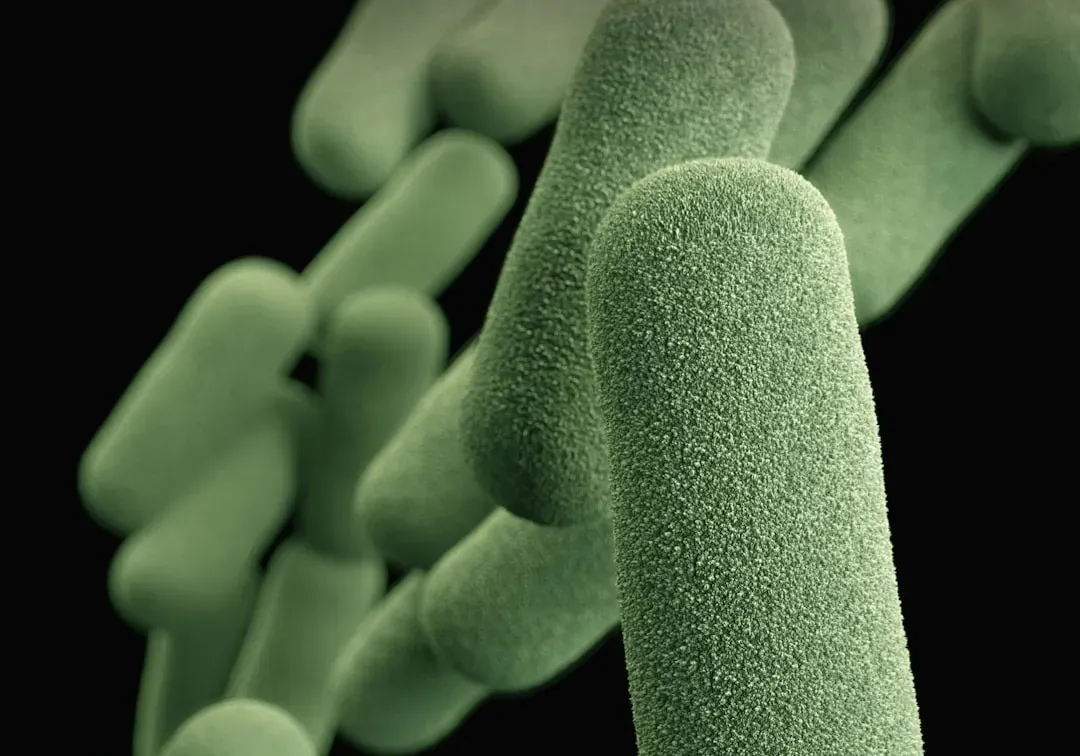
It’s easy to think of microbes only as germs, but a huge number of them are actually on your side. The bacteria, fungi, and other tiny organisms that live in your gut, on your skin, and in other parts of your body form what we now call the microbiome. In a healthy state, they crowd out harmful microbes, compete for resources, and even produce substances that keep would‑be invaders in check. It’s a bit like having a protective crowd that makes it hard for troublemakers to get close.
In your intestines especially, these friendly microbes help train the immune system to react strongly to real threats while staying calm around harmless food particles and normal bacteria. When the balance of the microbiome is disrupted – for example by repeated antibiotic use, poor diet, or certain illnesses – your immune responses can become confused or more easily overwhelmed. Paying attention to things like fiber‑rich foods, sufficient sleep, and stress management may seem simple, but they genuinely support this invisible community that quietly supports you in return.
When Defenses Misfire: Autoimmunity and Allergies
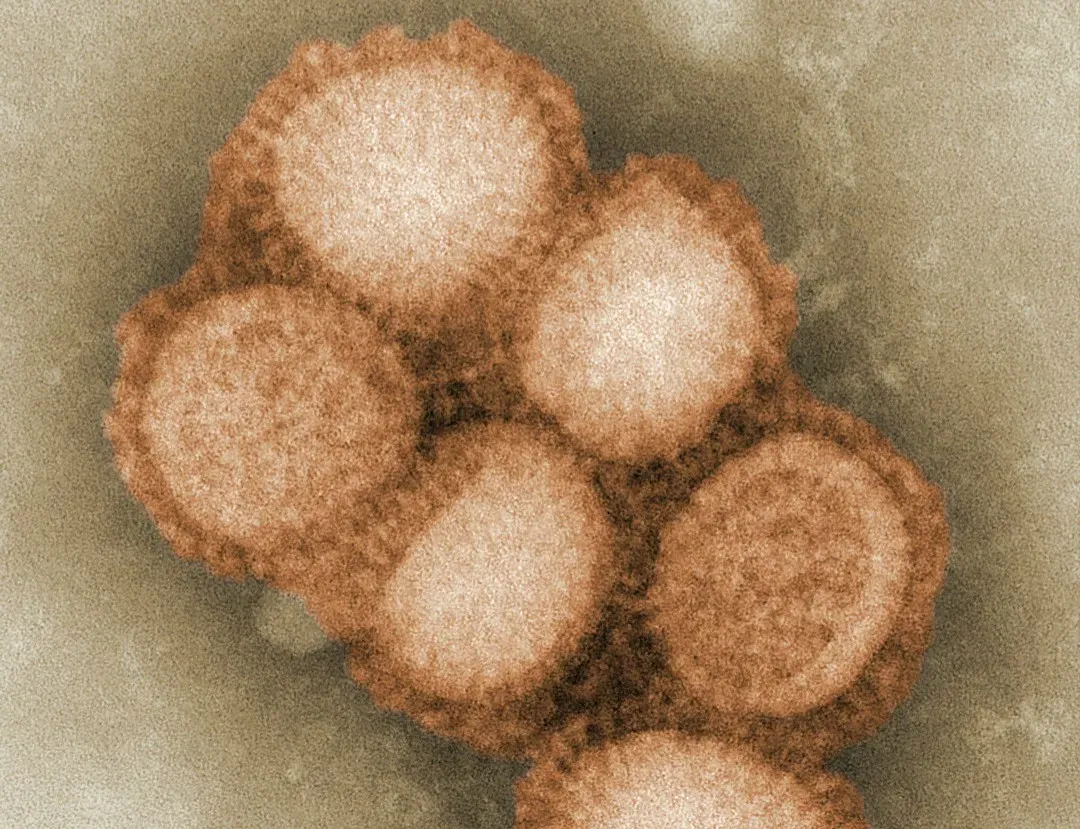
For all its sophistication, the immune system is not perfect, and sometimes its power turns against you. In autoimmune diseases, immune cells start treating parts of your own body as if they were foreign invaders. This can lead to chronic inflammation and damage in joints, skin, nerves, or organs, depending on the specific condition. It’s as if the security system got its friend‑or‑foe settings wrong and started attacking the building it was meant to protect.
Allergies are another kind of misfire, where the immune system overreacts to harmless substances like pollen, peanuts, or pet dander. Instead of ignoring them, it mounts a dramatic response, releasing chemicals such as histamine that cause itching, swelling, sneezing, or even dangerous drops in blood pressure in severe reactions. These conditions can be frustrating and frightening, but they also reveal just how powerful the immune system is when it becomes misdirected. Understanding these misfires is helping researchers design better treatments that gently “retrain” defenses rather than just shutting them down.
Supporting the Unseen Battle: What Actually Helps Your Immunity

With all the marketing around “immune‑boosting” products, it’s easy to feel like you’re missing a magic pill. In reality, the basics that support your immune system are not flashy, but they’re surprisingly effective. Regular, moderate movement like walking, enough high‑quality sleep, and a varied diet with plenty of fruits, vegetables, and whole foods give your body the raw materials it needs to make immune cells, antibodies, and repair tissues. Think of it as keeping the army well fed, well rested, and properly equipped rather than just yelling at it to work harder.
Managing chronic stress is another crucial, often overlooked piece. Long‑term stress can keep certain stress hormones elevated, which over time may weaken parts of the immune response and increase inflammation in ways that make you more vulnerable to illness. Simple habits – brief breaks during the day, breathing exercises, time with people you trust, or even moments of quiet – can nudge your system back toward balance. You don’t have to be perfect; even small, consistent steps can make your body’s unseen battle a little less uphill.
The Quiet Miracle Happening Inside You
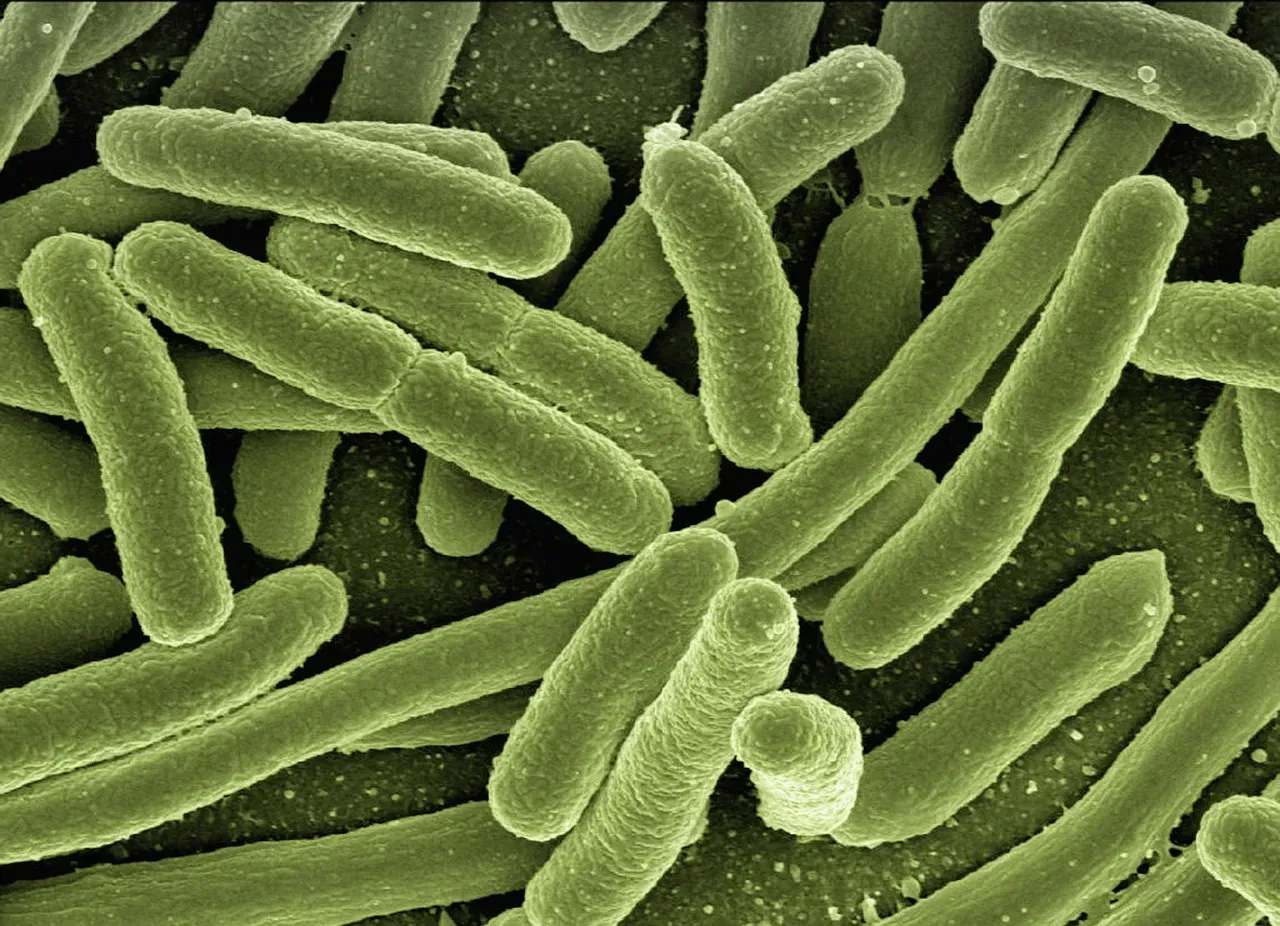
Every time you fight off a cough, recover from a stomach bug, or heal from a small cut, a complex, coordinated defense system has just saved your life on a tiny scale. From the simple shield of your skin to the highly trained memory cells that remember long‑gone infections, your body runs a twenty‑four‑seven security operation that you rarely notice until something goes wrong. Feeling sick is uncomfortable, but it’s also a reminder that your body is willing to throw everything it has into protecting you.
Next time you reach for a tissue or curl up under a blanket with a fever, it might help to picture the unseen battle you’re hosting – chaotic, yes, but also wildly impressive. You’re not just a passive victim of germs; you’re the home of an active, adaptive, learning defense network that has evolved over countless generations. Knowing that, does a simple sneeze feel a little more extraordinary now?




